Dental pain can disrupt your daily life, making simple tasks like eating or sleeping unbearable. Many patients in Kathmandu delay visiting their dentist, hoping symptoms will disappear on their own. Understanding warning signs early can save your natural tooth and prevent serious complications.
Root canal treatment remains one of the most misunderstood dental procedures, often surrounded by unnecessary fear. Modern dentistry has transformed this procedure into a comfortable, pain-relieving experience. Recognising symptoms early allows for timely intervention, preserving your smile and oral health.
This comprehensive guide explores the top 5 signs indicating you may need root canal therapy. We break down each symptom, explain what happens inside your tooth, and help you understand when to seek professional help. Knowledge empowers you to make informed decisions about your dental health.
Understanding Root Canal
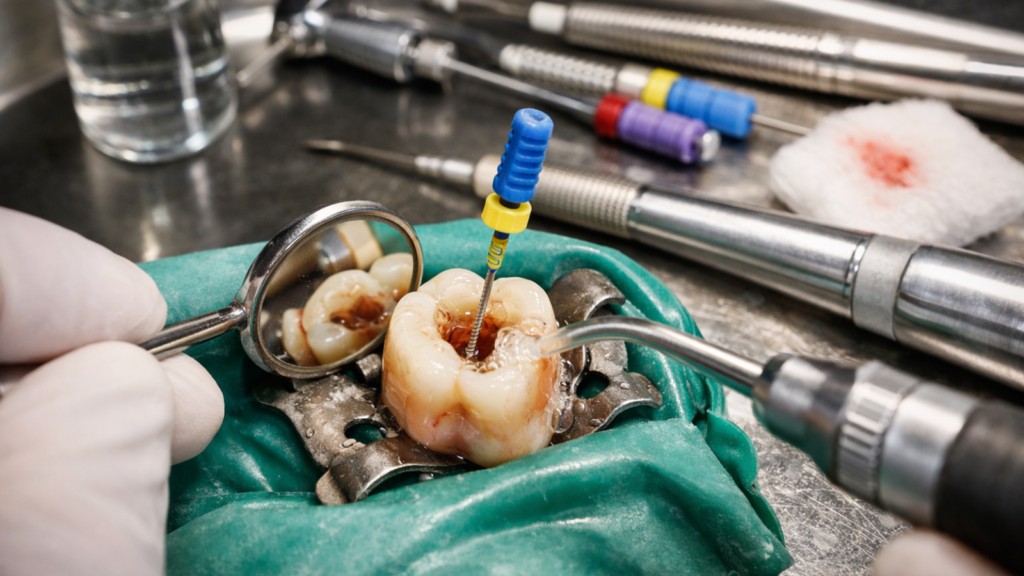
Root canal treatment saves severely infected or damaged teeth by removing diseased pulp tissue from inside the tooth. Modern techniques and anaesthesia have transformed this procedure into a comfortable, pain-relieving experience that preserves your natural tooth structure. Recognising symptoms early allows dentists in Kathmandu to intervene before infections spread, protecting your oral health and preventing costly tooth loss.
What Is a Root Canal and Why Dentists Perform It
A root canal is a dental procedure that removes infected or inflamed pulp tissue from inside your tooth. Each tooth contains soft pulp tissue housing nerves, blood vessels, and connective tissue within hollow spaces called root canals. Dentists perform this treatment to eliminate infection, relieve severe pain, and preserve your natural tooth rather than extracting it.
Saving natural teeth offers significant advantages over extraction and replacement options. Your natural tooth maintains proper jaw bone density, prevents neighbouring teeth from shifting, and functions just like before treatment. Root canal therapy has evolved into a routine, virtually painless procedure using modern anaesthesia and advanced techniques.
Preserving natural tooth structure benefits your overall oral health long-term. Artificial replacements like implants or bridges, while effective, cannot perfectly replicate natural tooth function. Early intervention through root canal treatment prevents infection spread and protects surrounding teeth and bone tissue.
How Pulp Infection Develops (Tooth Decay, Cracks, Trauma)
Pulp infection occurs when bacteria penetrate through protective enamel and dentin layers to reach soft inner tissue. Deep cavities from untreated tooth decay create pathways for bacterial invasion, gradually destroying healthy pulp. Once bacteria establish infection inside, inflammation and severe pain typically follow.
Cracks or chips in teeth, even hairline fractures you cannot see, allow bacteria direct access to pulp chambers. Physical trauma from accidents, sports injuries, or biting hard objects can bruise or damage pulp tissue internally. Multiple dental procedures on one tooth over time may eventually irritate or weaken pulp, increasing infection risk.
Untreated infections never resolve spontaneously; bacteria multiply and spread deeper into root canals and surrounding bone. Abscesses form when pus accumulates at root tips, creating pressure and intense discomfort. Without professional treatment, infected teeth ultimately lead to tooth loss and potential systemic health complications.
Who Is at Higher Risk (Age, Prior Dental Work, Oral Hygiene)
Individuals with extensive prior dental work face elevated infection risk because repeated procedures can stress pulp tissue. Older patients may experience natural pulp deterioration over decades, making teeth more vulnerable to infection. Poor oral hygiene habits accelerate cavity formation, increasing likelihood of deep decay reaching pulp chambers.
People who grind their teeth (bruxism) often develop microscopic cracks that serve as bacterial entry points. Patients with compromised immune systems fight dental infections less effectively, allowing bacteria to thrive. Those avoiding regular dental check-ups miss early cavity detection, letting decay progress until root canal becomes necessary.
Certain lifestyle factors compound risk: high-sugar diets promote rapid tooth decay, while smoking impairs healing and increases infection susceptibility. Patients postponing cavity treatment allow small problems to escalate into pulp infections. Understanding personal risk factors helps you prioritise preventive care and regular dental examinations.
The Top 5 Signs Every Patient Should Know
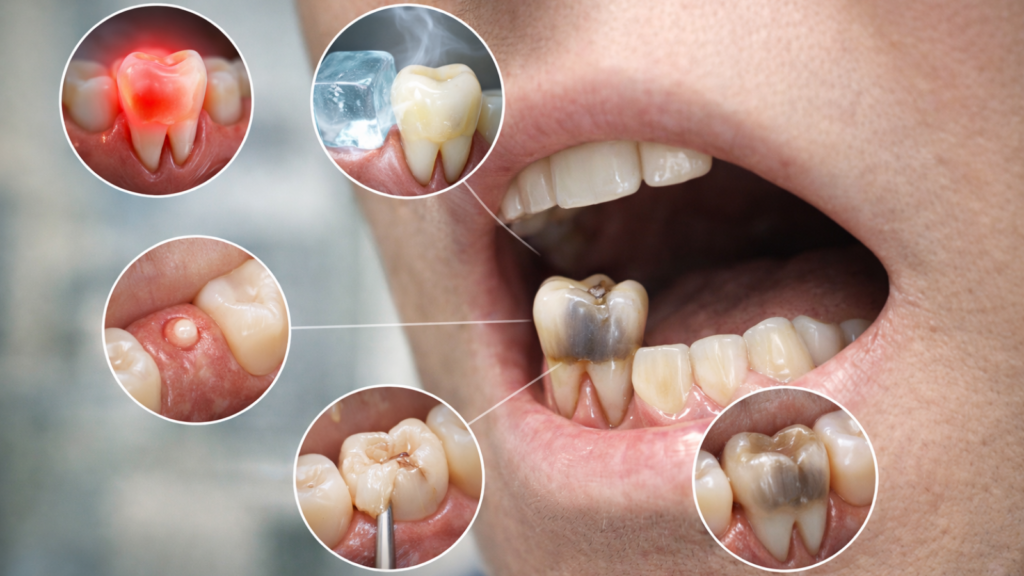
Five distinct warning signs indicate your tooth may require root canal therapy to prevent serious complications. These symptoms, persistent toothache, lingering temperature sensitivity, biting pain, gum pustules, and tooth discolouration, signal pulp infection or damage needing professional evaluation. Learning to recognise these red flags empowers you to seek timely treatment, potentially saving your natural tooth before irreversible damage occurs.
1. Severe or Persistent Toothache: When Pain Becomes a Red Flag
Constant, throbbing tooth pain that persists for days or weeks signals potential pulp infection requiring immediate attention. Unlike minor sensitivity that fades quickly, this pain feels intense, pulsating, and may radiate to your jaw, ear, or face. You might experience sharp shooting sensations when biting down or dull, continuous aching that disrupts sleep.
Pain relievers provide temporary relief but never eliminate underlying infection, which continues worsening beneath the surface. Some patients notice pain fluctuating in intensity yet never completely disappearing, indicating ongoing inflammation. Discomfort that awakens you at night or intensifies when lying down suggests advanced infection needing urgent evaluation.
Inflamed or infected pulp tissue sends distress signals through nerve pathways, creating that characteristic throbbing sensation. Ignoring persistent dental pain allows bacteria to spread beyond tooth roots into surrounding bone and gum tissue. Scheduling prompt dental examination prevents complications and addresses infection at its source.
2. Lingering Sensitivity to Hot or Cold (Not Quick to Subside)
Brief sensitivity to temperature changes is common, but prolonged discomfort lasting minutes after exposure indicates nerve damage. Healthy teeth may react momentarily to ice cream or hot tea, yet pain disappears within seconds. When sensitivity lingers significantly after removing cold or hot stimulus, damaged or inflamed pulp tissue cannot regulate responses properly.
Sharp, intense pain from mildly warm beverages or cool air suggests nerve exposure or advanced irritation. This prolonged reaction occurs because injured pulp nerves overcompensate, sending exaggerated pain signals long after temperature change ends. Some patients find even room-temperature foods trigger uncomfortable sensations that persist unnaturally.
Early-stage nerve damage often manifests through lingering temperature sensitivity before other symptoms appear. Teeth with large fillings or visible decay commonly develop this symptom as infection approaches pulp chambers. Addressing this warning sign promptly may prevent full-blown infection and preserve more healthy tooth structure.
3. Pain When Biting or Chewing (Localised Pressure Pain)
Discomfort specifically when applying pressure while chewing indicates possible crack, advanced decay, or root infection. Healthy teeth handle normal biting forces without pain, but infected or damaged teeth respond with sharp, localised sensations. You might avoid chewing on one side because certain teeth cause stabbing pain under pressure.
This symptom develops when infection spreads to tissues surrounding root tips, making tooth roots tender and inflamed. Microscopic cracks extending toward pulp chambers allow bacteria entry while causing pain during mechanical stress. Some patients describe feeling like something sharp pokes them each time they bite down.
Ligaments holding teeth in jaw sockets become irritated when infection leaks from root canals into bone. Pressure-related pain may start mild but typically worsens as infection progresses deeper. Dental evaluation can determine whether pain stems from cracked tooth, pulp infection, or other treatable conditions.
4. A Pimple/Blister on Gum or Pus Drainage (Sign of Abscess)
Small, pimple-like bumps appearing on gums near affected teeth indicate bacterial infection draining from tooth roots. These pustules, called dental abscesses, contain accumulated pus and bacteria seeking exit pathways through gum tissue. You might notice recurring swelling that occasionally bursts, releasing foul-tasting fluid before refilling.
Gum swelling, redness, or tenderness around specific teeth signals infection spreading beyond root canals into surrounding structures. Some patients experience persistent bad taste or odour when abscesses drain into mouths intermittently. Facial swelling, tender lymph nodes under jaw, or fever accompanying gum pustules require immediate dental attention.
Abscesses form when body attempts containing infection, but cannot eliminate bacteria trapped inside sealed tooth roots. Untreated abscesses can cause bone loss, spread to facial spaces, or rarely enter bloodstream causing serious illness. Root canal treatment removes infected pulp tissue, eliminating bacterial source and allowing proper healing.
5. Tooth Darkening or Visible Discoloration
Teeth suddenly turning grey, brown, or darker than neighbours often indicate internal pulp death or bleeding. Healthy pulp tissue maintains tooth vitality, but dying nerves and blood vessels cause discolouration from inside outward. This change differs from surface staining; darkness originates deep within tooth structure.
Trauma, even without visible cracks, can bruise pulp tissue internally, leading to gradual darkening over weeks or months. Dead pulp tissue undergoes breakdown, releasing pigments that permeate dentin and alter tooth appearance permanently. Single darkened teeth among otherwise white teeth almost always signal internal damage requiring investigation.
Some patients notice discolouration following old injuries they dismissed years ago, unaware pulp slowly died meanwhile. Darkening may precede pain symptoms, appearing first as subtle shade changes progressing to obvious grey tones. Dentists check colour changes during examinations because early detection enables intervention before infection establishes.
What Each Sign Actually Means (Clinical Explanation)
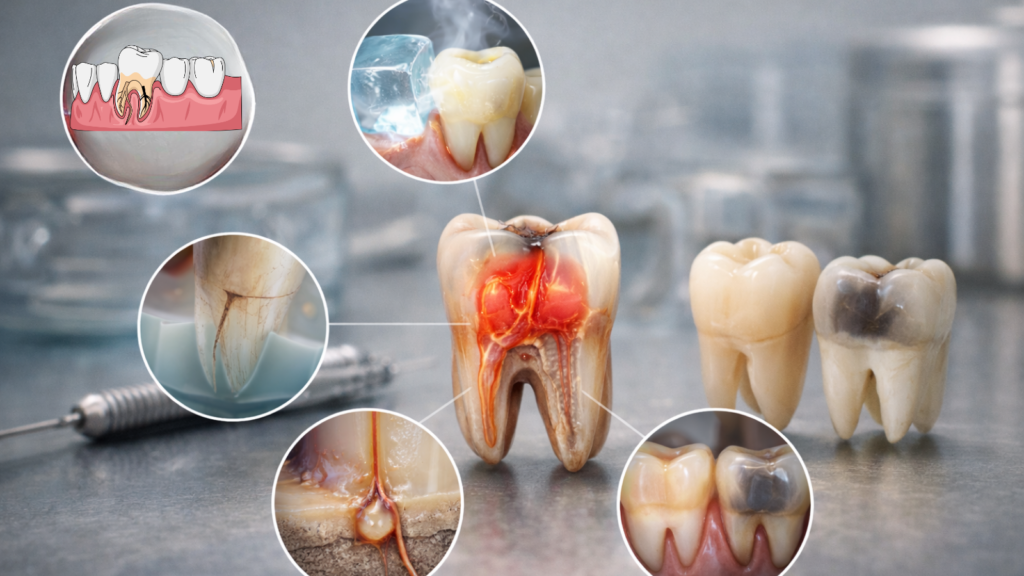
Understanding the biological mechanisms behind root canal symptoms helps you appreciate why prompt treatment matters so critically. Each warning sign reflects specific stages of pulp inflammation, infection, or death occurring deep within your tooth structure. Scientific knowledge of these processes reveals how seemingly minor symptoms can indicate serious underlying problems requiring immediate dental intervention.
Why Persistent Toothache Signals Pulp Inflammation or Infection
Dental pulp contains abundant nerve fibres that detect damage and transmit pain signals to your brain. Inflammation from bacterial invasion irritates these nerves, causing continuous firing that manifests as throbbing, persistent ache. Blood vessels within pulp tissue dilate during infection, increasing internal pressure against unyielding tooth walls.
This confined swelling creates intense, pulsating pain because inflamed tissue cannot expand outward through hard enamel and dentin. Nerve endings become hypersensitive, responding excessively to stimuli that normally cause no discomfort whatsoever. Chemical mediators released during infection amplify pain perception, explaining why dental pain feels particularly severe.
Persistent pain indicates infection has progressed beyond reversible inflammation into irreversible pulp damage requiring removal. Bacteria produce toxins that directly damage nerve tissue, causing spontaneous pain even without external triggers. Understanding pain mechanisms helps patients recognise symptoms warranting urgent professional evaluation rather than self-medication.
Biology Behind Lingering Temperature Sensitivity
Healthy pulp tissue regulates temperature through adequate blood flow and intact nerve responses, returning to baseline quickly. Damaged or inflamed pulp loses regulatory capacity, causing nerves to misinterpret harmless temperature changes as threats. Prolonged sensitivity occurs because injured nerves remain activated long after stimulus removal.
Exposed dentinal tubules, tiny channels connecting outer tooth to inner pulp, transmit temperature directly to already-irritated nerves. Inflammation causes nerve fibres to develop spontaneous activity and lower activation thresholds, overreacting to minor stimuli. Blood flow changes within infected pulp tissue amplify temperature transmission rather than buffering it properly.
This symptom often represents transitional stage between reversible irritation and complete nerve death needing root canal. Early intervention during lingering sensitivity phase may preserve some pulp vitality in certain cases. Ignoring symptom allows infection to progress, ultimately killing nerve tissue entirely and requiring complete pulp removal.
Biting Pain: Cracked Tooth, Occlusion or Root Involvement?
Pain when biting indicates mechanical forces transmitting through damaged tooth structure to sensitive underlying tissues or exposed nerves. Cracks act like wedges, flexing tooth segments apart during pressure application and stimulating nerve endings directly. Infected pulp extending into root canal system makes surrounding periodontal ligament inflamed and tender.
Occlusal trauma from high fillings or misaligned bite forces concentrates stress on specific teeth, potentially causing pulp inflammation. Bacteria from infected pulp canals leak through root apex (tip) into bone, creating painful inflammatory response. Biting pressure compresses already-inflamed tissues around root tips, generating sharp, localised discomfort.
Distinguishing crack-related pain from infection requires professional diagnostic testing including percussion tests and X-ray imaging. Some cracked or chipped teeth remain superficial, treatable with bonding or crowns without needing root canal therapy. Advanced cracks extending into the pulp chamber or infected roots necessitate endodontic treatment followed by crown placement.
Gum Pustules and Swelling: How Infections Track Out of Root
Bacterial infection confined within root canal system seeks exit when pressure builds from accumulated pus and debris. Bacteria and toxins travel through root apex into surrounding bone, establishing infection in jawbone tissue. Body’s immune response attempts containing infection, forming abscess, a walled-off pocket of pus.
Abscesses follow paths of least resistance, often tracking through bone to reach gum surface where they form visible pustules. Gingival tissue swells, reddens, and softens as abscess approaches surface, eventually creating draining fistula tract. Drainage provides temporary pressure relief but does not eliminate infection source inside tooth.
Chronic draining abscesses cause progressive bone loss around tooth roots, potentially leading to tooth mobility and eventual loss. Facial swelling occurs when infection spreads beyond local area into facial tissue planes, representing serious complication. Root canal treatment removes infected pulp tissue, eliminating bacterial source and allowing bone and gum tissue to heal properly.
Discoloration: Dead Nerve vs External Staining: How to Tell
Internal discolouration originates from breakdown products of dying pulp tissue, blood pigments, or bacterial by-products infiltrating dentin. External staining from coffee, tea, or tobacco affects only enamel surface and responds to professional cleaning. Internal darkening appears as grey, purple-brown, or black tones emanating from within tooth structure.
Dead nerve tissue undergoes decomposition, releasing haemoglobin breakdown products that permanently discolour internal dentin layers. Trauma-induced bleeding into pulp chamber leaves iron deposits that darken tooth over time as blood breaks down. External stains appear uniform across multiple teeth, while internal discolouration typically affects single traumatised or infected tooth.
Dentists differentiate causes using transillumination (shining light through tooth) and X-ray examination revealing pulp chamber changes. Internal discolouration may precede other symptoms by months, representing early warning of pulp death. While cosmetic concern motivates some patients, discolouration primarily signals need for endodontic evaluation and potential treatment.
Take Action for Your Dental Health
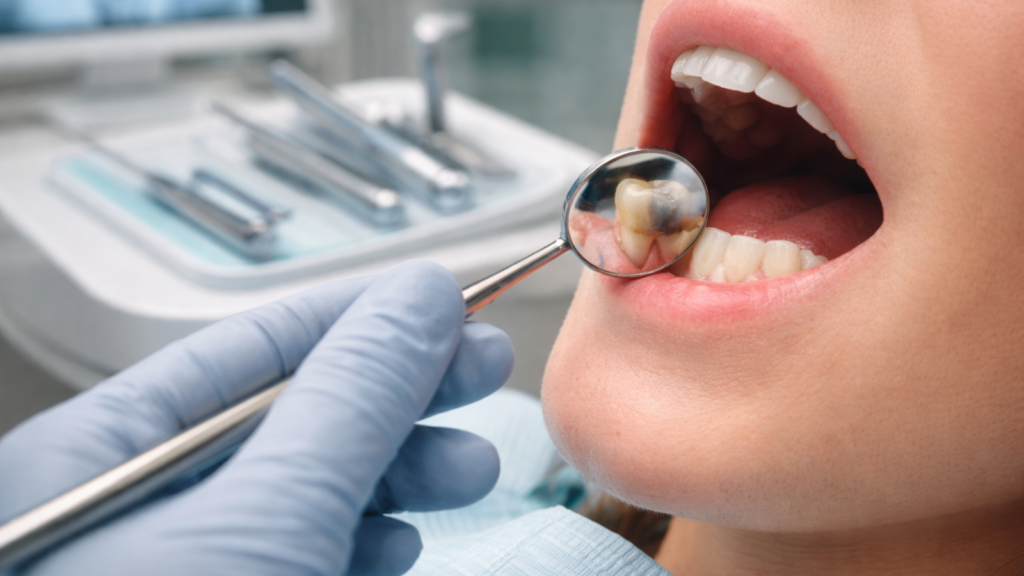
Recognising the top 5 signs you need a root canal empowers you to seek timely treatment and save your natural tooth. Persistent toothache may come from decay, cracks, gum issues, or infection, this quick guide to finding the cause of tooth pain can help you understand what’s likely happening. Lingering temperature sensitivity, biting pain, gum swelling with pustules, and tooth discolouration all warrant immediate dental evaluation. Modern root canal therapy has become routine, comfortable, and highly successful at eliminating infection while preserving your smile.
Delaying treatment only allows infection to worsen, potentially causing tooth loss, bone damage, and serious health complications. Dental technology and techniques available in Kathmandu match international standards, offering effective, affordable root canal solutions. Your natural teeth provide irreplaceable function and maintain jaw structure better than any artificial replacement.
If you are experiencing any symptoms discussed in this guide, visiting a qualified dental in Kathmandu can help prevent further complications and save your natural tooth. Early intervention makes treatment simpler, more comfortable, and significantly increases long-term success rates. Schedule your dental examination today, protecting your oral health is an investment in your overall wellbeing.
How much does root canal treatment cost in Kathmandu?
Root canal costs in Kathmandu vary depending on tooth location (front teeth versus molars) and clinic standards. Prices typically range from NPR 8,000 to NPR 25,000, with specialist endodontists charging higher fees. Most clinics offer instalment payment options, and dental insurance plans often cover 50-80% of treatment expenses.
Can root canal treatment be completed in one visit?
Many modern Kathmandu dental clinics complete uncomplicated root canals in single appointments lasting 60-90 minutes. Complex cases involving severe infection or difficult anatomy may require 2-3 visits for optimal results. Your dentist will assess infection severity and recommend appropriate treatment timeline during initial examination.
Will root canal treatment hurt during the procedure?
Modern local anaesthesia makes root canal therapy comfortable and virtually painless during treatment itself. Patients typically experience pressure sensations but no sharp pain while dentist works on the tooth; this root canal pain and recovery guide explains what’s normal. Most discomfort comes from pre-existing infection; treatment actually relieves pain by removing infected tissue.
How long does recovery take after root canal?
Recovery following root canal treatment is usually quick, with mild soreness lasting 1-3 days. Over-the-counter pain relievers manage any post-treatment discomfort effectively for most patients. Normal eating and daily activities resume immediately after numbness wears off, though avoiding very hard foods on treated tooth for few days is wise.
Do all teeth need crowns after root canal?
Back teeth (molars and premolars) almost always require crowns after root canal because chewing forces can fracture weakened tooth structure. Front teeth with minimal damage may need only filling restoration if sufficient tooth structure remains. Your dentist will recommend crown placement based on remaining tooth strength and location.
Can infection return after root canal treatment?
Properly performed root canals have 85-95% success rates with infection eliminated permanently. Rare failures occur if bacteria remain in complex canal anatomy or tooth fractures later allowing reinfection. Maintaining good oral hygiene and regular dental check-ups minimises reinfection risk.
What happens if infection spreads before treatment?
Untreated tooth infections can spread to surrounding teeth, jawbone, and facial tissues causing serious complications, learn the tooth abscess danger signs and urgent treatment steps to know when it’s an emergency. Severe cases may cause facial swelling, fever, difficulty swallowing, or breathing problems requiring emergency treatment. Systemic infections, though rare, can occur when bacteria enter bloodstream from dental abscesses.
Are there alternatives to root canal treatment?
Extraction remains the only alternative when pulp tissue is infected beyond saving. However, tooth extraction leads to bone loss, neighbouring tooth shifting, and requires costly replacement options. Dental implants or bridges cost significantly more than root canal treatment while compromising adjacent healthy teeth.
How can you prevent needing root canal?
Maintaining excellent oral hygiene through twice-daily brushing and daily flossing prevents most cavity-related infections. Regular dental check-ups every six months catch problems early before they reach pulp tissue. Wearing mouthguards during sports, avoiding chewing hard objects, and treating cavities promptly reduces root canal risk significantly.
What should you do if experiencing these symptoms in Kathmandu?
Contact your dentist immediately for proper examination and diagnosis using clinical tests and X-rays. Many dental clinics in Kathmandu offer emergency appointments for severe pain or swelling. Early professional evaluation prevents complications and increases treatment success rates while preserving your natural tooth.
