Sensitive teeth can turn simple everyday moments like sipping hot tea or drinking cold water into a sudden sharp “zing” that makes you pause. This hot/cold sensitivity usually happens when the tooth’s protective enamel wears down or the gums recede and expose the more vulneraiately or within seconds after you remove the trigger, while toothache pain persists and often worsens over time. This distinction helps you decide whether home treatment willble root surface. The good news is that most cases improve a lot once you identify the cause and use the right treatment consistently.
In this guide, you’ll learn the most common reasons teeth become sensitive, how to tell if it’s normal sensitivity or a sign of a bigger problem, and what actually works at home. We’ll also cover dentist treatments that fix the root cause, not just the symptoms, plus clear red flags that mean you should book a checkup sooner. By the end, you’ll have a simple plan to reduce sensitivity and prevent it from coming back.
Sensitive Teeth Basics: What It Is and What It’s Not

Sensitive teeth usually feel like a sudden, sharp “zing” when you drink something cold or hot, and it often happens when enamel is worn or the root surface is exposed. Cold, hot, sweet, sour, and even cold air can trigger it, so noticing your specific trigger helps narrow the cause. If the pain lingers for minutes or wakes you up at night, it may be more than simple sensitivity and needs a dental check.
What Tooth Sensitivity Feels Like (Short Sharp vs Lingering Pain)
Tooth sensitivity produces a quick, sharp jolt that disappears within 5 to 10 seconds after removing the trigger. You feel the sting immediately when cold air hits your teeth or when you take a sip of something hot. The pain stays localized to the tooth surface and does not spread to your jaw or surrounding areas.
Lingering pain tells a different story. The discomfort continues for 30 seconds to several minutes after you remove the trigger, which suggests deeper dental problems rather than simple sensitivity. Your tooth may throb or ache even after you finish drinking your cold beverage.
Trigger Map: Cold, Hot, Sweet, Sour/Acidic, Cold Air; What Each Can Suggest
Different triggers point to specific dental conditions:
- Cold sensitivity indicates exposed dentin from enamel wear or gum recession. Your teeth react because cold temperatures reach the nerve endings in the dentin tubules directly.
- Hot sensitivity often signals more serious issues like deep decay or an inflamed nerve (pulpitis). Teeth rarely develop isolated hot sensitivity from simple enamel wear.
- Sweet and sour/acidic reactions suggest active enamel erosion or existing cavities. Sugar and acid reach the dentin layer through weak spots in your enamel, triggering immediate discomfort.
- Cold air sensitivity happens when gum recession exposes root surfaces. The roots lack the protective enamel layer that covers tooth crowns, making them extremely reactive to temperature changes and airflow.
Multiple trigger types affecting the same tooth usually mean you need professional treatment beyond desensitizing toothpaste.
Why It Happens (Simple Dentin/Enamel Explanation)
The outer enamel layer protects the inner dentin, which contains thousands of microscopic tubules connected to your tooth nerve. Enamel has no nerve endings and blocks external stimuli from reaching the sensitive dentin underneath.
Dentin exposure occurs through 2 main pathways:
- Firstly, enamel wears down from acid erosion, grinding, or aggressive brushing, allowing hot and cold to penetrate the tubules.
- Secondly, gums recede from the tooth surface, exposing the root portion that has only a thin cementum layer instead of thick enamel.
The tubules act like tiny straws leading directly to the nerve. Temperature changes, sweet substances, and acidic foods travel through these channels and stimulate the nerve, creating that characteristic sharp pain.
Sensitivity vs Toothache: Quick Patterns That Point to Decay or Nerve Pain
Sensitivity pain stops immediately or within seconds after you remove the trigger, while persistent tooth pain persists and often worsens over time. This distinction helps you decide whether home treatment will work or whether you need urgent dental care.
Patterns suggesting simple sensitivity:
- Pain affects multiple teeth
- Discomfort stops the moment you stop eating or drinking
- No spontaneous pain when you are doing nothing
- Relief comes from warm water or avoiding triggers
Patterns indicating decay or nerve damage:
- Only one tooth hurts
- Pain wakes you from sleep
- Discomfort continues for minutes after removing the trigger
- Heat makes it worse; cold sometimes provides brief relief
- You notice swelling, bad taste, or visible damage
The one-tooth rule applies here: sensitivity affecting a single tooth for more than 2 weeks requires professional examination because it rarely results from simple enamel wear.
Common Causes of Hot/Cold Sensitivity (With Fast Self-Clues)
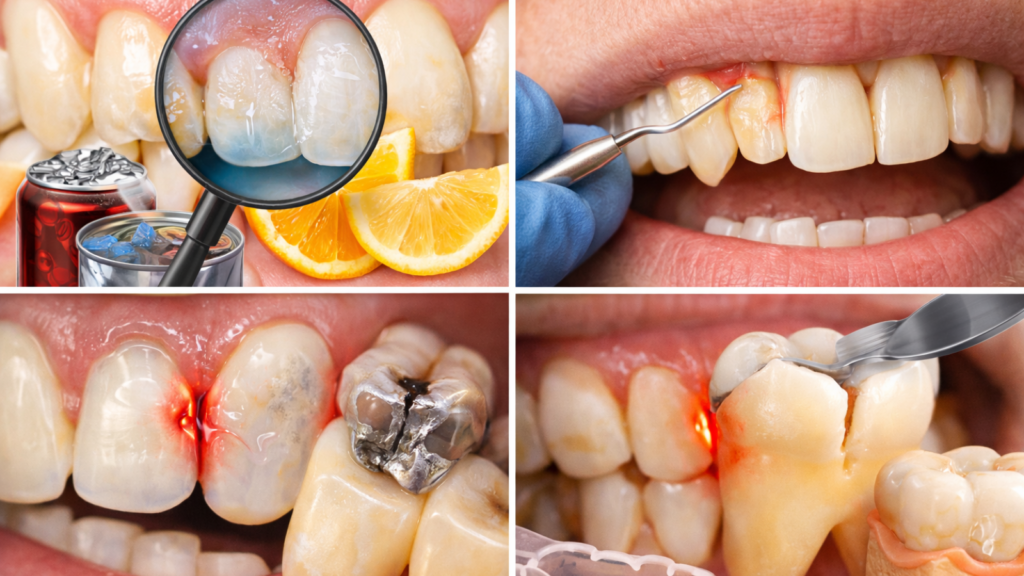
The most common causes include enamel erosion from acidic foods/drinks, gum recession that exposes the root, and tiny cracks or worn fillings that let temperature reach the sensitive inner layer. Sensitivity in many teeth often points to enamel wear or gum recession, while sensitivity in one tooth can suggest a cavity, crack, or leaking filling. Grinding/clenching can also create microscopic damage and make sensitivity worse over time.
1. Enamel Wear and Acid Erosion (Diet, Frequent Snacking, Acidic Drinks)
Dietary acids dissolve the mineral content of enamel faster than your saliva can repair it, gradually thinning the protective layer until dentin becomes exposed. This process happens slowly over months or years, making it easy to miss until sensitivity develops.
Common dietary culprits in Kathmandu include:
- Lemon water consumed first thing in the morning on an empty stomach
- Multiple cups of black tea throughout the day (tannins create acidic environment)
- Frequent consumption of achar (pickles) and citrus-based chutneys
- Soft drinks and packaged fruit juices
- Tomato-based curries eaten daily
Frequent snacking creates repeated acid attacks. Your mouth needs 30 to 60 minutes to neutralize acid and remineralize enamel after eating. Snacking every hour prevents this recovery cycle, keeping your teeth in constant demineralization mode.
Self-check clues: Your front teeth may appear slightly translucent at the edges, or you notice increased sensitivity to cold that started gradually and now affects several teeth at once.
2. Gum Recession Exposing Roots (Why Roots Feel Extra Sensitive)
Root surfaces lack the thick enamel protection that covers tooth crowns, making them 7 to 8 times more vulnerable to sensitivity triggers. The roots have only a thin cementum layer, and dentin tubules sit much closer to the surface.
Recession develops from:
- Hard horizontal brushing with medium or firm bristles
- Inadequate brushing allowing plaque buildup and gum inflammation
- Grinding teeth at night (puts pressure on gum attachment)
- Genetic thin gum tissue
- Tobacco use
You notice recession when:
- The yellow root portion becomes visible above the gum line
- Teeth appear longer than they used to
- Sensitivity occurs specifically near the gum line
- One side of your mouth (your brushing side) shows more sensitivity than the other
Recession rarely reverses on its own. The exposed root will remain sensitive until you either modify your triggers or get professional treatment to cover the area.
3. Cavities, Leaking Fillings, and Worn Restorations (Why One Tooth May Flare Up)
Decay creates pathways through enamel directly to the dentin and nerve, allowing temperature and food particles to reach sensitive areas immediately. This explains why cavity-related sensitivity affects only one tooth rather than multiple teeth at once.
Leaking fillings develop gaps between the filling material and tooth structure over time. Food, bacteria, and temperature changes seep through these microscopic gaps and irritate the nerve underneath the restoration.
Warning signs that point to decay or failing restorations:
- Sudden sensitivity in a tooth that was previously fine
- Sweet foods trigger immediate, sharp pain in that specific tooth
- You see visible brown or gray spots, or the filling looks discolored around edges
- Floss catches or shreds at the same spot consistently
- Sensitivity has progressed from mild to severe over 2 to 4 weeks
Old fillings (5+ years) and large restorations face higher failure rates. The filling material shrinks slightly over time, creating microscopic gaps even when the restoration looks intact from the outside.
4. Cracked Tooth and Grinding (Sharp Pain on Bite, “Zinger” With Cold)
Tooth cracks allow fluid movement inside the dentin tubules when you bite down, creating sudden sharp pain that feels like an electric shock. The crack may be invisible to the naked eye but deep enough to reach the dentin layer.
Grinding (bruxism) creates both direct cracks and enamel wear. People often grind hardest on their back molars and canines, which explains why these teeth show sensitivity first.
Self-assessment for cracks and grinding:
- Pain occurs specifically when you bite down on that tooth or release pressure
- Cold liquids create an intense “zinger” sensation that makes you flinch
- You wake up with jaw soreness or tight facial muscles
- Your partner hears grinding sounds at night
- The biting surfaces look flat or worn compared to other teeth
Cracks require professional diagnosis because they rarely show on X-rays until they become severe. Cracked tooth treatment involves special lights, dyes, or bite tests to locate the crack and determine the best repair option.
Untreated cracks worsen over time. The crack propagates deeper into the tooth structure, eventually reaching the nerve chamber and requiring root canal treatment or extraction.
Special Situations People Search For
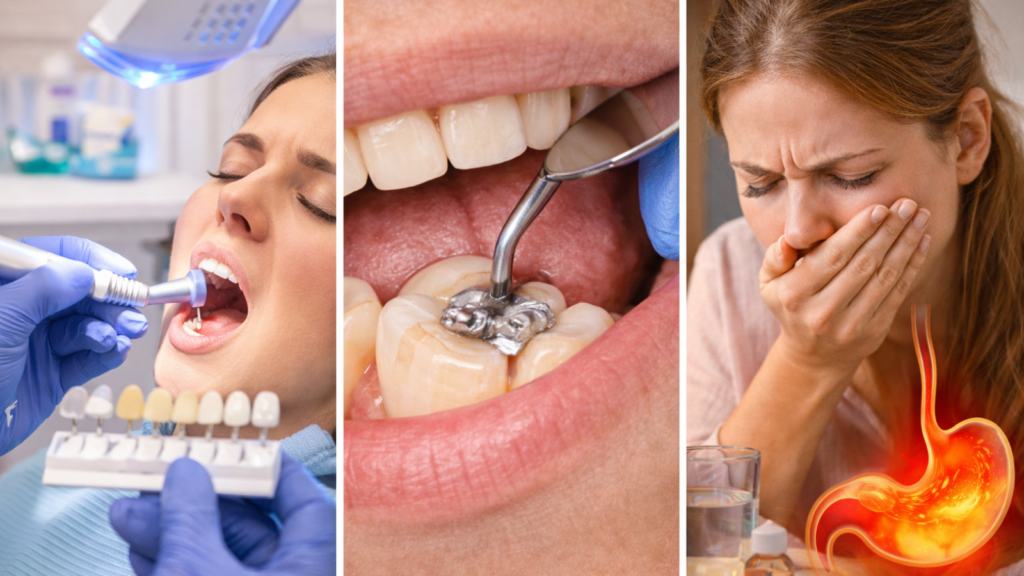
Some people notice sensitivity after a dental cleaning, whitening, or a new filling because the tooth and gums may be temporarily irritated or adjusting. This is often short-term, but if the bite feels “high” after a filling or the sensitivity keeps getting worse, it may need an adjustment or further evaluation. Reflux/GERD and frequent vomiting can silently erode enamel, so recurring sensitivity with acid symptoms is a key clue.
Sensitive After Cleaning/Scaling: What’s Normal and How Long It Lasts
Sensitivity after professional cleaning occurs because the dentist removes plaque and calculus deposits that were covering and insulating exposed root surfaces. Your teeth feel more sensitive temporarily as the newly cleaned surfaces adjust to direct contact with temperature and air.
Normal post-cleaning sensitivity:
- Affects multiple teeth, especially around the gum line
- Peaks within 24 to 48 hours after treatment
- Gradually improves over 3 to 7 days
- Responds well to sensitivity toothpaste
- Creates discomfort mainly with cold, not heat
The sensitivity timeline depends on the amount of calculus removed. Heavy calculus removal (often during first deep cleaning in years) causes more temporary sensitivity than routine 6-month cleanings with minimal buildup.
You can minimize discomfort by using sensitivity toothpaste for 2 weeks before your scheduled cleaning appointment. The active ingredients build protection in exposed tubules before the cleaning exposes them further.
Contact your dentist within 48 hours if the sensitivity becomes severe, affects only one tooth, or continues worsening past day 3. This pattern suggests the cleaning revealed an underlying problem like a crack or cavity rather than simple post-treatment sensitivity.
Sensitive After Fillings/Crowns: Bite Issues, Pulp Irritation, or Leakage; When to Return
New restorations can cause sensitivity for 2 to 6 weeks as the tooth nerve calms down from the drilling and preparation process. The nerve becomes inflamed (reversible pulpitis) from the mechanical trauma but usually heals without intervention.
Three distinct causes create post-restoration sensitivity:
High bite (most common): The new filling or crown sits slightly taller than your natural bite, creating concentrated pressure when you chew. The tooth feels sore and sensitive to biting, and cold sensitivity may develop from the constant pressure.
Pulp irritation: Deep cavities require drilling close to the nerve chamber. The heat, vibration, and proximity to the nerve cause temporary inflammation that makes the tooth reactive to temperature for several weeks.
Leakage or gap: The restoration may have a microscopic gap allowing bacteria or fluid to seep underneath. This creates persistent sensitivity that often worsens over time rather than improving.
Return to your dentist within 1 week if:
- The tooth hurts when you bite down (high bite needs adjustment)
- Hot beverages cause significant pain (suggests deep nerve irritation)
- Sensitivity increases past week 2 instead of improving
- You notice swelling or bad taste around the restoration
Most post-filling sensitivity resolves within 4 weeks. Sensitivity lasting beyond 6 weeks suggests the nerve may not recover and could require root canal treatment.
Sensitive After Whitening/Toothpastes: Common Irritants and What to Pause
Professional teeth whitening in Kathmandu temporarily dehydrates tooth enamel and increases fluid movement within dentin tubules, creating sensitivity that peaks 24 to 48 hours after treatment. The peroxide ingredient penetrates enamel to bleach internal stains, but this penetration pathway also allows temperature stimuli to reach the nerve more easily.
Post-whitening sensitivity:
- Affects all treated teeth equally
- Reaches maximum intensity on day 2
- Resolves completely within 2 to 5 days
- Responds well to fluoride treatments and sensitivity toothpaste
- Does not indicate permanent damage
You reduce whitening sensitivity by:
- Using the whitening product for shorter duration (30 minutes instead of 60 minutes)
- Taking a 1-day break between whitening sessions
- Applying sensitivity toothpaste to teeth before placing the whitening tray
- Avoiding extremely cold or hot foods during the whitening period
Certain whitening toothpastes contain abrasive particles that mechanically remove surface enamel along with stains. Daily use over months can thin enamel enough to cause persistent sensitivity. You notice this pattern when sensitivity developed gradually during consistent use of whitening toothpaste but improves when you switch to regular toothpaste.
Pause whitening immediately if pain persists beyond 5 days after stopping treatment or if sensitivity affects only one or two teeth rather than all whitened teeth (suggests underlying dental problem).
Reflux/GERD or Vomiting: How Stomach Acid Drives Sensitivity and Safe Immediate Steps
Stomach acid (pH 1.5 to 2) dissolves tooth enamel significantly faster than any food or beverage acid, creating severe sensitivity patterns that affect the tongue-side surfaces of upper front teeth first. Repeated acid exposure from reflux or vomiting creates characteristic erosion patterns that dentists recognize immediately.
Acid reflux damage differs from dietary erosion:
- Affects inside (tongue-side) surfaces more than outside (lip-side) surfaces
- Creates smooth, scooped-out areas on back teeth
- Causes widespread sensitivity across many teeth simultaneously
- Often includes sour taste in mouth upon waking or after lying down
Immediate protective steps after acid exposure:
- Rinse mouth with plain water or baking soda solution (1 teaspoon in 8 ounces water) to neutralize acid
- Wait 60 minutes before brushing (acid-softened enamel brushes away easily)
- Chew sugar-free gum to stimulate protective saliva flow
- Use prescription-strength fluoride toothpaste if recommended by your dentist
You need medical treatment for the underlying reflux problem, not just dental repair. Enamel erosion from acid reflux is a deeper problem than it appears, treating sensitivity symptoms without controlling acid exposure leads to progressive enamel loss and eventual tooth structure failure.
Sleep position modifications help reduce nighttime acid exposure: elevate the head of your bed by 15 to 20 centimeters, avoid eating 3 hours before sleep, and sleep on your left side rather than right side (reduces lower esophageal sphincter relaxation).
Best At-Home Treatments (What Works and How to Use It Correctly)

Start with a sensitivity toothpaste used consistently, because it helps block pain signals or seal exposed dentin over time rather than instantly. Switch to a soft toothbrush, lighten your brushing pressure, and avoid brushing right after acidic foods, rinse with water first and wait before brushing. Limit acidic snacks/drinks, avoid harsh whitening products if they flare symptoms, and track whether the problem is improving within 2–4 weeks.
Choosing Sensitivity Toothpaste by Ingredient (Stannous Fluoride, Potassium Salts, Arginine, Etc.)
Sensitivity toothpastes work through 2 distinct mechanisms: nerve desensitization (potassium compounds) or tubule blocking (stannous fluoride, arginine, calcium compounds). Understanding which ingredient matches your sensitivity type helps you select the most effective product.
Potassium nitrate (5% to 8%):
- Calms nerve response to stimuli
- Requires 2 to 4 weeks of consistent use
- Works best for general temperature sensitivity affecting multiple teeth
- Does not repair enamel or block tubules
Stannous fluoride (0.454%):
- Forms protective layer over exposed tubules
- Provides both sensitivity relief and cavity protection
- Shows improvement within 1 to 2 weeks
- May cause temporary tooth staining in some users
Arginine (8%) with calcium carbonate:
- Plugs tubules with calcium-based deposits
- Creates physical barrier against triggers
- Shows faster relief (within 3 to 7 days)
- Works particularly well for root sensitivity
Nano-hydroxyapatite:
- Rebuilds enamel mineral structure
- Fills surface defects and early erosion
- Popular in Asian markets; limited availability in Nepal currently
Most people in Kathmandu find products containing either potassium nitrate or stannous fluoride readily available at pharmacies. Products with arginine technology are becoming more common but may cost 20% to 30% more than standard sensitivity formulas.
Switch products after 6 weeks if you notice no improvement. Different mechanisms work better for different people based on their specific cause of sensitivity.
How to Use It for Best Results (Timeline and “Spot Application” Technique)
Standard brushing with sensitivity toothpaste provides minimal benefit compared to targeted application directly onto sensitive areas. The active ingredients need extended contact time with exposed dentin to create the protective barrier.
Optimal application protocol:
- Brush normally with sensitivity toothpaste twice daily
- After evening brushing, apply pea-sized amount directly to sensitive spots with clean fingertip
- Rub gently in circular motion for 60 seconds
- Leave overnight without rinsing
- Avoid eating or drinking for 30 minutes after application
The spot-application technique delivers concentrated active ingredients to problem areas and allows 6 to 8 hours of contact time overnight. Standard 2-minute brushing provides only brief exposure, limiting ingredient effectiveness.
Realistic timelines:
- Days 1 to 7: Minimal change; continue consistent use
- Days 7 to 14: Slight reduction in sensitivity to triggers
- Days 14 to 28: Noticeable improvement; most triggers become tolerable
- Days 28+: Maximum benefit achieved; maintenance use prevents return
You need continuous use to maintain results. Sensitivity returns within 2 to 3 weeks after stopping sensitivity toothpaste because the protective barriers gradually wear away from normal eating and drinking.
Track your improvement by testing the same trigger (specific cold beverage) weekly. Subjective improvement assessment helps you determine whether the product works or whether you need to try a different ingredient or seek professional treatment.
Fluoride at Home: When a Dentist May Suggest Higher-Fluoride Options
Standard toothpaste contains 1000 to 1450 ppm (parts per million) fluoride, while prescription-strength options provide 5000 ppm for enhanced remineralization of weakened enamel. Dentists prescribe high-fluoride toothpaste when sensitivity stems from active enamel erosion or early decay rather than simple tubule exposure.
Prescription fluoride indications:
- Widespread sensitivity across many teeth from acid erosion
- Visible white spot lesions (early decay) combined with sensitivity
- High cavity risk from dry mouth or medical conditions
- Sensitivity during active orthodontic treatment
- Post-whitening sensitivity management
High-fluoride toothpaste rebuilds the mineral structure of demineralized enamel, making it more resistant to acid attack and reducing tubule permeability. This differs from desensitizing ingredients that only block tubules or calm nerves without addressing the structural weakness.
Proper high-fluoride use:
- Apply only at night before sleep
- Use small pea-sized amount
- Brush for 2 minutes then spit (do not rinse)
- Avoid eating or drinking for 30 minutes minimum
- Continue regular fluoride toothpaste in morning
High-fluoride products require prescription in most markets including Nepal. Some brands available in Kathmandu pharmacies include Colgate Prevident 5000 and Clinpro 5000 (availability varies).
Fluoride supplements (drops or tablets) work poorly for topical sensitivity because they provide systemic fluoride during tooth development rather than surface protection for existing sensitivity. Topical application delivers the concentrated dose directly where you need it.
Brush Smarter: Soft Brush, Gentle Pressure, and Wait 30–60 Minutes After Acidic Foods
Aggressive brushing removes more enamel and gum tissue than plaque, making it the leading preventable cause of sensitivity in people who maintain good oral hygiene. The mechanical damage from hard bristles and excessive pressure outweighs any cleaning benefit.
Brushing damage patterns:
- Wedge-shaped grooves at the gum line (abrasion notches)
- Sensitivity concentrated on the cheek side of teeth (your brushing hand side)
- Gum recession on canines and premolars (teeth that stick out more)
- Shiny, smooth root surfaces from mechanical wear
Proper brushing technique for sensitive teeth:
- Use only soft or extra-soft bristles
- Hold brush with fingertip grip (not fist grip) to reduce pressure
- Angle bristles 45 degrees toward gum line
- Use gentle circular or vibrating motion instead of back-and-forth sawing
- Let the bristle tips do the work; pressing harder does not clean better
The 30 to 60 minute waiting rule after acidic exposure prevents you from brushing away acid-softened enamel. Acid temporarily demineralizes the surface layer, making it vulnerable to mechanical removal. Your saliva needs time to neutralize the acid and re-harden the surface.
Post-acid protocol:
- Rinse immediately with water
- Chew sugar-free gum to boost saliva
- Wait minimum 30 minutes (60 minutes is better) before brushing
- If you must clean teeth sooner, rinse thoroughly rather than brushing
People who brush immediately after morning lemon water or after vomiting remove significantly more enamel over time compared to those who wait the recommended period. This single timing change can prevent years of progressive enamel wear.
Electric toothbrushes with pressure sensors help people who struggle with manual brush pressure control. The brush stops or signals when you press too hard, providing immediate feedback.
Dentist Treatments That Fix the Root Cause (Not Just Symptoms)
A dentist will identify the real cause using a focused exam, possible X-rays, and tests for cracks, gum recession, or bite problems. In-clinic options like fluoride varnish, desensitizing agents, or bonding/sealants can protect exposed areas and reduce sensitivity quickly. If sensitivity is due to decay, a crack, or a failing filling, restoring the tooth (or addressing gum/bite issues) is what actually fixes it long-term.
What Your Dentist Checks: Exam, X-Rays, Gum Assessment, Bite and Crack Testing
Your dentist follows a systematic diagnostic process to identify the exact source of sensitivity because different causes require completely different treatments. Surface-level assessment often misses the underlying structural problems.
Standard sensitivity examination includes:
Visual examination: Looking for visible wear patterns, recession, cavities, old fillings, cracks, and enamel defects. Your dentist checks the gum line carefully where enamel meets exposed root.
X-rays (radiographs): Revealing decay between teeth, bone loss around roots, and problems underneath existing fillings. X-rays show issues not visible during visual inspection.
Gum measurement: Probing pocket depths around each tooth to assess recession and bone loss. Measurements deeper than 3 millimeters suggest periodontal disease contributing to root exposure.
Percussion testing: Tapping teeth with an instrument to identify inflammation or infection in the nerve. Painful percussion response often indicates the tooth needs root canal treatment rather than simple sensitivity management.
Cold testing: Applying controlled cold to identify which specific teeth react and how quickly pain resolves. Normal sensitivity resolves within 5 seconds; prolonged response suggests nerve damage.
Bite testing: Having you bite on different points to locate cracks or high spots on fillings. Cracked teeth often show pain only when you release the biting pressure rather than during the initial bite.
Transillumination: Shining bright light through the tooth to make cracks visible. Cracks appear as dark lines interrupting the light transmission.
This complete examination takes 15 to 20 minutes at BrightSmile Dental Clinic in Putalisadak and helps us develop a treatment plan that addresses your specific cause rather than providing temporary symptom relief.
In-Clinic Desensitizers: Fluoride Varnish, Sealants, Dentin Bonding Agents
Professional desensitizing treatments apply concentrated protective materials directly to exposed dentin, providing immediate relief that lasts 3 to 6 months per application. These treatments work significantly faster than over-the-counter products because of higher concentration and professional application technique.
Fluoride varnish (22,600 ppm):
- Painted directly onto sensitive areas
- Sets in contact with saliva; stays in place 4 to 6 hours
- Provides immediate mineral boost to weakened enamel
- Reduces sensitivity within 24 to 48 hours
- Cost in Kathmandu: typically NPR 1,500 to 2,500 per application
Dental sealants:
- Thin resin coating that physically seals exposed tubules
- Applied to root surfaces with recession
- Lasts 1 to 2 years before wearing away
- Works best for isolated sensitive spots
- Cost in Kathmandu: approximately NPR 1,000 to 1,500 per tooth
Dentin bonding agents:
- Professional-grade resin that penetrates and seals tubules
- Creates waterproof barrier against all triggers
- Most durable option (2+ years)
- Requires tooth surface preparation for good adhesion
- Cost in Kathmandu: typically NPR 2,000 to 3,500 per tooth
Glutaraldehyde-based desensitizers:
- Chemical treatment that coagulates proteins inside tubules
- Blocks fluid movement that causes pain
- Provides relief within minutes of application
- Effects last 3 to 6 months
- Cost in Kathmandu: approximately NPR 1,500 to 2,000 per application
Most patients at our clinic in Putalisadak start with fluoride varnish because it addresses multiple teeth efficiently and costs less than bonding individual teeth. We recommend bonding or sealants for persistent sensitivity in specific teeth that did not improve adequately with varnish alone.
Professional treatments work best combined with home desensitizing toothpaste. The in-clinic treatment provides immediate relief while the daily toothpaste maintains and extends the protective effect.
Restorations That Stop Sensitivity: Fillings/Bonding/Crowns for Decay, Wear, or Cracks
Structural dental problems require structural solutions, surface treatments cannot fix cavities, significant enamel loss, or cracked teeth. These conditions need restoration to rebuild tooth anatomy and eliminate the pathway allowing triggers to reach the nerve.
Composite bonding for wear and minor defects:
- Tooth-colored resin material applied to worn areas
- Rebuilds lost enamel at gum line (abrasion lesions)
- Single-visit treatment requiring no anesthesia usually
- Lasts 3 to 5 years before needing replacement
- Cost in Kathmandu: NPR 3,000 to 6,000 per tooth depending on size
Fillings for cavities and leaking old restorations:
- Removes decay completely before filling
- Seals tooth structure from bacteria and temperature changes
- Eliminates sensitivity within days as nerve inflammation resolves
- Cost in Kathmandu: NPR 3,000 to 8,000 depending on cavity size and location
Crowns (caps) for extensive wear, large cracks, or failed fillings:
- Covers entire visible tooth portion
- Provides complete protection and structural reinforcement
- Required when decay or damage involves more than 40% to 50% of tooth structure
- Typically needs 2 visits (preparation, then crown placement)
- Cost in Kathmandu: NPR 15,000 to 35,000 depending on material (metal-ceramic vs full ceramic)
Root canal treatment for cracks reaching the nerve:
- Removes inflamed or infected nerve tissue
- Followed by crown to prevent further crack propagation
- Only option when crack extends into the pulp chamber
- Cost in Kathmandu: NPR 9,800 to 16,000 for RCT plus crown cost
The restoration type depends on how much tooth structure remains healthy. Your dentist at BrightSmile Dental Clinic evaluates whether bonding suffices or whether crown coverage is necessary for long-term success.
Sensitivity from structural problems does not respond to desensitizing toothpaste alone. You may notice temporary mild improvement, but the underlying defect continues worsening until you get proper restoration.
Gum Solutions and Bite Protection: Gum Treatment/Graft Options and Night Guards for Grinding
Gum recession requires different treatment approaches depending on severity and cause. Mild recession (1 to 2 millimeters) responds to improved home care and desensitizing treatments, while severe recession (3+ millimeters) may need gum grafting to restore coverage and eliminate sensitivity permanently.
Non-surgical gum treatment:
- Deep cleaning (scaling and root planing) to remove calculus below gum line
- Improves gum health and stops progressive recession
- Combined with proper brushing technique modification
- Cost in Kathmandu: NPR 8,000 to 15,000 for full-mouth treatment
Gum graft surgery:
- Takes tissue from palate or uses donor material
- Covers exposed roots surgically
- Provides permanent solution for severe recession
- Heals in 2 to 4 weeks
- Cost in Kathmandu: NPR 15,000 to 30,000 per tooth depending on technique
Pinhole surgical technique (minimally invasive):
- Advances existing gum tissue over exposed roots without cutting
- Faster healing than traditional grafts
- Limited availability in Kathmandu currently
- Cost where available: typically 20% to 30% higher than traditional grafts
Night guards for grinding protection:
- Custom-fitted acrylic appliance worn during sleep
- Prevents tooth-to-tooth contact that causes wear and cracks
- Reduces grinding force transmitted to tooth structure
- Requires 1 to 2 weeks adjustment period
- Lasts 2 to 5 years with proper care
- Cost in Kathmandu: NPR 8,000 to 15,000 for custom guard
Over-the-counter guards (boil-and-bite type) cost only NPR 1,500 to 3,000 but provide poor fit and protection compared to custom guards. The loose fit allows continued grinding damage and often falls out during sleep.
We evaluate grinding damage at BrightSmile Dental Clinic by checking for flat biting surfaces, small chips at tooth edges, and jaw muscle tenderness. Most grinders benefit from a night guard to prevent future sensitivity and structural damage even after we treat existing sensitivity.
Gum grafts eliminate root sensitivity permanently by restoring the protective tissue coverage. Patients who qualify for grafting typically see complete sensitivity resolution within 6 to 8 weeks after healing completes.
When to See a Dentist in Kathmandu and Prevention Plan
If your tooth sensitivity is mild and improving with sensitivity toothpaste, gentle brushing, and avoiding triggers, you can monitor it for about 2–4 weeks. For anything beyond that, seeking dental in Kathmandu means getting a proper diagnosis before the problem deepens. But book a dental visit sooner if the pain is getting worse, lasts after the hot/cold stimulus is gone, is limited to one tooth, or comes with swelling, fever, a bad taste, or pain that wakes you up, these can signal decay, a crack, or infection. For prevention, use a soft brush with light pressure, wait after acidic foods before brushing, reduce frequent acidic snacks/drinks, keep fluoride in your routine, and consider a night guard if you clench or grind.
Red Flags: Lingering Pain After Cold, Swelling, Fever, Bad Taste, Pain Waking You Up
Certain sensitivity patterns indicate dental emergencies requiring immediate professional care rather than home treatment. These red flags suggest infection, abscess, or severe nerve damage that worsens rapidly without intervention.
Seek same-day dental care if you experience:
- Lingering pain (30+ minutes) after cold exposure: Suggests irreversible pulpitis (dying nerve) that will not heal on its own. The tooth typically needs root canal treatment within days to prevent abscess formation.
- Swelling in gum or face near sensitive tooth: Indicates active infection spreading from tooth into surrounding tissues. Dental abscesses require drainage and antibiotics; they do not resolve with desensitizing products.
- Fever combined with tooth pain: Suggests systemic spread of dental infection. This constitutes a medical emergency requiring immediate care.
- Bad taste or odor from one tooth: Points to necrotic (dead) nerve tissue or pus drainage from an abscess. The infection source must be removed through root canal or extraction.
- Pain that wakes you from sleep: Spontaneous pain unrelated to triggers indicates severe nerve inflammation or infection. This pattern rarely improves without professional treatment.
- Sensitivity increasing in intensity over days: Progressive worsening suggests advancing decay, deepening crack, or worsening infection rather than simple dentin exposure.
BrightSmile Dental Clinic in Putalisadak provides same-day emergency appointments for patients experiencing these warning signs. You can reach us at +977-9748343015 for immediate consultation when symptoms suggest urgent problems.
Most genuine dental emergencies benefit from early treatment. Waiting often allows simple problems to escalate into situations requiring more extensive and expensive treatment.
When It’s Only One Tooth: When to Suspect Deep Decay/Crack (Don’t Self-Treat Too Long)
Single-tooth sensitivity persisting beyond 2 weeks of home treatment typically indicates a structural problem requiring professional diagnosis and restoration. General sensitivity affects multiple teeth because enamel wear and gum recession occur gradually across your entire mouth, not on just one tooth.
Patterns suggesting single-tooth pathology:
- Sensitivity started suddenly rather than gradually: Indicates specific incident like crack formation, filling failure, or cavity reaching dentin layer.
- One tooth reacts differently from others to the same trigger: Points to localized problem rather than generalized enamel thinning.
- Sensitivity appeared after biting something hard: Suggests crack that may not be visible but allows fluid movement inside the tooth.
- The sensitive tooth had previous dental work: Old fillings fail over time, creating gaps that allow temperature and bacteria penetration.
- You can see or feel a defect: Visible cavity, crack, or rough filling edge.
Attempting home treatment beyond 2 weeks for single-tooth sensitivity delays necessary care and allows the underlying problem to worsen. Cracks propagate deeper, decay spreads, and mild nerve inflammation progresses to infection.
Schedule examination within 1 week if:
- Home desensitizing products show zero improvement after 2 weeks
- Sensitivity intensity increases despite consistent product use
- The tooth develops new symptoms (pain on biting, swelling, changed color)
- You notice visible damage or changes to the tooth
BrightSmile Dental Clinic uses diagnostic imaging and clinical testing to identify the exact cause. Treatment often involves straightforward restoration (filling or bonding) when caught early, avoiding need for more complex procedures later.
What to Expect at a Kathmandu Dental Clinic: Same-Day Relief Options and Follow-Up Care
Your first visit at BrightSmile Dental Clinic in Putalisadak typically includes comprehensive examination, diagnosis, and initial treatment, many patients leave with immediate relief even on the first appointment. We prioritize same-day solutions whenever clinically appropriate.
Standard first-visit process:
- Consultation (10 to 15 minutes): Discussion of your symptoms, triggers, duration, and what you have tried already. We review medical history and medications that might contribute to sensitivity.
- Clinical examination (15 to 20 minutes): Visual inspection, X-rays if needed, gum measurements, and testing to identify sensitivity sources. We explain findings as we examine.
- Treatment options discussion: We present 2 to 3 suitable treatment approaches with realistic timelines and costs in Kathmandu price ranges. You choose the option matching your needs and budget.
Same-day treatment (when appropriate):
- Fluoride varnish application: immediate (15 minutes)
- Desensitizing bonding: immediate to 30 minutes per tooth
- Simple fillings: usually same-day if time permits (45 to 60 minutes)
- Night guard impressions: same-day; guard ready in 3 to 5 days
Treatment requiring follow-up visits:
- Crowns: 2 visits spaced 5 to 7 days apart
- Gum grafts: separate surgical appointment after planning
- Root canals: may complete in 1 or 2 visits depending on infection
We provide detailed home care instructions including:
- Specific products to use between visits
- Triggers to avoid during treatment period
- Signs that require immediate callback
- Timeline for improvement
Follow-up care at BrightSmile Dental Clinic includes:
- Check appointment 1 to 2 weeks after initial treatment
- Evaluation of symptom improvement
- Additional treatment if needed
- Long-term prevention strategies
Our location in Putalisadak makes us accessible from major areas of Kathmandu including Durbar Marg, Thamel, Kamaladi, and Dhobidhara. Most patients schedule follow-up visits during lunch break or after work (we accommodate evening appointments).
Contact us at brightsmileclinic33@gmail.com or +977-9748343015 to schedule consultation if your sensitivity persists despite 2 weeks of home treatment.
Prevention Checklist: Acid-Smart Eating, Brushing Timing, Fluoride Routine, and Grinding Control
Preventing sensitivity requires addressing all contributors simultaneously rather than focusing on just one factor. This comprehensive approach stops new sensitivity from developing and prevents treated sensitivity from returning.
Acid-smart eating habits:
- Limit lemon water to once daily; rinse with plain water afterward
- Drink acidic beverages through a straw positioned past your front teeth
- Consume acidic foods as part of meals rather than alone (saliva flow during meals helps neutralize)
- Wait 30 to 60 minutes after acidic exposure before brushing
- End meals with cheese or milk (calcium helps neutralize acid and remineralize)
Optimal brushing protocol:
- Use soft or extra-soft bristle brush exclusively
- Hold brush with light fingertip grip, not fist
- Brush 2 minutes, twice daily (morning and night)
- Replace brush every 2 to 3 months or when bristles fray
- Brush before breakfast if you consume acidic breakfast items, or wait 60 minutes after eating
Fluoride routine for prevention:
- Use fluoride toothpaste (1000 to 1450 ppm) twice daily
- Spit but do not rinse after brushing (leaves protective fluoride film)
- Apply sensitivity toothpaste to vulnerable spots at bedtime
- Consider fluoride mouth rinse if your dentist recommends it for high acid exposure
Grinding control strategies:
- Wear custom night guard consistently (every night, not just occasionally)
- Manage stress through exercise, meditation, or counseling
- Avoid chewing gum, hard foods, and ice
- Notice daytime clenching and consciously relax jaw
- Position tongue between teeth during day to prevent unconscious clenching
Additional prevention measures:
- Schedule dental cleanings every 6 months
- Address new cavities promptly before they cause sensitivity
- Replace old fillings showing wear or leakage
- Treat gum disease early to prevent recession progression
- Stay hydrated (dry mouth increases cavity and sensitivity risk)
Prevention checklist for Kathmandu patients:
Daily tasks:
- Brush with soft brush and sensitivity toothpaste morning and night
- Wait 60 minutes after acidic foods before brushing
- Drink water after meals and snacks
Weekly awareness:
- Check for new sensitive spots
- Evaluate whether night guard needs adjustment
- Notice grinding or clenching patterns
Every 6 months:
- Professional cleaning and examination at BrightSmile Dental Clinic
- Fluoride varnish application if you have active sensitivity or high risk
- Update X-rays to catch problems early
As needed:
- Replace toothbrush when bristles fray
- Schedule appointment if new sensitivity develops
- Adjust diet if you notice increased sensitivity after specific foods
Following this prevention plan reduces your sensitivity risk by 60% to 70% according to dental research. The combination approach addresses causes more effectively than any single intervention alone.
Patients at our Putalisadak clinic receive personalized prevention plans based on their specific risk factors and past dental history. Schedule your next preventive visit by calling +977-9748343015 or emailing brightsmileclinic33@gmail.com.
BrightSmile Dental Clinic provides comprehensive sensitivity diagnosis and treatment in Putalisadak, Kathmandu. Our comfort-first approach combines modern techniques with transparent pricing. Call +977-9748343015 to schedule your consultation.
Why are my teeth suddenly sensitive to cold and hot?
Sudden tooth sensitivity to cold and hot often results from worn enamel or gum recession exposing the roots. Whitening, dental cleanings, or harsh toothpaste can trigger it. If one tooth is affected, a cavity or crack is likely. Persistent or sharp pain requires a dental exam to identify the cause.
Is sensitive teeth a sign of a cavity?
Sensitive teeth can signal a cavity, especially if pain occurs in one area and worsens with sweets or chewing. Cavities may start with brief cold sensitivity and progress to lingering pain. Signs like visible holes, bad taste, or food trapping need dental evaluation and X-rays to confirm decay.
Why does cold hurt more than hot for sensitive teeth?
Cold hurts more because it causes rapid fluid movement in dentin tubules, triggering sharp pain. Hot also causes pain if the tooth nerve is inflamed. Lingering heat pain may signal nerve damage. Persistent or delayed hot pain should be examined by a dentist to rule out deep pulp issues.
How long does sensitivity toothpaste take to work?
Sensitivity toothpaste usually works within 1–2 weeks, with full relief in up to 4 weeks. Use it twice daily and apply directly to sensitive areas for faster results. If there’s no improvement after 2–4 weeks, a dentist should evaluate for underlying causes like cavities or gum issues.
Which toothpaste ingredient is best for sensitive teeth?
Potassium nitrate, stannous fluoride, arginine, and hydroxyapatite are effective ingredients for sensitive teeth. The best choice depends on the cause—erosion, exposed roots, or brushing damage. If you also have cavities, fluoride-based formulas are preferred. Dentists may recommend high-fluoride products or apply protective varnish in severe cases.
Should I stop brushing if brushing hurts my sensitive teeth?
Do not stop brushing if your teeth are sensitive. Instead, switch to a soft-bristled brush, use light pressure, and avoid scrubbing near the gums. Rinse with lukewarm water and use sensitivity toothpaste. If pain or bleeding continues, get a dental evaluation for gum inflammation or recession.
Can teeth sensitivity go away on its own?
Teeth sensitivity may go away if caused by temporary irritation, like whitening or cleaning. It usually improves within days to two weeks. But if it stems from enamel loss, cavities, or gum recession, it won’t resolve without treatment. Ongoing or worsening sensitivity needs a dental check.
Why are my teeth sensitive after a cleaning or scaling?
Sensitivity after cleaning or scaling occurs when inflamed gums shrink and expose sensitive areas. Tartar removal may uncover roots previously covered. This pain usually fades in a few days to two weeks. Use sensitivity toothpaste and avoid extreme temperatures during healing. If pain persists, seek a dental check.
When is tooth sensitivity an emergency?
Tooth sensitivity is an emergency if it’s accompanied by swelling, fever, pus, bad taste, or difficulty swallowing. Lingering pain after heat, night pain, or sudden severe pain may indicate nerve infection or abscess. Seek urgent dental care if symptoms escalate or spread.
What’s the best way to prevent sensitive teeth from coming back?
Prevent sensitive teeth by brushing gently with a soft brush, avoiding acidic foods before brushing, and limiting acidic drinks. Use fluoride toothpaste and treat grinding with a night guard. Regular checkups help detect gum recession, small cracks, and early cavities before sensitivity returns.
