Wisdom teeth are the last molars to appear, often between ages 17 and 25, and for many people in Kathmandu, they don’t have enough space to come in smoothly. That’s when you may notice pain at the very back of the mouth, swollen gums, bad breath, or jaw stiffness that comes and goes. Knowing which symptoms are normal “eruption discomfort” and which ones signal infection or impaction helps you decide when to book a visit and when to seek urgent care.
This guide walks you through wisdom tooth removal from start to finish: the common symptoms, how dentists confirm the problem with an exam and X-ray, what happens during surgery, and how many recovery days to plan for. You’ll also find a practical day-by-day healing timeline, food and aftercare rules that prevent dry socket, and red flags that mean you should contact your dentist right away. If you’re comparing clinics in Kathmandu, we’ll also cover what to ask about imaging, sedation, follow-ups, and cost so there are no surprises.
Wisdom Tooth Symptoms: What You Feel and What It Usually Means
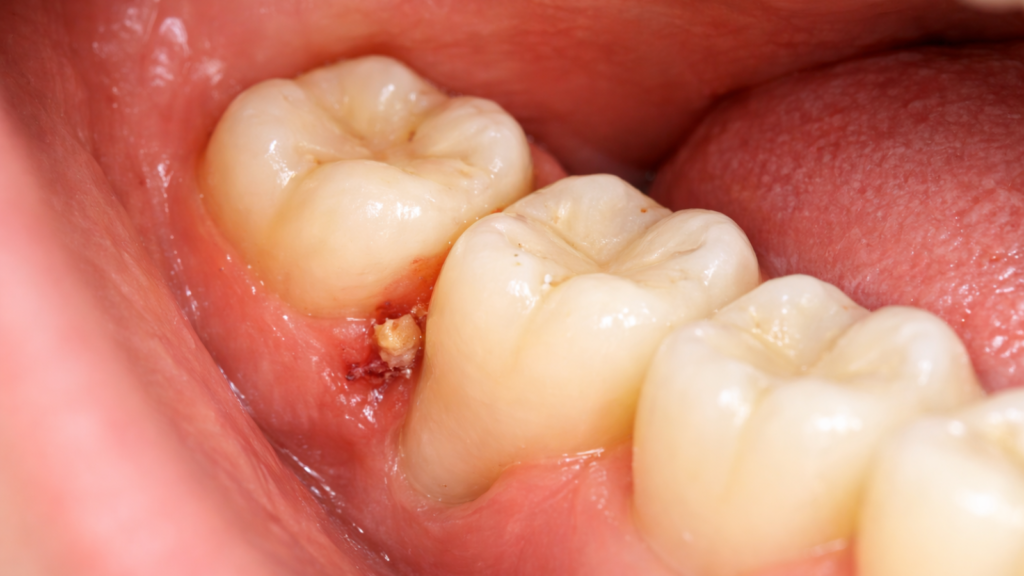
Wisdom tooth symptoms range from mild discomfort to severe pain that disrupts daily life. Most patients first notice pressure or soreness in the back gums between ages 17 and 25. The pain may come and go for weeks or months before becoming constant. Understanding the difference between normal eruption and serious complications helps you decide when to seek dental care.
Early eruption signs vs “this is getting worse” symptoms
- Normal eruption feels like mild pressure or soreness in the back gums that comes and goes over weeks. The area may feel slightly swollen, and you might notice the gum tissue stretching as the tooth pushes through. These early signs typically respond well to warm salt rinses and resolve as the tooth emerges fully.
- “This is getting worse” symptoms include persistent throbbing pain that wakes you at night, visible redness spreading beyond the immediate area, and difficulty opening the mouth fully. The pain stops responding to regular painkillers you take at home. These signs indicate complications like impaction or infection rather than normal eruption.
Pericoronitis (infected gum flap): symptoms, triggers, and why it keeps returning
Pericoronitis is an infection of the gum tissue (operculum) that partially covers an erupting wisdom tooth. The gum flap creates a pocket where food particles and bacteria accumulate, leading to inflammation and infection. Symptoms include sharp pain when biting down, a bad taste in the mouth, swollen gums that bleed easily, and sometimes visible pus around the affected tooth.
Common triggers include biting the swollen gum flap while chewing, poor oral hygiene in the back corners of the mouth, and upper wisdom teeth traumatizing the lower gum tissue. The infection keeps returning because the anatomical problem (the gum flap) remains unchanged. You clean the area and take antibiotics, but the flap continues to trap debris, and if left untreated, the surrounding tissue can develop into broader bleeding gums and gum disease. Removal of the wisdom tooth eliminates the recurring cycle permanently.
Warning signs that need urgent care: fever, facial swelling, trouble swallowing, trismus
You need same-day dental evaluation when wisdom tooth pain comes with fever above 100°F (37.8°C), visible facial swelling extending to the cheek or jaw, difficulty swallowing, or severe limitation in mouth opening (trismus). These symptoms indicate the infection is spreading beyond the tooth socket into surrounding tissue spaces.
Fever signals systemic involvement requiring antibiotics and possibly drainage. Facial swelling that crosses anatomical boundaries (from the jaw toward the eye or neck) suggests deep space infection. Trouble swallowing or breathing difficulty is a medical emergency because swelling can compress the airway. Trismus (inability to open the mouth more than 2 finger-widths) often accompanies severe pericoronitis or abscess formation.
Patients in Kathmandu should contact the clinic immediately when these signs appear rather than waiting for a scheduled appointment. The infection progresses rapidly once it involves facial spaces.
Safe short-term relief before your appointment (what helps vs what makes it worse)
Rinse gently with warm salt water (1 teaspoon salt in 1 cup lukewarm water) every 2 to 3 hours to keep the area clean without disturbing tissues. Take over-the-counter pain relievers like ibuprofen 400 milligrams every 6 to 8 hours with food, which reduces both pain and inflammation. Apply a cold compress externally on the cheek for 15 minutes on, 15 minutes off to control swelling.
Avoid poking the area with toothpicks, fingers, or hard-bristled brushes, which introduces more bacteria and damages inflamed tissue. Do not apply heat packs directly, as warmth can increase bacterial growth and swelling. Skip alcohol-based mouthwashes that sting and dry out the tissues. Never use aspirin directly on the gums, as it causes chemical burns rather than relief.
Why Wisdom Teeth Cause Problems (Impaction, Infection, Damage)
Wisdom teeth cause problems because modern human jaws are often too small to accommodate them. The third molars become impacted, meaning they cannot erupt properly into functional position. Impacted teeth trap food and bacteria, leading to recurring infections that antibiotics cannot permanently resolve. The anatomy itself creates the problem rather than poor oral hygiene alone.
Types of impaction (soft tissue vs bony) and how they affect pain and treatment
- Soft tissue impaction occurs when the wisdom tooth has erupted through bone but remains partially covered by gum tissue. The tooth crown is visible or palpable, but the gum flap (operculum) creates a trap for food and bacteria. Pain tends to be intermittent, triggered by chewing or food accumulation, and responds initially to cleaning and antibiotics. Surgical removal typically requires only gum incision and possibly minimal bone trimming.
- Bony impaction means the tooth remains fully or partially locked inside the jawbone, unable to erupt naturally. The tooth may be angled horizontally, tilted forward, or inverted. Pain is often chronic and dull rather than sharp because the tooth presses on bone and adjacent structures. Treatment requires bone removal to access the tooth, sectioning the crown and roots into pieces for extraction, and more extensive socket cleaning. Recovery from bony impaction takes longer (7 to 10 days) than soft tissue cases (3 to 5 days).
Food trapping and repeated infection cycles: why antibiotics alone don’t “solve it”
The anatomy of a partially erupted wisdom tooth creates a permanent food trap that cleaning cannot fully address. The gum flap and tilted position form a deep pocket where rice grains, meat fibers, and other particles lodge beyond the reach of the toothbrush or floss. Bacteria ferment this debris, causing inflammation and infection every few weeks or months.
Antibiotics kill the active bacteria and temporarily reduce symptoms, but the structural problem remains. The gum flap stays in place, the tooth angle does not change, and food continues accumulating. Patients return to the clinic every 2 to 3 months with the same complaint. Definitive treatment requires removing the tooth, which eliminates the pocket and stops the cycle permanently.
Damage to nearby teeth: cavities on the second molar and gum disease behind it
Impacted wisdom teeth commonly cause decay on the adjacent second molar, particularly on the back surface where cleaning is impossible. The wisdom tooth tilts forward and contacts the second molar at an angle, creating a narrow space that traps bacteria and food. Decay develops on both teeth over months to years, often unnoticed until pain appears.
Gum disease (periodontitis) develops behind the second molar because the wisdom tooth position prevents proper cleaning. The gum pocket deepens, bone loss progresses, and the second molar starts loosening. Patients who delay wisdom tooth removal sometimes lose both the wisdom tooth and the healthy second molar, requiring more complex and expensive treatment, including root canal therapy to save a compromised second molar before it is lost entirely. Removing the impacted tooth before damage occurs protects the second molar.
Upper vs lower wisdom teeth: why lower ones are tougher and recoveries can differ
- Lower wisdom teeth are embedded in denser bone (mandible) compared to upper teeth in the maxilla, requiring more force and time for extraction. The mandibular nerve and lingual nerve run close to lower wisdom tooth roots, creating risk for temporary or (rarely) permanent numbness. Surgical removal of lower impacted teeth typically involves bone drilling, tooth sectioning, and careful nerve avoidance.
- Upper wisdom teeth sit in softer bone and usually extract more easily, even when impacted. The maxillary sinus lies just above upper wisdom tooth roots, so infection or root displacement into the sinus are the main concerns rather than nerve injury. Recovery from upper wisdom tooth removal often involves less swelling and pain (2 to 4 days) compared to lower teeth (5 to 7 days or longer for difficult cases).
Patients should expect different recovery experiences when removing upper versus lower teeth, and surgeons in Kathmandu routinely discuss these differences during the consultation.
Do You Need Wisdom Tooth Removal? How Dentists Decide in Kathmandu
Not every wisdom tooth requires removal, and dentists in Kathmandu make removal decisions based on specific clinical criteria. The evaluation balances current symptoms against future risk of complications. Factors include impaction type, infection history, damage to adjacent teeth, and the patient’s ability to clean the area effectively. A thorough assessment prevents both unnecessary surgery and delayed treatment of problematic teeth.
When removal is recommended vs when monitoring is safe (clear decision factors)
- Removal is recommended when the wisdom tooth causes recurrent infection, damages adjacent teeth, remains partially erupted with a persistent gum flap, or shows bony impaction on X-ray with insufficient space to erupt. Dentists also remove wisdom teeth when orthodontic treatment requires space or when cysts develop around the impacted tooth crown.
- Monitoring is safe when the wisdom tooth has fully erupted, aligns properly with adjacent teeth, causes no symptoms, and can be cleaned effectively. Patients must demonstrate good oral hygiene and attend regular check-ups (every 6 months) so the dentist can detect problems early. Asymptomatic, fully buried wisdom teeth in patients over age 35 may also be monitored rather than removed, though this decision depends on individual risk factors.
The key distinction is functional eruption versus impaction. A tooth that erupts but cannot be cleaned properly still requires removal, even without current pain.
Pre-surgery assessment checklist: medical history, medicines, allergies, pregnancy, blood thinners
The dentist will ask about chronic diseases (diabetes, heart conditions, kidney problems, bleeding disorders), current medications, drug allergies, pregnancy status, and recent illnesses. Patients taking blood thinners (aspirin, warfarin, newer anticoagulants) must inform the dentist, as these medications increase bleeding risk and may need adjustment before surgery.
Diabetic patients require good blood sugar control (fasting below 126 milligrams per deciliter or 7.0 millimoles per liter) for proper healing. Pregnant patients typically postpone wisdom tooth surgery until after delivery unless infection threatens maternal health. Patients with heart valve disease or joint replacements may need antibiotics before the procedure to prevent infection.
Bring a complete list of medications, including herbal supplements and over-the-counter drugs. Disclose all allergies (penicillin, local anesthetics, latex) so the clinic can prepare alternatives. This information helps the surgeon plan safe anesthesia and post-operative medications.
X-rays for wisdom teeth (OPG) vs CBCT: when 3D imaging matters for nerve/sinus risk
Orthopantomogram (OPG) is the standard 2-dimensional panoramic X-ray that shows all teeth, jaw structure, and wisdom tooth position in a single image. OPG costs approximately Nepali Rupees (NPR) 800 to 1,200 in Kathmandu (80 to 120 United States dollars at current exchange rates) and provides sufficient information for most wisdom tooth extractions. The image reveals impaction angle, proximity to adjacent teeth, and general bone level.
Cone Beam Computed Tomography (CBCT) provides 3-dimensional imaging that precisely maps the position of the inferior alveolar nerve, lingual nerve, and maxillary sinus relative to wisdom tooth roots. CBCT costs NPR 4,000 to 6,000 (approximately 400 to 600 United States dollars) and is ordered when OPG shows the nerve canal running very close to or overlapping the tooth roots. The 3D view helps surgeons plan nerve-safe extraction techniques and discuss realistic numbness risks with patients.
Clinics in Kathmandu use CBCT selectively rather than routinely to balance diagnostic accuracy with cost.
Choosing a clinic in Kathmandu: what to confirm (sedation options, follow-up, emergency contact, itemized estimate)
Ask whether the clinic offers intravenous (IV) sedation or only local anesthesia for anxious patients or complex cases. Confirm the follow-up schedule (typically day 2, day 7, and day 14 after surgery) and whether follow-up visits are included in the quoted price or charged separately. Request a direct emergency contact number for after-hours complications like severe bleeding or suspected dry socket.
Obtain an itemized written estimate that separates consultation fees, X-rays, surgical removal charges, anesthesia costs, medications, and follow-up visits. Prices for wisdom tooth removal in Kathmandu typically range from NPR 5,000 to 8,000 (approximately 500 to 800 United States dollars) for simple extractions and NPR 12,000 to 20,000 (1,200 to 2,000 United States dollars) for surgical removal of impacted teeth. Sedation adds NPR 8,000 to 15,000 (800 to 1,500 United States dollars) depending on the type.
Verify the dentist’s credentials (Bachelor of Dental Surgery or Master of Dental Surgery specialization in oral surgery) and ask how many wisdom tooth surgeries they perform monthly. Experience matters significantly for difficult impactions.
Wisdom Tooth Surgery: What Happens on the Day (Step-by-Step)
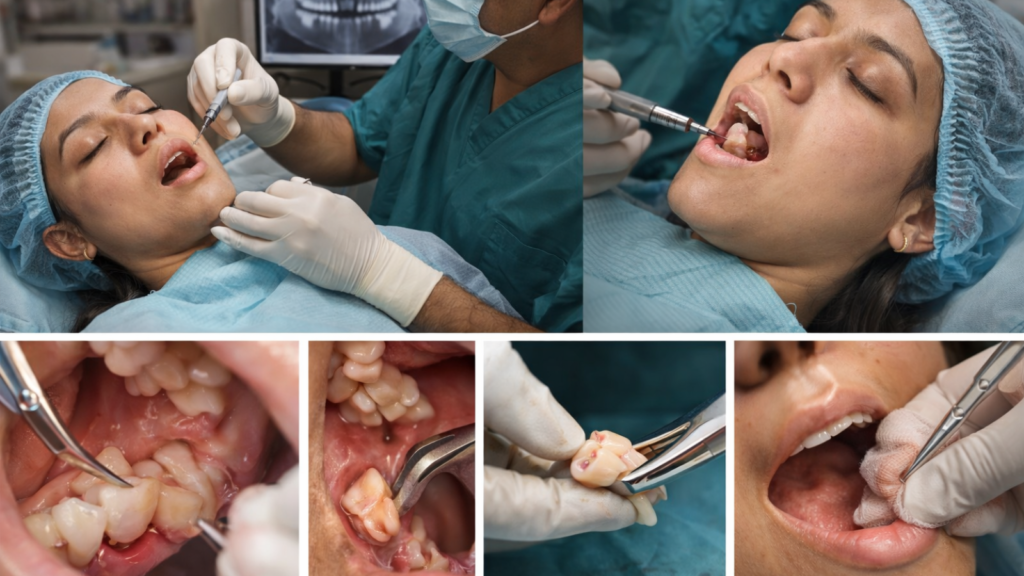
Understanding the surgical process reduces anxiety and helps patients prepare properly for the procedure. Wisdom tooth removal follows a systematic sequence from anesthesia through socket closure. The specific steps vary based on whether the tooth is fully erupted or deeply impacted in bone. Knowing what to expect during each phase allows patients to cooperate effectively and recognize normal sensations versus complications.
Anesthesia options: local vs sedation, what you’ll feel and how to prepare (fasting/escort)
Local anesthesia involves injecting numbing medication (lidocaine with epinephrine) around the wisdom tooth and adjacent tissues. You remain fully awake and aware during the procedure but feel no pain, only pressure and pushing sensations. The injection stings briefly (5 to 10 seconds), then numbness develops within 2 to 3 minutes. Local anesthesia requires no fasting and allows you to leave the clinic independently.
Intravenous (IV) sedation combines local anesthesia with medications (midazolam, propofol) that induce deep relaxation or light sleep. You feel drowsy, time passes quickly, and you remember little of the procedure. IV sedation requires fasting for 6 to 8 hours before surgery and an escort to take you home, as drowsiness persists for 2 to 4 hours. Patients who choose sedation must avoid driving, operating machinery, or making important decisions until the next day.
Discuss your anxiety level and medical history with the dentist to determine the safest, most comfortable option for your situation.
Surgical removal steps: incision, bone work, tooth sectioning, cleaning the socket
The surgeon makes a gum incision to expose the impacted tooth and underlying bone. Flap elevation reveals the tooth crown and roots. The surgeon uses a high-speed dental drill with sterile saline irrigation to remove bone covering the tooth, creating access to the crown and root surfaces. This step generates vibration and sound but no pain.
The tooth is sectioned (cut into 2 to 3 pieces) using the drill when it cannot be removed intact due to angulation or bone lock. The crown is removed first, then each root is elevated separately using specialized instruments. Sectioning reduces the force needed and minimizes trauma to surrounding bone and nerves.
The socket is thoroughly cleaned with saline irrigation to remove bone fragments, tooth particles, and bacteria. The surgeon inspects for root tips, smooths sharp bone edges, and packs the socket with gauze. The gum flap is repositioned and sutured closed with 2 to 4 stitches.
Immediately after surgery: gauze pressure, bleeding control, and the “first 60 minutes” rules
Bite firmly on the gauze pad placed over the extraction socket for 30 to 45 minutes without speaking, moving, or checking the area. Continuous pressure allows blood clot formation, which is essential for healing. Light oozing (pink-tinged saliva) is normal for 12 to 24 hours, but active bleeding should stop within the first hour.
The first 60 minutes rules are to avoid rinsing, spitting, or using straws, which create suction that dislodges the clot. Do not touch the surgical site with fingers or tongue. Keep the head elevated (sit upright or recline with extra pillows) rather than lying flat, which increases bleeding. Apply an ice pack externally on the cheek for 15 minutes on, 15 minutes off during the first 4 to 6 hours to control swelling.
Take the first dose of prescribed pain medication and antibiotics within this window, ideally before the numbness wears off completely.
Stitches and prescriptions: dissolvable vs removable sutures and what you’ll take home
Most clinics in Kathmandu use dissolvable sutures (polyglycolic acid or chromic gut) that fall out on their own within 7 to 10 days. These stitches soften and fragment as healing progresses, requiring no removal appointment. Some surgeons use non-dissolvable silk sutures that must be removed at the day 7 follow-up visit.
You will take home 3 to 4 medications: firstly, an antibiotic (typically amoxicillin 500 milligrams 3 times daily for 5 to 7 days or azithromycin for penicillin-allergic patients); secondly, a pain reliever (ibuprofen 400 milligrams or combination ibuprofen plus paracetamol); thirdly, an antiseptic mouthwash (chlorhexidine gluconate 0.12 percent or 0.2 percent solution for gentle rinsing starting day 2). Some prescriptions include a steroid (dexamethasone) to reduce swelling or a proton pump inhibitor if you have a sensitive stomach.
Follow dosing instructions exactly, complete the full antibiotic course even when you feel better, and avoid alcohol while taking medications.
Recovery Days After Wisdom Tooth Removal: Practical Timeline and Rules

Wisdom tooth removal recovery follows a predictable timeline that varies based on extraction complexity. Simple extractions heal faster (3 to 5 days) than surgical removal of impacted teeth (7 to 10 days or longer). Each recovery phase has specific care requirements and restrictions that protect the healing socket. Following the timeline prevents complications like dry socket, infection, and prolonged discomfort.
Day 0–1: protect the blood clot (no straw/spit), sleep position, and expected bleeding
The blood clot forming in the socket is the foundation for healing and must remain undisturbed. Avoid creating suction in the mouth by not using straws, not spitting forcefully, and not smoking (suction from inhaling dislodges the clot). Let saliva and blood drool passively into a tissue rather than spitting it out.
Sleep with the head elevated on 2 to 3 pillows to reduce blood flow to the surgical site and minimize swelling. Lying flat increases overnight bleeding and next-day facial swelling. Some patients sleep semi-reclined in a chair the first night for better elevation.
Expect pink-tinged saliva for 12 to 24 hours. Bright red bleeding that fills the mouth or soaks through a fresh gauze pad within 5 minutes indicates the clot has dislodged or did not form properly. Bite on a moistened tea bag (tannic acid promotes clotting) for 20 minutes. Contact the clinic immediately when bleeding does not slow after 2 attempts.
Days 2–3: swelling peak and jaw stiffness plan (ice first, then heat and gentle opening)
Facial swelling peaks on day 2 or day 3 after surgery and is proportional to the surgical difficulty. Simple extractions cause minimal swelling, while bony impaction removal can produce noticeable cheek enlargement and jaw stiffness. Swelling is a normal inflammatory response, not necessarily infection.
Continue ice packs externally for the first 48 hours (15 minutes on, 15 minutes off while awake). After 48 hours, switch to warm compresses (warm, damp towel held on the cheek for 20 minutes 3 to 4 times daily) to increase circulation and promote swelling resolution. The combination of ice first, then heat, produces the fastest recovery.
Jaw stiffness (trismus) makes opening the mouth difficult. Perform gentle jaw stretching exercises starting day 3: open the mouth slowly as wide as comfortable, hold 5 seconds, relax, and repeat 5 times every 2 to 3 hours. Gradual stretching restores normal opening within 5 to 7 days. If clicking or pain in the jaw joint persists well beyond the healing window, read about jaw pain, clicking, and TMJ causes to distinguish post-surgical stiffness from a separate joint issue.
What to eat by day: liquids/soft foods, when rice/solids usually return, what to avoid
Days 0 to 1 require a liquid or very soft diet: yogurt, smoothies (no straw), lukewarm soup (not hot), mashed potatoes, scrambled eggs, and protein shakes. Chew on the opposite side if only one tooth was removed. Avoid hot liquids that dissolve the clot, crunchy foods that can lodge in the socket, and acidic juices that sting the surgical site.
Days 2 to 4 allow semi-soft foods: dal-bhat with well-cooked vegetables, soft rice (not hard or sticky), noodles, boiled chicken, and ripe fruits like banana or papaya. Foods should require minimal chewing and not produce sharp particles. Continue avoiding hard, crunchy, or sticky items (nuts, chips, hard candies, gum).
Rice and normal solids usually return by days 5 to 7 for simple extractions and days 7 to 10 for surgical cases. Introduce foods gradually and stop anything that causes pain or gets stuck in the socket. Rinse gently after every meal starting day 2 to keep the area clean.
Days 4–7 to Week 2+: brushing/rinsing safely, back to work/school, exercise and travel timing
Start gentle brushing on day 2, carefully avoiding the surgical site itself but cleaning all other teeth normally. Brush the adjacent teeth very softly near the socket edge from day 4 onward. Beginning day 2, rinse gently with warm salt water or prescribed chlorhexidine mouthwash after each meal and before bed. Tilt the head to allow the rinse to flow over the area passively rather than swishing vigorously.
Patients with desk jobs usually return to work or school by days 3 to 5 after simple extractions and days 5 to 7 after surgical removals. Jobs requiring heavy lifting, bending, or physical exertion should wait until day 7 to 10, as strain increases bleeding and swelling. Students taking exams may wish to schedule surgery during breaks rather than immediately before important tests.
Avoid strenuous exercise, running, or gym workouts for 7 to 10 days, as increased heart rate raises blood pressure and can reopen the socket. Light walking is acceptable. Delay air travel for 5 to 7 days when possible, as cabin pressure changes can aggravate healing tissues. Patients traveling to high-altitude areas (Everest Base Camp, Annapurna Circuit) should postpone such trips for at least 2 weeks and confirm healing with their dentist.
Complications, Red Flags, and Wisdom Tooth Removal Cost in Kathmandu
Complications after wisdom tooth removal are relatively uncommon but require prompt recognition and treatment when they occur. Dry socket, infection, and nerve or sinus issues each present with distinctive symptom patterns. Knowing the warning signs helps patients distinguish normal post-operative discomfort from problems requiring dentist intervention. Early treatment of complications prevents prolonged pain and more serious consequences.
Dry socket: when it starts (often days 1–3), symptoms pattern, prevention, and treatment
Dry socket (alveolar osteitis) occurs when the blood clot dislodges or fails to form, exposing bare bone in the socket. It typically starts 1 to 3 days after extraction (peak incidence day 2) and presents as sudden, severe, throbbing pain that radiates to the ear or temple. The pain is much worse than the post-surgical discomfort you felt immediately after the procedure.
Patients describe a foul taste and bad breath (halitosis) due to bacterial activity on exposed bone. Looking in the mirror reveals a dry, empty socket with visible whitish bone rather than a dark blood clot. Dry socket is more common after lower wisdom tooth removal, in smokers, women taking oral contraceptives, and patients who failed to follow post-operative instructions.
Prevention involves firstly, avoiding smoking and tobacco use for at least 72 hours (ideally 1 week); secondly, not using straws or spitting; thirdly, following medication instructions; and fourthly, rinsing gently rather than vigorously. Treatment requires a return visit to the dentist, who irrigates the socket and places a medicated dressing (eugenol paste or iodoform gauze). The dressing soothes pain within hours and is replaced every 1 to 2 days until healing resumes (typically 5 to 7 days total).
Infection after extraction: signs you shouldn’t ignore and when antibiotics are needed
Post-extraction infection usually appears 3 to 5 days after surgery, past the initial healing phase. Warning signs include increasing pain instead of gradual improvement, fever above 100°F (37.8°C), foul-smelling pus draining from the socket, swelling that worsens or spreads to the face/neck, and red streaks on the skin near the jaw.
Infection develops when bacteria colonize the socket despite prophylactic antibiotics, often because the patient has diabetes, immune suppression, or poor oral hygiene. Some infections result from food particles trapped deep in the socket that were not cleaned out properly.
You need additional or different antibiotics when these signs appear. Contact the clinic immediately for re-evaluation, use this guide on tooth abscess danger signs and urgent treatment to understand when it’s an emergency. The dentist will drain any abscess, irrigate the socket, and prescribe a different antibiotic (often metronidazole added to amoxicillin or switching to clindamycin). Ignoring these signs risks deep space infection that requires hospitalization and intravenous antibiotics.
Numbness/nerve and sinus issues: what’s normal vs urgent (lower nerve / upper sinus)
Temporary numbness of the lower lip, chin, or tongue is relatively common after lower wisdom tooth removal due to proximity of the inferior alveolar nerve or lingual nerve. Numbness persists for days to weeks in approximately 5 percent of cases and usually resolves completely within 3 to 6 months. Permanent numbness is rare (less than 1 percent) and more likely when the nerve is directly injured during difficult extractions.
Tingling (paresthesia) or gradual return of sensation are positive signs of nerve recovery. Patients should report numbness lasting beyond 2 weeks so the dentist can assess and consider vitamin B complex supplements or referral to an oral surgeon for advanced evaluation.
Upper wisdom tooth complications include sinus exposure (a small hole connecting the socket and sinus) or root displacement into the sinus. Symptoms include air or fluid passing from the nose to the mouth when drinking, chronic sinus drainage, or sinus pressure/pain. Small sinus exposures (under 3 millimeters) often heal spontaneously with instructions to avoid nose blowing, sneezing with the mouth open, and using a decongestant. Larger openings or displaced roots require surgical closure or retrieval.
Cost factors in Kathmandu: simple vs surgical/impacted, imaging, sedation, and what to ask for in a quote
Simple (non-surgical) wisdom tooth extraction in Kathmandu costs approximately NPR 5,000 to 8,000 (500 to 800 United States dollars), including local anesthesia and basic follow-up. This applies to fully erupted teeth that can be removed with forceps and minimal bone work.
Surgical removal of impacted wisdom teeth ranges from NPR 12,000 to 20,000 (1,200 to 2,000 United States dollars) depending on impaction severity (soft tissue vs deep bony), surgical time, and bone removal required. Horizontal or deeply buried impactions fall on the higher end of this range.
Additional cost factors include firstly, panoramic X-ray (OPG) NPR 800 to 1,200 (80 to 120 United States dollars); secondly, CBCT scan NPR 4,000 to 6,000 (400 to 600 United States dollars) when nerve risk requires 3D imaging; thirdly, IV sedation NPR 8,000 to 15,000 (800 to 1,500 United States dollars); and fourthly, medications and follow-up visits, which some clinics include and others charge separately (NPR 500 to 1,000 or 50 to 100 United States dollars).
Ask for a written quote that specifies what is included (consultation, X-rays, anesthesia type, surgical fees, medications, post-operative visits) and what incurs extra charges (CBCT if needed, sedation upgrade, additional follow-up beyond the standard protocol). Verify whether the clinic offers installment payment plans or accepts insurance (many dental insurance policies in Nepal provide partial coverage for medically necessary extractions). For a broader view of what different procedures cost across specialties, dental in Kathmandu is a useful starting point for comparing services and pricing in one place. Understanding the total cost before treatment prevents surprises and allows proper financial planning.
How do I know if my wisdom tooth pain is serious?
Know your wisdom tooth pain is serious if you have fever over 100°F (37.8°C), facial swelling, difficulty swallowing, limited mouth opening, pus discharge, or pain spreading to your ear or throat, use this toothache relief guide: home remedies vs emergency dental care to decide what to do next. Pain that wakes you up or doesn’t respond to painkillers requires same-day dental evaluation.
Can I keep my wisdom teeth if they don’t hurt?
You can keep your wisdom teeth if they fully erupt, align properly, and can be cleaned well. Regular dental check-ups every 6 months are required, and this Kathmandu dental checkup price guide explains what affects cost (exam, X-rays, and add-ons). Painless but impacted teeth that trap food or harm nearby teeth still need removal despite no symptoms.
How long does wisdom tooth surgery take?
Wisdom tooth surgery takes 10–15 minutes for simple extractions and 30–45 minutes for impacted teeth. Removing all four takes 60–90 minutes including anesthesia. Complex cases with deep impaction or nerve proximity may take longer based on surgical difficulty.
Will I be awake during the procedure?
You remain awake under local anesthesia, which blocks pain but allows pressure sensation. IV sedation is available for deep relaxation or light sleep and requires fasting and an escort. Discuss your comfort level with your dentist to choose the best sedation option.
When can I eat rice and normal food after surgery?
You can eat soft rice and normal food by days 5 to 7 after simple extraction and days 7 to 10 after surgical removal. Start with liquids and very soft foods for 2 days, move to semi-soft by day 3, and avoid hard or sticky food until full healing.
What is dry socket and how do I prevent it?
Dry socket is a painful condition where the blood clot dislodges, exposing bone 1 to 3 days after surgery. Prevent it by avoiding smoking, spitting, and using straws. Follow post-op instructions. Smokers face higher risk and should stop for at least 72 hours after extraction.
How much does wisdom tooth removal cost in Kathmandu?
Wisdom tooth removal in Kathmandu costs NPR 5,000–8,000 for simple extractions and NPR 12,000–20,000 for surgical cases. X-rays cost NPR 800–1,200 and CBCT scans add NPR 4,000–6,000. IV sedation adds NPR 8,000–15,000. Always request a written quote detailing all charges.
Can I go to work the next day after wisdom tooth removal?
You should rest for 24–48 hours after wisdom tooth removal. Return to desk work by day 3 to 5 for simple cases and day 5 to 7 for surgical cases. Avoid heavy labor and speaking jobs until day 7 to 10. Plan around important work events.
What if I feel numbness in my lip or tongue after surgery?
Temporary numbness in your lip or tongue after lower wisdom tooth surgery affects about 5% of patients. It usually resolves within 3 to 6 months. Tingling means recovery is in progress. Report numbness lasting over 2 weeks to your dentist for evaluation and possible treatment.
Should I remove all 4 wisdom teeth at once or one at a time?
Removing all 4 wisdom teeth at once saves time, reduces cost, and allows one recovery period. Removing one at a time is better for anxious patients or those with medical issues. Choose based on your health, comfort, and schedule after discussing with your dentist.
BrightSmile Dental Clinic in Putalisadak offers comprehensive wisdom tooth evaluation and surgical removal with transparent pricing and patient-focused care. Contact us at +977-9748343015 or brightsmileclinic33@gmail.com to schedule your consultation and receive a detailed treatment estimate. Our team provides safe, comfortable extractions with clear recovery guidance and dedicated follow-up support throughout the healing process.
