Bad breath affects more than 25% of adults worldwide, yet most people struggle to identify the real source behind persistent odor. You might brush twice daily, use mouthwash religiously, and still notice that unpleasant smell returning hours later. The reality is that bad breath, medically known as halitosis, often stems from causes that go far beyond surface-level oral hygiene, and understanding the difference between occasional morning breath and chronic halitosis can save you months of frustration and ineffective solutions.
Persistent bad breath creates social anxiety, damages professional confidence, and signals underlying oral or systemic health issues you shouldn’t ignore. Whether you’re dealing with sulfurous odor that won’t fade, noticing white coating on your tongue, or experiencing bleeding gums alongside bad taste, this guide walks you through the scientific causes, accurate self-assessment methods, and evidence-based treatments that actually resolve halitosis at its source.
Bad Breath (Halitosis): Types, Triggers, and What’s Normal

Understanding the difference between normal morning breath and chronic halitosis starts with recognizing that temporary odor after sleep or eating garlic resolves within 30 minutes of brushing, while true halitosis persists throughout the day regardless of oral hygiene efforts. Halitosis divides into three main categories: physiological (from bacterial coating on your tongue, accounting for 85% of cases), pathological (from gum disease, infections, or systemic conditions), and pseudo-halitosis (where you perceive odor that clinical testing proves doesn’t exist).
Halitosis vs occasional bad breath: what counts as a real problem?
Occasional bad breath after eating garlic, waking up with morning breath, or noticing odor during fasting is physiologically normal and doesn’t qualify as halitosis. Your mouth produces less saliva during sleep, allowing bacteria to multiply and release volatile sulfur compounds (VSCs) that create temporary odor. This resolves quickly after brushing, eating breakfast, and resuming normal saliva flow.
Halitosis becomes a clinical concern when bad breath persists throughout the day despite regular oral hygiene, when others consistently notice the odor from normal conversation distance (approximately 0.5 to 1 meter), or when you experience additional symptoms such as dry mouth, white tongue coating, or bleeding gums. True halitosis indicates an underlying bacterial imbalance, infection, or systemic condition that requires targeted intervention rather than just mouthwash or mints.
The key distinction lies in duration and response to basic hygiene: temporary bad breath disappears within 30 minutes of brushing and hydrating, while chronic halitosis returns within 2 to 3 hours regardless of oral care efforts. Track your breath quality at different times of day for one week, halitosis shows a consistent pattern rather than isolated incidents tied to specific foods or timing.
Types of halitosis: physiological vs pathological vs pseudo-halitosis
The types of halitosis are:
- Physiological halitosis accounts for approximately 85% of cases and originates from bacterial breakdown of proteins in the mouth itself, producing VSCs primarily on the posterior tongue surface. This type responds well to mechanical cleaning (tongue scraping and interdental brushing) because the source is accessible and not linked to disease. You’ll typically notice improvement within 3 to 5 days of proper tongue hygiene and adequate hydration.
- Pathological halitosis stems from oral diseases such as periodontitis (affecting 15 to 20% of halitosis cases) or systemic conditions including chronic sinusitis, gastroesophageal reflux disease (GERD), or metabolic disorders like uncontrolled diabetes (accounting for less than 5% of cases). This type requires medical or dental treatment of the underlying condition, topical oral care alone won’t resolve the problem. Pathological cases often present with additional warning signs: persistent gum bleeding, tooth mobility, chronic postnasal drip, heartburn, or fruity-smelling breath (indicating ketosis).
- Pseudo-halitosis describes situations where you genuinely believe you have bad breath, but clinical testing reveals no detectable malodor and trusted individuals confirm no odor exists. This perception-reality gap affects approximately 1 to 2% of people concerned about halitosis and requires psychological support rather than dental treatment. Dentists diagnose pseudo-halitosis using organoleptic scoring (trained examiner smelling your breath) and sometimes portable sulfide monitors to provide objective evidence that contradicts your subjective experience.
Halitophobia (breath anxiety): when you smell it but others don’t
Halitophobia represents a psychological condition where persistent fear of having bad breath continues despite multiple professional evaluations confirming no detectable malodor. This affects approximately 0.5 to 1% of the population and often co-occurs with social anxiety disorder or obsessive-compulsive tendencies. You might find yourself constantly checking your breath, avoiding close conversations, covering your mouth excessively, or seeking repeated dental consultations that all yield negative findings.
The condition differs from pseudo-halitosis in severity and persistence: while pseudo-halitosis may resolve after one or two professional confirmations and reassurance, halitophobia remains resistant to evidence and significantly impairs social functioning. Many patients with halitophobia develop elaborate checking rituals (breathing into cupped hands dozens of times daily, carrying multiple breath-freshening products, or asking family members for repeated confirmation) that reinforce rather than reduce the anxiety.
Clinical management requires cognitive-behavioral therapy or psychiatric intervention alongside dental clearance. Your dentist should conduct a thorough halitosis evaluation once to rule out genuine causes, document normal findings, and then refer you to appropriate mental health professionals rather than enabling repeated unnecessary examinations. Repeated dental appointments without psychological treatment typically worsen the condition by providing temporary reassurance that feeds the checking cycle without addressing the underlying anxiety disorder.
Bad breath smell guide: sulfur/rotten-egg vs sour vs fruity (what it can suggest)
Sulfurous or rotten-egg odor indicates bacterial production of hydrogen sulfide and methyl mercaptan, the most common VSCs in oral halitosis, typically originating from tongue coating or gum disease. This sharp, unpleasant smell becomes more pronounced after waking or during fasting because reduced saliva flow allows anaerobic bacteria to proliferate. You’ll notice it intensifies if you skip meals for 6 to 8 hours or breathe primarily through your mouth (which dries tissues and promotes bacterial activity).
Sour or acidic breath suggests acid reflux (GERD), where stomach contents periodically enter the esophagus and oral cavity, or accumulation of acidic bacterial byproducts from tooth decay. GERD-related breath often worsens after meals, when lying flat, or when bending over, patterns that don’t match purely oral halitosis. Dentists can help differentiate by checking for dental erosion patterns on tooth enamel (particularly on tongue-facing surfaces) that confirm chronic acid exposure beyond what diet alone would cause.
Fruity or sweet-smelling breath (similar to overripe fruit or nail polish remover) signals ketosis from diabetes, extreme low-carbohydrate dieting, or prolonged fasting. This odor comes from ketone bodies in your bloodstream being exhaled through your lungs rather than from mouth bacteria, so oral hygiene measures won’t eliminate it. You urgently need medical evaluation when fruity breath appears alongside increased thirst, frequent urination, unexplained weight loss, or fatigue, these symptoms together suggest uncontrolled diabetes requiring immediate intervention. Fecal-smelling breath may indicate intestinal obstruction (medical emergency) or severe sinus infection with trapped purulent material, both requiring prompt specialist care.
The Most Common Oral Causes of Halitosis (Mouth-Related)

The posterior third of your tongue harbors 60 to 70% of odor-causing bacteria that toothbrushing alone cannot remove, making tongue scraping essential for resolving most halitosis cases. Gum disease creates deep pockets between teeth and gums where bacteria colonize unreachable areas, producing continuous odor that persists despite surface cleaning and requires professional scaling to eliminate.
1. Tongue coating and VSC bacteria: why brushing teeth alone isn’t enough
The posterior third of your tongue harbors approximately 60 to 70% of oral bacteria responsible for halitosis, yet most people never clean this area effectively during routine oral hygiene. This region features deep papillae (tiny projections) that trap food debris, dead cells, and bacteria, creating an anaerobic environment where sulfur-producing microorganisms thrive. Brushing your teeth twice daily removes bacteria from smooth tooth surfaces but leaves the primary odor source untouched, which explains why your breath improves for only 1 to 2 hours post-brushing before VSC levels rebuild.
Research shows that mechanical tongue cleaning reduces VSC production by 40 to 75% when performed correctly, making it more effective than mouthwash alone for physiological halitosis. The most efficient technique involves using a dedicated tongue scraper (not your toothbrush) to gently pull forward from the back of your tongue 5 to 7 times, rinsing the scraper between passes. Toothbrush bristles are designed for hard tooth surfaces and prove ineffective at dislodging the sticky biofilm from your tongue’s rough texture, most patients report minimal coating removal when attempting tongue cleaning with their toothbrush.
Common mistakes that reduce effectiveness include scraping too gently (you need firm but not painful pressure), only cleaning the visible anterior tongue (the odor-causing bacteria concentrate in the posterior area you can’t easily see), or skipping this step when rushed. Set a timer for 60 seconds dedicated to tongue cleaning as the final step of your oral hygiene routine, ideally before bed when bacterial accumulation peaks overnight. You should notice clearer, pinker tongue tissue and fresher breath lasting 4 to 6 hours within the first week of consistent scraping.
2. Gum disease (gingivitis/periodontitis): pockets, bleeding gums, and persistent odor
Periodontal disease creates deep spaces (pockets) between your gums and teeth where anaerobic bacteria colonize areas toothbrushes cannot reach, producing continuous VSC emission that persists regardless of surface cleaning. Healthy gums attach to teeth at 1 to 3 millimeters depth; gingivitis pushes this to 4 to 5 millimeters; moderate periodontitis creates 6 to 7 millimeter pockets; advanced cases exceed 8 millimeters. Each millimeter of increased pocket depth exponentially multiplies bacterial surface area and halitosis severity because these deep crevices remain perpetually undisturbed by normal chewing or rinsing.
The distinctive odor from periodontal halitosis combines sulfur compounds with other bacterial metabolites that create a more putrid, persistent smell than simple tongue coating produces. You’ll typically notice this correlates with bleeding gums during brushing or flossing (indicating inflammation), bad taste that lingers throughout the day, food particles that trap between teeth and are difficult to remove, or visible gum recession exposing tooth roots. Approximately 50 to 60% of halitosis patients who fail to respond to basic hygiene improvements have undiagnosed periodontal disease requiring professional intervention.
Surface-level solutions like mouthwash or tongue scraping won’t resolve periodontitis-driven halitosis, you need professional scaling and root planing to mechanically remove calculus (hardened plaque) and infected tissue from pocket depths that only dental instruments reach. Treatment typically requires 2 to 4 appointments for deep cleaning, followed by improved home care focusing on interdental cleaning (floss, interdental brushes, or water flossers) that reaches below the gumline. To understand the full progression of this condition, read about bleeding gums and gum disease causes and treatment. Expect 4 to 6 weeks for inflamed tissues to heal and pocket depths to reduce after scaling, with corresponding breath improvement as bacterial loads drop and gum attachment strengthens.
3. Cavities, broken fillings, and dental infections: hidden “trap zones” that smell
Untreated dental cavities and defective restorations create sheltered areas where food debris ferments and bacteria multiply without disturbance, functioning as permanent odor-generating sites regardless of your hygiene efforts. A cavity larger than 2 to 3 millimeters in depth or width traps food particles that decompose over 24 to 48 hours, releasing foul-smelling compounds you can taste but cannot clean away with brushing or rinsing. Broken fillings or crowns with gaps between the restoration and tooth create similar trap zones, often going unnoticed because they don’t cause pain until infection progresses significantly.
Dental abscesses (infections at tooth roots or in surrounding bone) produce distinctive malodor from pus formation and tissue breakdown, typically accompanied by localized swelling, extreme sensitivity to temperature, throbbing pain, or visible pimple-like bumps on your gums. This infection-driven halitosis smells notably worse than bacterial coating and often creates a persistent bad taste that worsens throughout the day. You can’t resolve infection-related odor with oral hygiene products, these situations require antibiotic therapy and either root canal treatment or tooth extraction to eliminate the infected tissue physically. Learn more about tooth abscess symptoms, danger signs, and urgent treatment to recognize when this is the source of your bad breath.
Wisdom teeth (third molars) present unique challenges in patients aged 17 to 25 when they partially erupt and create a gum flap that traps bacteria and food debris in a space you cannot effectively clean. This condition, called pericoronitis, produces localized bad breath, swelling, and difficulty opening your mouth fully. Wisdom teeth (third molars) present unique challenges in patients aged 17 to 25 when they partially erupt and create a gum flap that traps bacteria and food debris in a space you cannot effectively clean. This condition, called pericoronitis, produces localized bad breath, swelling, and difficulty opening your mouth fully. The only definitive solution involves either professional cleaning of the area by your dentist or wisdom tooth removal, including what to expect during surgery and recovery.
At BrightSmile Dental Clinic, we use clinical examination and X-rays to identify all hidden trap zones contributing to halitosis, treating cavities with fillings (NPR 1,500 to 3,000 depending on size), replacing defective restorations, or performing root canal therapy (NPR 9,800 to 16,000 per tooth) to eliminate infection sources that cleaning alone cannot address.
4. Dentures, retainers, aligners, and braces: cleaning mistakes that cause bad breath
Removable dental appliances develop bacterial biofilms within 24 hours of wear, and most patients fail to clean these devices thoroughly enough to prevent odor accumulation and transfer back to oral tissues. Dentures feature porous acrylic surfaces that absorb bacteria and food particles, requiring daily brushing with appliance-specific cleaners (not regular toothpaste, which is too abrasive) plus soaking in antimicrobial solutions for 6 to 8 hours. Simply rinsing your dentures or brushing them briefly with water leaves 60 to 70% of bacterial biofilm intact, which then recolonizes your mouth when you reinsert the appliance.
Clear aligners and braces, including systems like Invisalign and similar options, trap saliva against your teeth for 20 to 22 hours daily, creating a stagnant environment where bacteria multiply rapidly without the natural cleansing action of saliva flow and tongue movement. Common mistakes include wearing aligners while eating or drinking anything except water (which traps food particles and sugars against teeth), not brushing teeth before reinserting aligners after meals, or going more than 2 days without deep-cleaning the aligners with appropriate solutions. This negligence produces distinctive sour or musty odor noticeable when removing the appliance and often correlates with white film buildup on the plastic.
Fixed orthodontic braces create permanent trap zones around brackets and wires where traditional brushing cannot reach effectively, requiring specialized cleaning tools (interdental brushes, orthodontic flossers, or water flossers) used 2 to 3 times daily. Patients with braces who rely solely on regular toothbrushing typically develop halitosis within 3 to 4 weeks because food particles and plaque accumulate in the dozens of small spaces around each bracket. Effective braces hygiene requires 5 to 7 minutes of dedicated cleaning time, focusing on brushing at 45-degree angles around brackets, using interdental brushes for wire areas, and finishing with water flosser to flush trapped debris, most orthodontic patients spend less than 2 minutes and wonder why their breath worsens despite “brushing regularly.”
Non-Dental Causes and Red Flags (When It’s Not Just the Mouth)
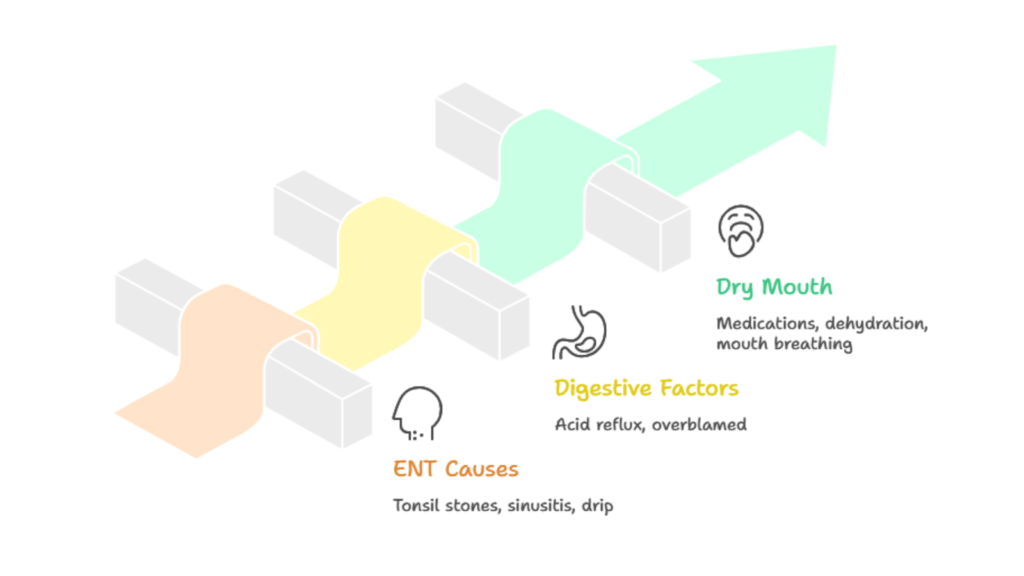
Tonsil stones, chronic sinusitis, and postnasal drip account for 10 to 15% of halitosis cases originating outside the mouth, producing distinctive odor from the back of your throat rather than from tooth or tongue surfaces. Acid reflux causes bad breath in only 5 to 10% of cases despite popular belief, see how acid reflux leads to enamel erosion and what actually helps, and requires specific diagnostic patterns (sour taste, worsening after meals, dental erosion) rather than just reporting stomach problems.
1. Tonsil stones, sinus infection, and post-nasal drip: signs that point to ENT causes
Tonsil stones (tonsilloliths) are calcified accumulations of dead cells, bacteria, and food debris that lodge in tonsil crypts, producing extremely potent sulfur odor that patients describe as “something died in my throat.” These whitish or yellowish formations range from 1 millimeter to over 1 centimeter, sometimes visible when you open wide and look in a mirror, though many remain hidden deep in crypt openings. You’ll typically notice intermittent episodes where severe bad breath coincides with throat discomfort, coughing up small, foul-smelling particles, or metallic taste, patterns that don’t match oral hygiene quality and often worsen despite improved dental care.
Chronic sinusitis creates persistent postnasal drip where infected mucus continuously drains down the back of your throat, coating the posterior tongue and throat tissues with odor-causing bacteria and inflammatory byproducts. This produces halitosis that intensifies upon waking (after hours of horizontal drainage) and often accompanies nasal congestion, facial pressure, thick discolored nasal discharge, or reduced sense of smell. Distinguishing features include breath odor originating from the back of the mouth and throat rather than the front, and the problem worsening during allergy seasons or upper respiratory infections.
ENT-related halitosis requires evaluation by an otolaryngologist rather than a dentist, particularly when you notice enlarged or pitted tonsils, chronic throat clearing, recurrent sinus infections requiring antibiotics 3 or more times per year, or when dental treatment fails to resolve persistent bad breath. Treatment options range from saline nasal irrigation and topical nasal corticosteroids for sinus issues to tonsillectomy for recurrent tonsillitis with chronic stone formation. Your dentist at BrightSmile Dental Clinic will screen for obvious tonsil stones or postnasal drip during examination and refer you to appropriate ENT specialists in Kathmandu when clinical findings suggest non-oral sources.
2. Acid reflux (GERD) and digestive factors: what’s real, what’s overblamed
Gastroesophageal reflux disease produces halitosis in only 5 to 10% of cases, far less frequently than popular belief suggests, and requires specific diagnostic patterns beyond just reporting “stomach problems.” True GERD-related halitosis occurs when stomach acid and partially digested food periodically reach your esophagus and mouth, most commonly during nighttime (when lying flat), immediately after large meals, or when bending over or lifting heavy objects. You’ll typically experience heartburn or sour taste alongside breath changes, isolated bad breath without these accompanying symptoms rarely traces to GERD.
Research shows that simply having GERD doesn’t automatically cause halitosis; only severe or uncontrolled GERD that allows frequent reflux episodes into the upper esophagus and pharynx produces detectable breath changes. Many patients overattribute their halitosis to digestive issues because it feels more acceptable than poor oral hygiene, but clinical studies demonstrate that treating confirmed GERD with proton pump inhibitors (medications like omeprazole) resolves breath odor in only about 30 to 40% of patients who blame stomach issues, the majority actually have unaddressed oral sources discovered upon proper dental evaluation.
Genuine GERD-related halitosis presents with specific patterns: sour or acidic breath (not sulfurous), worsening after meals or at night, improvement when upright or fasting, visible dental erosion on tooth surfaces (especially tongue-facing areas of upper front teeth), and confirmed GERD diagnosis through endoscopy or pH monitoring. A useful test involves treating your mouth thoroughly for 2 weeks (professional cleaning plus meticulous home care) while tracking whether symptoms persist, if halitosis continues unchanged despite excellent oral hygiene and healthy gums, then systemic causes like GERD warrant investigation. Don’t assume stomach issues without evidence; over 85% of halitosis resolves with proper oral treatment alone.
3. Dry mouth (xerostomia): medications, dehydration, mouth breathing, and snoring links
Saliva naturally cleanses your mouth by washing away food debris and dead cells, neutralizing acids, and providing antimicrobial proteins, reduced saliva flow allows bacterial populations to multiply unchecked and VSC production to increase 3 to 5 fold. Xerostomia (dry mouth) affects approximately 20% of adults and stems from multiple causes: over 400 medications including antihistamines, antidepressants, blood pressure medications, and diuretics; insufficient water intake (less than 1.5 to 2 liters daily); chronic mouth breathing during sleep or due to nasal obstruction; and systemic conditions like diabetes or Sjögren syndrome. For a deeper look at how reduced saliva flow directly fuels persistent odor, see dry mouth causes, its bad breath link, and remedies.
Medication-induced dry mouth represents the most common reversible cause, particularly affecting patients taking multiple daily medications who notice worsening halitosis that correlates with when they started new prescriptions. You can confirm medication-related xerostomia by tracking saliva changes after dose timing, many drugs cause peak dry mouth effects 2 to 4 hours post-dose, corresponding to breath odor spikes. Never discontinue prescribed medications without physician consultation, but you can implement saliva-stimulating strategies: frequent water sipping throughout the day, sugar-free gum or lozenges containing xylitol (which stimulates flow), and avoiding alcohol-containing mouthwashes that further dry tissues.
Mouth breathing during sleep drastically reduces oral moisture overnight, explaining why many people wake with extremely dry mouth and severe morning breath that exceeds normal physiological patterns. This often links to snoring, sleep apnea, chronic nasal congestion, or anatomical factors (deviated septum, enlarged turbinates). Clues that mouth breathing contributes to your halitosis include waking with cracked lips or dry throat, bed partners reporting your mouth hangs open during sleep, or noticing the problem disappears on nights you use nasal breathing strips or when nasal congestion improves. Addressing the underlying breathing obstruction, through ENT evaluation, allergy management, or sleep study for suspected apnea, often resolves the dry mouth and associated halitosis more effectively than topical mouth moisturizers alone.
Red flags: when to see a dentist or doctor urgently (pain, swelling, fever, worsening odor)
Certain symptoms accompanying bad breath signal serious infections or systemic conditions requiring immediate professional evaluation rather than waiting for routine appointments. Seek urgent dental care within 24 hours when you experience facial or gum swelling (particularly if it restricts mouth opening or spreads toward your eye or neck), fever above 38°C (100.4°F) with oral pain, severe throbbing toothache that prevents sleep or normal function, or visible pus discharge from gums or tooth areas. These signs indicate dental abscess or spreading infection that can progress to life-threatening complications when delayed.
Sudden onset of severe halitosis that develops over 1 to 3 days rather than gradually often accompanies acute infections: rapidly progressive gum disease (acute necrotizing ulcerative gingivitis), peritonsillar abscess, or infected wisdom teeth. This differs from chronic halitosis that builds slowly over weeks or months. You’ll typically notice this acute pattern correlates with systemic symptoms (fever, fatigue, difficulty swallowing) rather than occurring in isolation, and the breath odor is markedly more putrid than your baseline.
Non-dental red flags requiring urgent medical (not just dental) evaluation include fruity-smelling breath with increased thirst and urination (possible diabetic ketoacidosis), fecal-smelling breath with abdominal pain or vomiting (possible intestinal obstruction), ammonia or urine-like breath smell (suggesting kidney dysfunction), or musty-sweet breath with cognitive changes or jaundice (indicating liver problems). These metabolic breath changes originate from bloodstream compounds being exhaled through your lungs rather than from mouth bacteria, so they won’t improve with oral care and demand immediate laboratory testing and medical intervention. Schedule emergency medical assessment when breath changes accompany unexplained weight loss, night sweats, persistent cough, or chronic fatigue, rare cases of halitosis signal underlying cancer or serious systemic disease requiring prompt diagnosis.
Symptoms, Self-Checks, and the Biggest Myths That Waste Time
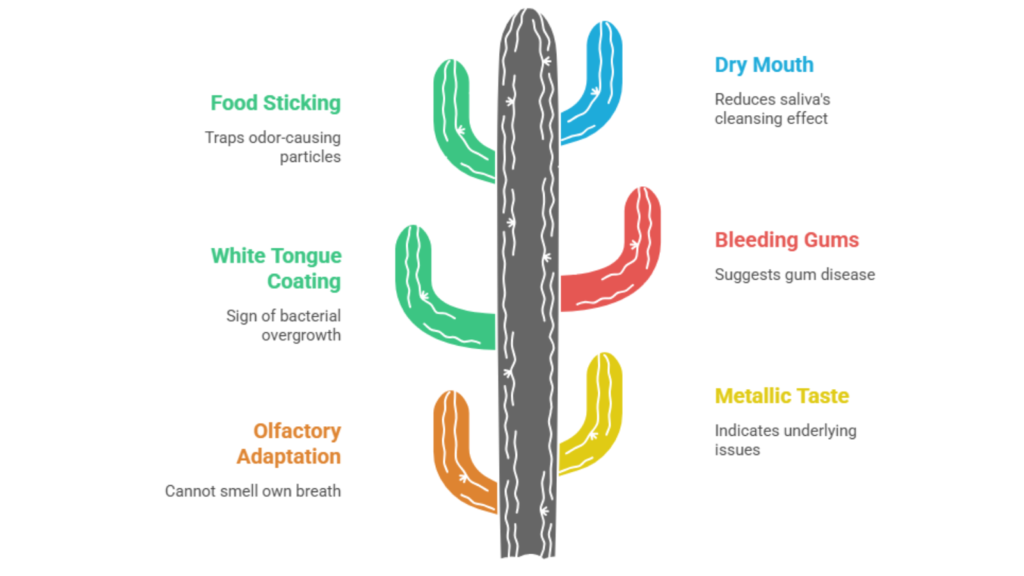
Persistent metallic taste, thick white tongue coating, bleeding gums during brushing, and chronic dry mouth serve as reliable indicators that correlate with detectable halitosis in 70% of cases. You cannot accurately smell your own breath because your olfactory system adapts to constant odors within 2 to 5 minutes, making the only reliable self-test asking a trusted person to assess your breath at different times of day or scraping your tongue with a spoon and smelling the collected material.
Symptoms checklist: bad taste, white tongue, bleeding gums, food getting stuck, dry mouth
Persistent metallic or bitter taste in your mouth, noticeable throughout the day regardless of eating or drinking, strongly correlates with halitosis and typically indicates bacterial activity or gum inflammation. This taste differs from temporary flavor changes after specific foods or medications, you’ll notice it returns within 30 to 60 minutes even after brushing and using mouthwash. Approximately 70% of patients with chronic bad taste also have detectable halitosis when professionally assessed, making this one of the most reliable self-indicators that others likely smell what you taste.
White or yellowish coating on your tongue, particularly concentrated on the posterior third, visually confirms excessive bacterial accumulation producing VSCs. Use your phone camera with flash to photograph your extended tongue, healthy tongue tissue appears light pink with minimal coating. Thick white coating that doesn’t easily brush away indicates the bacterial biofilm has matured over 24 to 48 hours and requires mechanical scraping (not just brushing) to remove effectively. This coating often feels fuzzy or rough when you run your tongue across the roof of your mouth.
Bleeding gums during brushing or flossing (even small amounts of blood) signals inflammation from bacterial infection, nearly always accompanying halitosis in these cases. Healthy gums don’t bleed from normal brushing pressure, any bleeding indicates your immune system is fighting bacterial invasion in gum tissues. Additional warning signs include food particles that consistently trap between the same teeth (indicating pocket formation or spacing issues), chronic dry mouth requiring frequent water sipping to remain comfortable, or the sensation that you need to constantly clear your throat (suggesting postnasal drip or tonsil stones). Track these symptoms for 5 to 7 days; having 3 or more concurrently suggests oral disease requiring professional treatment rather than just improved hygiene.
How to test your breath at home (reliable methods) and what to avoid
The most accurate home test involves asking a trusted person you see regularly to honestly smell your breath from normal conversation distance (approximately 0.5 meters) at different times of day. Choose someone who interacts with you daily and will provide truthful feedback without trying to spare your feelings, many halitosis sufferers receive false reassurance from family members avoiding awkward conversations. Schedule 3 separate assessments: first thing after waking (before any oral hygiene), mid-afternoon (at least 3 hours after eating or brushing), and before bed. Consistent detection at all 3 time points confirms chronic halitosis; detection only in the morning suggests normal physiological patterns.
The wrist-lick test (licking your wrist, waiting 10 seconds, then smelling it) provides moderate reliability but tests primarily front-of-mouth saliva rather than posterior tongue coating where most VSCs originate. A more accurate variation involves using a clean spoon to gently scrape the back of your tongue 3 to 4 times, then smelling the spoon after 30 seconds, the material you collect should appear whitish or yellowish if bacterial coating is present, and the odor will approximate what others smell. Strong unpleasant odor from this scraping confirms halitosis; minimal or no odor suggests your breath concerns may be overestimated.
Avoid unreliable methods that create false results: breathing into cupped hands and smelling immediately (your nose adapts to your own odors too quickly for objective assessment), using disposable face masks then smelling them after wearing for several hours (traps condensation and bacteria in ways that don’t reflect actual breath), or obsessively asking the same person repeatedly throughout the day (creates response bias as they become desensitized or annoyed). Commercial breath-testing devices measuring sulfide levels (available for NPR 3,000 to 8,000) can quantify VSCs but don’t replace professional evaluation, they measure one factor without identifying the underlying cause or appropriate treatment.
Why you can’t “taste” your own breath accurately (and how to get honest feedback)
Your olfactory system (sense of smell) automatically adapts to constant odors within 2 to 5 minutes, making it physiologically impossible to accurately perceive your own breath odor regardless of how hard you try. This adaptation, called olfactory fatigue, evolved to help detect new environmental threats rather than continuously processing familiar background smells. You experience this same phenomenon when you stop noticing your home’s scent, your perfume or cologne fades from your perception after application, or you can’t smell your own body odor as readily as strangers would, your breath odor follows identical neurological patterns.
The disconnect between self-perception and reality explains why many patients with severe halitosis genuinely believe they have no problem, while others with clinically normal breath develop halitophobia convinced they smell terrible. Approximately 30 to 40% of people cannot detect their own bad breath even when others clearly smell it, and conversely about 20% perceive odor where none objectively exists. Trying to “taste” your breath by breathing through your mouth or trapping breath in your hands creates artificial conditions that don’t replicate what others experience during normal conversation, these methods typically underestimate actual halitosis severity.
The only reliable method involves recruiting objective assessors who interact with you regularly enough to notice patterns but haven’t adapted to your baseline odor. Explain that you need honest feedback about a health concern (not just reassurance), specify that vague politeness won’t help you get proper treatment, and ask for assessment at times when you haven’t recently eaten strong-flavored foods or used breath products. Alternatively, schedule professional evaluation at a dental clinic where practitioners use standardized organoleptic scoring (rating breath odor on 0 to 5 scales) and sometimes portable sulfide monitors that provide objective measurements independent of subjective perception. At BrightSmile Dental Clinic, we perform clinical halitosis assessment using both examiner scoring and symptom correlation to diagnose the problem definitively before recommending treatment.
Halitosis myths and misconceptions: “it’s always the stomach,” “mouthwash solves it,” and more
The most persistent myth claims that bad breath originates from stomach problems in most cases, yet research shows that oral sources account for 85 to 90% of halitosis while true gastrointestinal causes represent less than 5%. This misconception causes patients to waste months pursuing digestive treatments, changing diets, taking probiotics, treating presumed GERD, while ignoring the bacterial coating on their tongue or gum disease that actually produces the odor. Your stomach is a closed system sealed by the lower esophageal sphincter except during active reflux episodes; gases and odors from digestion don’t simply travel upward during normal function.
Another common misconception suggests that mouthwash alone can cure halitosis, when in reality, antimicrobial rinses only temporarily suppress bacterial activity for 1 to 3 hours without addressing the underlying colonization sources. Mouthwash containing cetylpyridinium chloride (CPC) or essential oils reduces VSC production by 20 to 30% for short periods, functioning as a helpful adjunct to mechanical cleaning but never as a standalone solution. Patients who rely exclusively on mouthwash without tongue scraping, interdental cleaning, and professional treatment of gum disease or cavities maintain the bacterial reservoirs that continuously repopulate and produce new odor compounds.
The belief that “everyone gets bad breath from food” conflates temporary dietary effects with chronic halitosis. Garlic, onions, coffee, and alcohol do produce noticeable breath changes, but these resolve within 24 to 48 hours as the compounds metabolize and clear from your system, and they affect everyone equally regardless of oral health status. Chronic halitosis persists on days you avoid these foods entirely and typically smells different (sulfurous rather than food-specific) from simple dietary breath. Similarly, the myth that “brushing teeth harder or more often” cures halitosis fails because most cases stem from tongue coating, gum pockets, or systemic factors that tooth-brushing doesn’t address, excessive brushing can damage gums and enamel while leaving the actual odor source untouched.
Diagnosis at a Dental Clinic in Kathmandu: Step-by-Step Evaluation
Your dentist begins with detailed questions about timing patterns, lifestyle factors (tobacco use, medications, hydration), and systemic symptoms to identify whether halitosis stems from oral bacteria, gum disease, or requires ENT or medical referral. Clinical examination systematically evaluates tongue coating thickness, gum pocket depths around each tooth, visible cavities or broken restorations, and tonsil areas, identifying the primary odor source in approximately 80% of cases before any laboratory testing.
1. What your dentist will ask: diet, tobacco, hydration, meds, reflux, and daily routine
Your dentist will begin by asking detailed questions about timing patterns: when you first noticed the halitosis, whether others have commented on it (and how frequently), and what times of day the odor is most severe. This establishes whether you’re dealing with normal morning breath, meal-related temporary changes, or true chronic halitosis that persists regardless of timing. Expect questions about attempted solutions, what oral hygiene products you’ve tried, how long you used them, and whether you noticed any improvement (even temporary). Patients who report zero response to improved brushing and tongue cleaning typically have non-oral causes or pathological oral conditions requiring professional intervention.
Lifestyle history helps identify contributing factors: tobacco use (smoking or chewing tobacco reduces saliva production and promotes gum disease), alcohol consumption (dries mouth tissues), caffeine intake (mild diuretic effect), and daily water consumption (aiming for 2 to 3 liters daily in Kathmandu’s dry climate). Your dentist will specifically ask about medications you take regularly because xerostomia represents a side effect of hundreds of common drugs, bring a complete medication list including over-the-counter supplements. Questions about acid reflux, heartburn, sinus problems, snoring, or mouth breathing during sleep screen for systemic and anatomical factors beyond oral sources.
Diet questions focus less on blaming specific foods and more on identifying patterns: do you eat breakfast (skipping morning meals reduces saliva stimulation), how frequently you snack between meals (affects bacterial feeding cycles), and whether you notice correlations between certain foods and breath changes. Your dentist may ask about fasting periods for religious observance or dietary reasons, as extended fasting (8 or more hours) predictably worsens physiological halitosis. This conversation typically takes 5 to 7 minutes and provides your dentist with enough context to prioritize which diagnostic procedures will most efficiently identify your specific halitosis source.
2. Clinical exam that finds the source: gums, tongue, cavities, infection, appliances, wisdom area
The intraoral examination systematically evaluates every potential bacterial reservoir starting with the tongue: your dentist will ask you to extend your tongue fully and visually assess the coating thickness and distribution, often using a tongue blade to gently scrape the posterior surface. Thick white or yellowish coating that doesn’t easily dislodge indicates mature bacterial biofilm requiring mechanical removal. Dentists look for “hairy tongue” (elongated papillae that trap more debris) or geographical tongue (patchy areas with different coating patterns) that increase halitosis risk.
Periodontal evaluation involves probing around each tooth to measure pocket depths (normal 1 to 3 millimeters; 4 to 5 millimeters indicates gingivitis; 6 or deeper signals periodontitis), noting bleeding on probing (indicating active inflammation), and checking for gum recession, tooth mobility, or pus discharge. Your dentist will examine tooth surfaces for visible cavities, fractured teeth, broken or loose fillings and crowns, and areas where food consistently traps between teeth. Special attention goes to wisdom teeth areas (particularly partially erupted third molars), spaces where teeth have been removed without replacement, and areas around dental appliances like bridges or implants.
Your dentist will check any removable appliances you wear (dentures, retainers, aligners) for cleanliness, proper fit, and signs of biofilm accumulation or acrylic degradation that harbor bacteria. Visualization of tonsils and posterior throat helps identify obvious tonsilloliths (white or yellow debris in tonsil crypts) or postnasal drip indicating ENT involvement. The entire clinical exam typically requires 10 to 15 minutes and often identifies the primary halitosis source before any laboratory testing. At BrightSmile Dental Clinic in Putalisadak, we combine this thorough visual examination with patient history to pinpoint causes in approximately 80% of cases during the initial consultation.
3. Tests that confirm halitosis: organoleptic scoring, VSC meters, gum pocket charting, X-rays
Organoleptic scoring represents the gold standard for halitosis diagnosis, where a trained examiner (typically your dentist or a dental hygienist) directly smells your breath and rates the odor intensity on a 0 to 5 scale. The examiner asks you to breathe normally through your mouth at a distance of approximately 10 centimeters (about 4 inches), wait 30 seconds without talking to allow oral air to equilibrate, then exhale slowly while the examiner assesses. Scores of 0 (no odor) to 1 (barely noticeable) fall within normal range; 2 indicates slight but definite halitosis; 3 represents moderate halitosis clearly noticeable in normal conversation; 4 to 5 indicates severe halitosis detectable from greater distances. This subjective method correlates well with objective measurements and costs nothing beyond clinical time.
Portable sulfide monitors (costing NPR 50,000 to 150,000 for professional models) objectively measure VSC concentrations in parts per billion, typically reading breath samples from a tube you breathe into for 30 seconds. Readings below 100 ppb (parts per billion) generally indicate no significant halitosis; 100 to 150 ppb suggests mild halitosis; 150 to 300 ppb indicates moderate levels; above 300 ppb confirms severe VSC production requiring treatment. While more objective than organoleptic scoring, these devices only measure sulfur compounds and miss other malodorous substances, so they serve as supplements rather than replacements for examiner assessment.
Periodontal charting involves recording pocket depths around every tooth (usually 6 measurements per tooth for comprehensive mapping), bleeding points, and recession measurements to document gum disease severity and extent. Dental X-rays reveal hidden decay between teeth, bone loss around tooth roots indicating periodontitis, periapical infections at tooth tips, and impacted or problematic wisdom teeth not visible during clinical examination. A full diagnostic workup combining these tests typically costs NPR 3,000 to 5,000 at Kathmandu dental clinics, providing definitive diagnosis before beginning treatment.
When referrals happen: ENT vs physician vs gastro (and what to check next)
Your dentist will refer you to an otolaryngologist (ENT specialist) when clinical findings suggest tonsil stones, chronic sinusitis, or structural nasal problems as primary halitosis sources. This typically occurs when you present with visible enlarged or cryptic tonsils containing debris, report chronic nasal congestion or postnasal drip alongside halitosis, or when treating obvious oral issues (cleaning, fillings, gum treatment) fails to resolve bad breath after 4 to 6 weeks. The ENT will perform nasal endoscopy to visualize sinus drainage pathways, assess tonsil crypts more thoroughly than dental examination allows, and may recommend imaging studies (CT scans) for chronic sinusitis that doesn’t respond to medical management.
Physician referrals (to your general practitioner or internist) are indicated when your breath odor suggests metabolic issues, fruity smell with diabetes symptoms, ammonia odor with possible kidney dysfunction, or when you report significant dry mouth alongside systemic symptoms like unexplained weight changes, chronic fatigue, or joint pain that could indicate Sjögren syndrome or other autoimmune conditions. Your physician will order blood tests checking glucose control (HbA1c for diabetes screening), kidney function (creatinine and blood urea nitrogen), liver enzymes, and may perform autoimmune panels. Medication reviews with your physician help identify xerostomia-causing drugs and explore alternatives when available.
Gastroenterology referral becomes necessary only when you report typical GERD symptoms (heartburn, acid regurgitation, difficulty swallowing) alongside halitosis, or when your dentist observes dental erosion patterns suggesting chronic acid exposure. The gastroenterologist may recommend esophagogastroduodenoscopy (endoscopy) to visualize your esophagus and stomach directly, pH monitoring studies that track acid reflux episodes over 24 hours, or trials of proton pump inhibitor medications to see if suppressing acid production resolves both reflux symptoms and associated breath changes. Importantly, gastroenterology referral should occur only after ruling out oral causes, most patients referred for presumed “stomach-related” halitosis actually need dental treatment rather than digestive evaluation.
Treatments That Work: Professional Care and a Simple Daily Prevention Plan
Professional scaling and root planing removes calculus and infected tissue from gum pockets up to 8 to 10 millimeters deep that home care cannot reach, while restorative treatments (fillings for cavities, root canals for infections, wisdom tooth extractions) permanently eliminate bacterial trap zones causing persistent odor.
In-clinic treatments: scaling/deep cleaning, fillings, infection care, denture/appliance adjustments
Professional scaling and root planing (deep cleaning) represents the foundational treatment for halitosis linked to gum disease, mechanically removing calculus and infected tissue from pocket depths that home care cannot reach. Professional scaling and root planing (deep cleaning) represents the foundational treatment for halitosis linked to gum disease, mechanically removing calculus and infected tissue from pocket depths that home care cannot reach. If you want to understand exactly what happens during professional teeth cleaning and scaling, the procedure typically requires 2 to 4 appointments depending on disease severity, with local anesthesia to ensure comfort during deep subgingival cleaning.
Your dentist or hygienist uses ultrasonic scalers and hand instruments to debride bacterial deposits from tooth roots up to 8 to 10 millimeters below the gumline, smoothing root surfaces to prevent rapid bacterial recolonization. Expect 4 to 6 weeks for gum healing post-treatment, with most patients noticing breath improvement within 2 to 3 weeks as inflammation subsides and pocket depths reduce.
Restorative treatments address structural causes: composite fillings (NPR 1,500 to 3,000 per tooth at BrightSmile Dental Clinic) eliminate cavities that trap bacteria; crown replacements (NPR 8,000 to 15,000 depending on material) fix defective restorations creating gaps where food accumulates; root canal therapy (NPR 9,800 to 16,000 per tooth) resolves dental infections producing pus and odor. These treatments permanently remove the “trap zones” that allow bacterial colonization regardless of hygiene efforts, typically resolving associated halitosis within 1 to 2 weeks post-treatment as the treated areas heal.
Denture adjustments or relining improve appliance fit and reduce areas where food debris traps beneath the denture base, while professional ultrasonic denture cleaning removes embedded bacterial biofilm that daily brushing misses. For patients with retainers or aligners, your dentist may recommend switching to nightly-only wear (if orthodontically appropriate) to reduce the hours of stagnant saliva trapped against teeth, or prescribe antimicrobial aligner cleaning systems. Problematic wisdom teeth may require surgical extraction (NPR 5,000 to 12,000 depending on impaction difficulty) when pericoronitis and associated halitosis recur despite repeated professional cleaning attempts.
At-home routine that actually fixes halitosis: brushing and interdental cleaning and tongue scraping
A comprehensive home care routine requires 3 distinct mechanical cleaning actions performed in the correct sequence twice daily: firstly, interdental cleaning (floss or interdental brushes); secondly, tongue scraping; thirdly, tooth brushing. Starting with interdental cleaning while you’re motivated and before fatigue sets in ensures you remove plaque and food debris from between teeth and below the gumline, areas that harbor 30 to 40% of oral bacteria but get neglected when you rush. Use waxed dental floss, interdental brushes sized appropriately for your tooth spacing, or water flossers on medium to high settings for 2 to 3 minutes, cleaning all tooth surfaces including back molars where access is difficult.
Tongue scraping follows interdental cleaning: use a dedicated tongue scraper (not your toothbrush) positioned as far back on your tongue as comfortable without triggering gag reflex, then pull forward with firm pressure 5 to 7 times, rinsing the scraper between passes. The goal is to remove visible white or yellow coating, leaving pinker tongue tissue, this should take 60 to 90 seconds daily. Perform this before brushing so you don’t recontaminate cleaned teeth with the bacterial debris you’re removing from your tongue.
Tooth brushing comes last, using soft-bristled brushes and fluoride toothpaste for 2 minutes minimum, focusing on the gumline where plaque accumulates most heavily and using gentle circular motions rather than aggressive horizontal scrubbing that damages gums. Electric toothbrushes with pressure sensors and 2-minute timers help ensure adequate technique and duration. This complete routine requires 5 to 7 minutes twice daily, significantly longer than the 30 to 60 seconds most people spend on hasty brushing alone. Set a timer during your first week to build the habit, and expect noticeable breath improvement within 3 to 5 days as you reduce bacterial loads consistently.
Mouthwash and products: CPC/essential oils vs chlorhexidine (short-term) and safety cautions
Antimicrobial mouthwashes serve as useful adjuncts to mechanical cleaning but never as replacements, with cetylpyridinium chloride (CPC) and essential oil formulas appropriate for long-term daily use. CPC rinses (found in products like Crest Pro-Health and some Colgate formulas) reduce bacterial populations by approximately 20 to 30% and provide 2 to 3 hours of VSC suppression when used twice daily after mechanical cleaning. Essential oil mouthwashes (like Listerine) containing thymol, eucalyptol, menthol, and methyl salicylate show similar efficacy with slightly different antimicrobial spectrum, choose based on taste preference since consistency of use matters more than minor efficacy differences.
Use mouthwash after completing brushing, flossing, and tongue scraping (not before, which would wash away the antimicrobial agents prematurely). Swish vigorously for 30 to 60 seconds, making sure to gargle briefly to reach posterior throat areas, then spit without rinsing with water afterward to maximize residual activity. Avoid mouthwashes containing high alcohol concentrations (over 20%), which dry oral tissues and can paradoxically worsen halitosis long-term despite providing temporary fresh sensation, alcohol-free formulations now dominate the market and work equally well without drying effects.
Chlorhexidine gluconate 0.12% or 0.2% represents the most potent antimicrobial mouthwash available but should only be used for short-term periods (2 to 4 weeks maximum) under dental supervision because prolonged use causes brown staining on teeth and tongue, taste alterations, and potential disruption of healthy oral microbiome balance. Your dentist may prescribe chlorhexidine following gum disease treatment or oral surgery to reduce bacterial loads during healing, but it’s inappropriate for daily long-term halitosis prevention. Never use chlorhexidine for more than the prescribed duration, and inform your dentist if you notice staining or taste changes developing so treatment can be adjusted.
A 14-day “breath reset” plan: daily checklist and when to follow up if it returns
Days 1-3 focus on establishing mechanical cleaning habits without adding other variables: floss or use interdental brushes for all tooth surfaces once before bed, scrape your tongue until coating visibly reduces (60 seconds), then brush for 2 full minutes. Drink 2 to 3 liters of water spread throughout the day to maintain saliva production, and avoid skipping meals (which reduces saliva stimulation for extended periods). Take before-photos of your extended tongue to document baseline coating, and ask a trusted person to assess your breath at a consistent time each day (such as mid-afternoon) using the same 0 to 5 scale dentists use. Most people notice 20 to 30% breath improvement by Day 3 from mechanical cleaning alone, confirming physiological rather than pathological halitosis.
Days 4-7 add targeted products: incorporate alcohol-free antimicrobial mouthwash (CPC or essential oils) twice daily after mechanical cleaning, and begin using sugar-free xylitol gum or lozenges between meals to stimulate saliva flow if you experience any dry mouth. Keep refining your interdental cleaning technique, you should see less bleeding and easier floss passage as gum inflammation decreases. By Day 7, reassess: improvements of 40 to 60% suggest your routine is working and you should continue; minimal improvement (less than 20%) or no change indicates you likely need professional intervention for underlying gum disease, cavities, or systemic issues requiring diagnosis.
Days 8-14 focus on consistency and troubleshooting: maintain the full routine twice daily without exceptions, and identify any times when breath worsens (after certain foods, upon waking, during stress) to understand your specific patterns. Schedule a follow-up dental appointment if breath improvement plateaus below 50% or if you notice persistent symptoms like bleeding gums, bad taste, or visible coating despite compliant hygiene, review bleeding gums and gum disease causes and treatment to understand what could be happening, or visit dental in Kathmandu to explore comprehensive care options available locally. Most patients with purely physiological halitosis achieve 70 to 80% improvement by Day 14 and can maintain results with consistent daily care. Breath odor returning to baseline within 2 to 3 days of reducing your routine confirms the need for permanent habit change rather than temporary fixes.
Can bad breath come from the stomach?
Stomach-related bad breath accounts for less than 5% of cases. Most halitosis originates in the mouth, especially from tongue coating, gum disease, or tooth decay. GERD-related breath only occurs when acid reflux reaches the mouth and is usually accompanied by heartburn or a sour taste.
How often should I scrape my tongue?
Scrape your tongue once daily before bed using a tongue scraper, not a toothbrush. Most odor-causing bacteria live on the posterior third of the tongue, where brushes are ineffective. Scrape 5 to 7 times with firm pressure and rinse between passes to reduce odor within 3 to 5 days.
Does mouthwash cure bad breath permanently?
Mouthwash does not cure bad breath permanently. It reduces bacteria for 1 to 3 hours but cannot eliminate halitosis without addressing root causes like tongue coating, plaque, or gum disease. Use mouthwash as a supplement to brushing, flossing, and tongue scraping for better long-term results.
Why does my breath smell bad even after brushing?
Bad breath persists after brushing because most odor-causing bacteria live on the tongue’s back and between teeth. Brushing alone misses up to 70% of bacteria, especially without flossing or tongue scraping. Gum disease and plaque below the gumline also contribute and require professional care.
Can wisdom teeth cause bad breath?
Partially erupted wisdom teeth trap food and bacteria under gum flaps, leading to localized bad breath and inflammation called pericoronitis. This condition is common in people aged 17 to 25. Treatment may include professional cleaning or surgical removal depending on severity and recurrence.
How do I know if I have bad breath?
You can’t reliably smell your own breath. Ask someone you trust to check at different times, or scrape the back of your tongue and smell it after 30 seconds. For a definitive answer, visit a dentist for an evaluation using standardized odor scoring.
What’s the fastest way to fix bad breath?
Fix bad breath fast by scraping your tongue daily, flossing, and brushing twice a day for two minutes. Drink 2 to 3 liters of water daily and avoid mouth-breathing. Most people notice 40–60% improvement in 5 to 7 days. Seek dental care if symptoms persist beyond 2 weeks.
Do certain foods cause permanent bad breath?
Certain foods like garlic and onions cause temporary breath odor, not permanent halitosis. These smells clear within 24–48 hours. Chronic bad breath that persists without eating these foods often signals bacterial buildup, gum disease, or systemic issues requiring treatment.
When should I see a dentist for bad breath?
See a dentist if bad breath lasts more than 2 weeks despite flossing, brushing, and tongue scraping. Also go if others mention your breath or if you have bleeding gums, bad taste, or thick tongue coating. Seek urgent care for swelling, pain, or fever over 38°C.
Can dry mouth cause bad breath?
Yes, dry mouth causes bad breath by reducing saliva’s ability to cleanse the mouth. Over 400 medications cause dry mouth, including antihistamines and antidepressants. Mouth breathing and low water intake also worsen symptoms. Use xylitol gum, stay hydrated, and avoid alcohol-based rinses.
If you’re experiencing persistent bad breath despite improving your oral hygiene, or if you’d like professional halitosis evaluation to identify the exact source, schedule a comprehensive dental examination at BrightSmile Dental Clinic. We’re located in Putalisadak, Kathmandu, and offer thorough halitosis assessment including clinical evaluation, periodontal charting, and treatment planning tailored to your specific situation. Call +977-9748343015 or email brightsmileclinic33@gmail.com to book your consultation, most halitosis cases resolve completely with proper diagnosis and targeted treatment within 4 to 6 weeks.
