Tooth damage happens suddenly; you bite into something hard, feel a sharp crack, and immediately wonder how serious it is. The difference between a chipped, cracked, or broken tooth determines whether you need same-day emergency care or can wait for a routine appointment within 48 hours. Understanding these distinctions helps you respond appropriately, protect your tooth from worsening damage, and avoid unnecessary panic or dangerous delays.
Chipped teeth involve small enamel fragments breaking away, cracked teeth have invisible fracture lines that cause bite pain, and broken teeth mean large pieces have separated with possible nerve exposure. Each type produces different symptoms, requires specific treatments, and carries varying risks if ignored, from minor cosmetic concerns to serious infections requiring root canal therapy or extraction. This guide explains exactly what happened to your tooth, what symptoms to watch for, and what steps to take right now to save your tooth and prevent complications.
Chipped vs Cracked vs Broken Tooth
A chipped tooth involves a small piece of enamel breaking off, creating a rough edge you can feel with your tongue. A cracked tooth has an invisible fracture line running through the tooth structure, causing sharp pain when you bite or release pressure. A broken tooth means a large fragment has separated, often exposing the yellow dentin layer or red pulp, and typically requires immediate dental attention.
Quick Comparison Table: How It Looks, How It Feels, and How Urgent It Is
Understanding the three main types of tooth damage helps you decide your next step.
| Type | What You See | What You Feel | Urgency Level |
| Chipped | Small piece of enamel missing, rough edge, usually visible on front teeth | Mild sensitivity to cold, tongue catches on sharp edge | Low to medium (24–48 hours unless severe pain) |
| Cracked | Often invisible to eye, may see faint line under bright light | Sharp pain when biting down or releasing bite, intermittent discomfort | Medium to high (within 24 hours; cracks worsen with time) |
| Broken | Large fragment missing, visible dentin (yellowish) or red pulp, sometimes entire crown gone | Immediate pain, bleeding, extreme sensitivity, difficulty eating | High to emergency (same day, especially if bleeding persists or pulp exposed) |
This table gives you a starting point. The sections below explain each condition in detail so you can identify what happened to your tooth.
What a Chipped Tooth Usually Means (Enamel Piece Off) and When It Is Minor
A chipped tooth means a small fragment of enamel, your tooth’s outermost protective layer, has broken away. Chips commonly occur on front teeth (incisors and canines) after minor impacts, such as hitting your tooth on a glass or biting something hard unexpectedly.
You notice a chipped tooth when your tongue keeps touching a rough or jagged edge. The missing piece is typically small, and the damage rarely extends beyond enamel. Most chips are minor if the dentin (the yellowish layer beneath enamel) is not exposed and you experience little to no pain.
When a chip is minor, you can wait 24 to 48 hours for a dental appointment. Your dentist will smooth the sharp edge or apply a small filling to restore the contour. The treatment is quick, usually painless, and prevents further damage or irritation to your tongue and cheek.
However, a chip is not always minor. It becomes urgent if you see yellow dentin, feel sharp pain, or notice sensitivity that interferes with eating. Large chips that expose deeper layers require prompt attention to prevent infection.
What a Cracked Tooth Means (Often Hurts on Biting/Release) and Why It Can Worsen

A cracked tooth has a fracture line that runs through the enamel and often into the dentin, though you rarely see it with the naked eye. Cracks are treacherous because they often remain invisible until you feel pain, usually a sharp, sudden jolt when you bite down or when you release the bite.
Cracks are different from chips. Chips involve a piece breaking off, while cracks involve a split that stays within the tooth structure. The fracture line acts like a fault line in an earthquake zone: every time you chew, the crack opens slightly, allowing saliva, bacteria, and food particles to seep deeper into the tooth.
You experience pain on biting or releasing pressure because the crack flexes. The flexing irritates the nerve inside the tooth, especially when the crack reaches the dentin. Cold liquids, sweet foods, or even cold air can trigger sharp, fleeting discomfort.
Cracks worsen over time. Chewing pressure, temperature changes, and natural tooth flexion cause the fracture to propagate deeper. A shallow crack that starts in enamel can extend through dentin and eventually reach the pulp (the nerve chamber). Once the pulp is involved, you need root canal treatment. If the crack extends below the gum line or splits the tooth vertically, extraction may be the only option.
Ignoring a cracked tooth is risky. What feels like minor, intermittent pain today can become constant, severe pain within weeks. Dentists in Kathmandu often see patients with advanced cracks that could have been saved with early crown placement. Cracks are time-sensitive: the earlier you treat them, the better the outcome.
The 5 Dentist Terms You Will Hear: Craze Lines, Fractured Cusp, Cracked Tooth, Split Tooth, Vertical Root Fracture
Dentists classify cracks and fractures into five categories. Knowing these terms helps you understand your diagnosis and treatment options.
- Craze lines are tiny, superficial cracks in enamel that look like hairline fractures. They are common in adults and do not cause pain or compromise tooth structure. Craze lines are cosmetic concerns only. Your dentist may polish them out or leave them untreated.
- Fractured cusp occurs when a piece of the chewing surface breaks off, usually around a filling. You feel a sudden change in how your tooth fits when you bite, and you may notice a rough or sharp edge. Fractured cusps rarely involve the nerve, so pain is mild or absent. Your dentist restores the tooth with a filling or crown.
- Cracked tooth is the most common serious fracture. The crack runs from the chewing surface downward, often stopping before it reaches the gum line. Cracked teeth cause pain on biting or release and sensitivity to temperature. Treatment depends on depth: shallow cracks get a crown; deeper cracks that reach the pulp require root canal therapy followed by a crown.
- Split tooth is the result of an untreated cracked tooth. The crack has extended fully through the tooth, dividing it into separate segments. Split teeth cannot be saved in most cases. Your dentist will extract the tooth and discuss replacement options such as implants or bridges.
- Vertical root fracture starts in the root and travels upward toward the chewing surface. These fractures are rare and usually affect teeth that have had root canal treatment. Symptoms include pain, swelling, and gum infection around the affected tooth. Vertical root fractures almost always require extraction because the crack is too deep to repair.
Understanding these terms empowers you during consultations. You know what your dentist means when they say “fractured cusp” versus “split tooth,” and you understand why treatment recommendations differ.
How Deep the Damage Goes (and What Can Happen If You Ignore It)
The depth of tooth damage determines both your symptoms and treatment urgency, enamel chips cause minor discomfort, dentin cracks trigger sensitivity and bite pain, and pulp exposure creates severe throbbing pain. Cracks spread deeper over time because chewing pressure and temperature changes cause the fracture line to widen, eventually reaching the nerve chamber. Ignoring tooth damage allows bacteria to enter through the fracture, leading to pulp infection, abscess formation, facial swelling, and potential tooth loss within weeks or months.
Tooth Layers Explained: Enamel vs Dentin vs Pulp (Why Deeper Damage Hurts More)
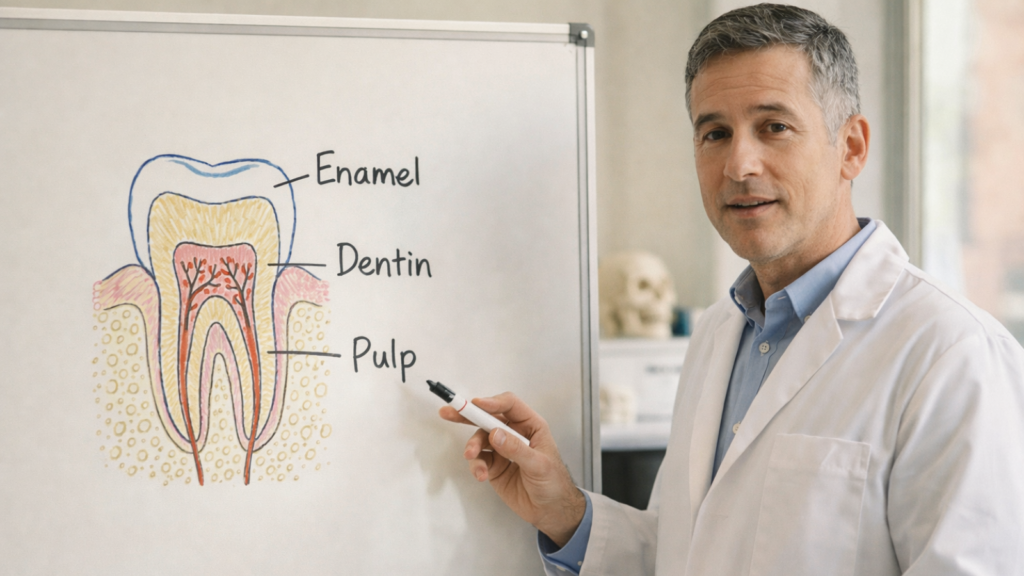
Your tooth has three layers: enamel, dentin, and pulp. Each layer has a different function, and damage to deeper layers produces more severe symptoms.
- Enamel is the outermost layer and the hardest substance in your body. It protects the tooth from decay, temperature changes, and biting forces. Enamel has no living cells and no nerve endings, so damage limited to enamel causes little to no pain. Chips and craze lines confined to enamel are minor issues.
- Dentin sits beneath enamel and makes up the bulk of your tooth structure. Dentin is softer than enamel and contains microscopic tubules that connect to the nerve chamber. Damage to dentin triggers sensitivity and pain because stimuli (cold, hot, sweet, pressure) travel through these tubules to the nerve. Cracked teeth that reach dentin hurt when you bite, and broken teeth that expose dentin cause sharp, persistent discomfort.
- Pulp is the innermost layer and contains nerves, blood vessels, and connective tissue. The pulp keeps your tooth alive by supplying nutrients and sensory feedback. Damage that reaches the pulp causes severe, throbbing pain, especially at night. Exposed pulp bleeds and is extremely sensitive to air, liquids, and touch. Pulp exposure requires immediate treatment to prevent infection and save the tooth.
Deeper damage hurts more because nerves become directly involved. Enamel damage is a cosmetic or structural concern. Dentin damage introduces pain signals. Pulp damage creates unbearable discomfort and risk of abscess. The depth of the fracture determines urgency and treatment complexity.
Why Cracks Spread: Biting Pressure, Temperature Changes, and “Invisible” Fractures
Cracks spread because teeth flex under normal use, and fractures create weak points that amplify this flexion. Three main forces drive crack propagation: biting pressure, temperature changes, and the invisible nature of fractures.
- Biting pressure is the primary driver. Every time you chew, your teeth experience hundreds of pounds of force. A cracked tooth flexes more than an intact tooth because the fracture line allows slight movement between the two sides of the crack. This repeated flexing widens the crack over time, like bending a paperclip back and forth until it breaks.
- Temperature changes exacerbate crack propagation. Hot foods and drinks cause your tooth to expand slightly, while cold items cause contraction. Enamel and dentin expand and contract at different rates, and the fracture line becomes a stress point where these differential movements concentrate. Over weeks and months, thermal cycling deepens the crack.
- Invisible fractures are dangerous because you do not see them, so you do not modify your behavior. You continue chewing on the cracked tooth, drinking cold beverages, and grinding your teeth at night. The crack silently extends deeper until it reaches the pulp or splits the tooth entirely. Many patients are shocked to learn their tooth is cracked because they see nothing wrong in the mirror.
Cracks rarely stay stable. They progress from enamel into dentin, from dentin into pulp, and from above the gum line to below it. The progression can take weeks or years, but the endpoint is predictable: untreated cracks eventually compromise the tooth beyond repair.
If Untreated: Infection, Abscess, Swelling, and Why It Can Become an Emergency
Untreated tooth damage leads to infection, and infection can become a dental emergency. The progression follows a predictable path: bacteria enter the tooth through the fracture, the pulp becomes infected, the infection spreads to surrounding bone, and an abscess forms.
- Firstly, bacteria colonize the fracture line. Saliva, food debris, and plaque accumulate in the crack, providing a pathway for bacteria to reach dentin and eventually pulp.
- Secondly, the pulp becomes inflamed and infected. You experience throbbing pain, sensitivity to hot temperatures, and pain that worsens at night.
- Thirdly, the infection spreads beyond the tooth into the surrounding bone, forming a pus-filled pocket called tooth abscess.
An abscess is serious. You develop facial swelling, fever, difficulty swallowing, and severe pain that radiates to your jaw, ear, or neck. The swelling can spread rapidly, and in rare cases, the infection can enter your bloodstream, causing sepsis, a life-threatening condition.
Untreated abscesses require emergency care. Your dentist will drain the abscess, prescribe antibiotics, and perform root canal treatment or extraction. Delaying treatment turns a manageable crack into a medical emergency that requires hospitalization in severe cases.
Infections are preventable. Treating a cracked tooth early, before bacteria reach the pulp, stops the progression. A crown placed on a cracked tooth seals the fracture, prevents bacterial invasion, and preserves the nerve. Ignoring the crack allows infection to develop, transforming a straightforward restoration into a complex emergency.
Which Teeth Are at Higher Risk (Molars, Heavily Filled Teeth, Root-Canal Teeth)
Certain teeth are more prone to cracking and breaking because of their location, structure, or previous dental work. Understanding which teeth are vulnerable helps you take preventive measures.
- Molars (back teeth) are at highest risk. Molars bear the greatest chewing forces and have deep grooves that concentrate stress. The second molars, in particular, crack frequently because they receive intense pressure during grinding and chewing. Dentists in Kathmandu commonly see cracked molars in patients who chew hard foods, grind their teeth at night, or have large fillings in these teeth.
- Heavily filled teeth have compromised structural integrity. Large fillings remove significant tooth structure, leaving thin walls of enamel that flex under pressure. These thin walls are prone to fracturing, especially around the edges of the filling. Teeth with fillings that cover more than half the chewing surface are at high risk for cusp fractures.
- Root-canal teeth are more brittle than living teeth because root canal treatment removes the pulp, eliminating the tooth’s blood supply and moisture. Over time, root-canal teeth become desiccated and less flexible. They crack more easily under normal biting forces. This is why dentists recommend placing crowns on root-canal teeth, the crown distributes chewing forces evenly and protects the brittle tooth from fracturing.
- Aging teeth also crack more often. Enamel naturally wears down with age, and decades of chewing create microscopic cracks that accumulate. Older patients experience cracked teeth more frequently, even without obvious trauma.
Preventive strategies for high-risk teeth include wearing a night guard if you grind, avoiding hard foods (bones, ice, nuts), replacing old large fillings with crowns before they fracture, and placing crowns on root-canal teeth immediately after treatment. These measures reduce your risk of serious fractures.
Common Causes and Risk Factors
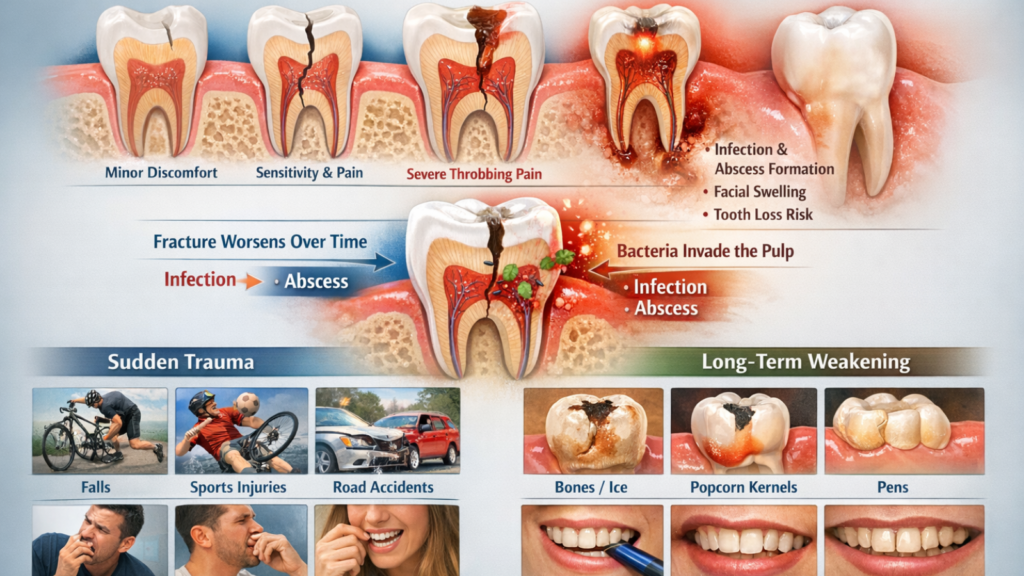
The depth of tooth damage determines both your symptoms and treatment urgency, enamel chips cause minor discomfort, dentin cracks trigger sensitivity and bite pain, and pulp exposure creates severe throbbing pain. Cracks spread deeper over time because chewing pressure and temperature changes cause the fracture line to widen, eventually reaching the nerve chamber. Ignoring tooth damage allows bacteria to enter through the fracture, leading to pulp infection, abscess formation, facial swelling, and potential tooth loss within weeks or months.
Sudden Trauma: Falls, Sports Injuries, Road Accidents, and Hits to the Mouth
Sudden trauma is the most obvious cause of chipped, cracked, or broken teeth. Falls, sports injuries, and road accidents generate high-impact forces that exceed your tooth’s structural limits.
- Falls are common in Kathmandu, especially during the monsoon season when streets and staircases become slippery. Tripping and hitting your face on pavement, stairs, or furniture can chip or break front teeth instantly. Children and elderly individuals are particularly vulnerable because they have slower reflexes and less ability to protect their face during a fall.
- Sports injuries occur frequently in contact sports such as football, basketball, and martial arts. A blow to the face from a ball, elbow, or opponent’s head can fracture multiple teeth. Athletes who play without mouthguards face significantly higher risk. Even non-contact sports like cycling can result in dental trauma if you crash and hit your face on handlebars or the ground.
- Road accidents, including motorcycle crashes and pedestrian collisions, cause severe dental injuries. High-speed impacts often break teeth at the root level or knock teeth out entirely. Accident victims who suffer facial injuries should see a dentist immediately, even if dental damage seems minor initially, hidden fractures may not become apparent for days or weeks.
- Hits to the mouth from domestic accidents, workplace injuries, or altercations also cause sudden tooth damage. Closing a car door on your face, getting hit by a swinging object, or being struck during an argument can chip, crack, or break teeth.
Sudden trauma requires immediate dental evaluation. Your dentist will assess not only visible damage but also hidden fractures, jaw alignment, and nerve integrity. X-rays reveal cracks and bone involvement that you cannot see in the mirror.
Hard Biting Triggers: Bones/Ice, Popcorn Kernels, Nuts, Pens, and Nail Biting

Biting hard objects is the most preventable cause of tooth damage. Your teeth are designed to chew food, not withstand the forces generated by biting ice, bones, or non-food items.
- Bones and ice are common culprits. Chewing goat meat bones (khasikomasuको हड्डी), frozen ice cubes, or hard candy exposes your teeth to extreme point loads. Enamel can withstand distributed chewing forces, but concentrated pressure on a single point creates microfractures that accumulate into visible cracks. Molars with large fillings are especially vulnerable because the filling material is weaker than natural tooth structure.
- Popcorn kernels cause unexpected damage because they are small, hard, and easily hidden among soft popcorn. Biting down on an unpopped kernel generates intense localized force that can fracture a cusp or create a vertical crack. Patients in Kathmandu who enjoy popcorn during movies should chew carefully and avoid forcing kernels between teeth.
- Nuts and hard-shelled foods such as walnuts, supari (betel nut), and peanut shells damage teeth over time. Repeatedly cracking shells with your teeth wears down enamel and creates stress fractures. Supari, in particular, hardens with age and places tremendous stress on molars. Dentists in Nepal see many cracked molars in patients who chew supari regularly.
- Pens and nail biting are nervous habits that slowly weaken teeth. Chewing on pens, pencils, or fingernails subjects your front teeth to abnormal forces and increases crack risk. The damage is cumulative: each chewing session creates microscopic damage that eventually results in a visible chip or crack.
Avoiding hard biting triggers is simple but requires awareness. Use scissors or nutcrackers instead of teeth, spit out popcorn kernels, stop nail biting by keeping nails short, and choose soft snacks. These habits protect your teeth from preventable damage.
Long-Term Weakening: Cavities, Big Fillings, Bruxism (Grinding), and Age-Related Enamel Wear
Long-term weakening makes teeth vulnerable to damage under normal use. Unlike sudden trauma, long-term factors gradually reduce tooth strength until a routine action, eating bread, yawning, causes the tooth to crack or break.
- Cavities create weak spots by dissolving enamel and dentin. A tooth with untreated decay has less structural integrity and cracks more easily under chewing forces. Decay also softens dentin, allowing cracks to propagate faster. Treating cavities early prevents this weakening.
- Big fillings remove significant tooth structure to eliminate decay. The remaining tooth walls become thin and prone to fracture, especially when the filling is large and extends to the edges of the tooth. Composite and amalgam fillings are strong, but they do not flex like natural tooth structure. Over time, the interface between filling and tooth becomes a stress point where cracks initiate.
- Bruxism (teeth grinding) is a major risk factor for cracked teeth. Many people grind their teeth at night without realizing it, subjecting their teeth to hundreds of pounds of horizontal and vertical force for hours. Grinding wears down enamel, creates flat spots on chewing surfaces, and initiates cracks at the gum line or along existing fillings. Patients in Kathmandu who wake with jaw pain, headaches, or worn teeth should ask their dentist about bruxism and night guard use.
- Age-related enamel wear occurs naturally over decades. Years of chewing, temperature changes, and acid exposure gradually thin enamel and reduce its protective capacity. Older teeth are more brittle and less able to withstand sudden forces. This is why tooth fractures become more common after age 50.
Addressing long-term weakening involves replacing large fillings with crowns before they fracture, treating cavities promptly, using a night guard if you grind, and maintaining good oral hygiene to slow enamel erosion. Preventive care is more effective and less expensive than repairing broken teeth.
Symptoms Checklist: How to Tell the Difference at Home (Safely)
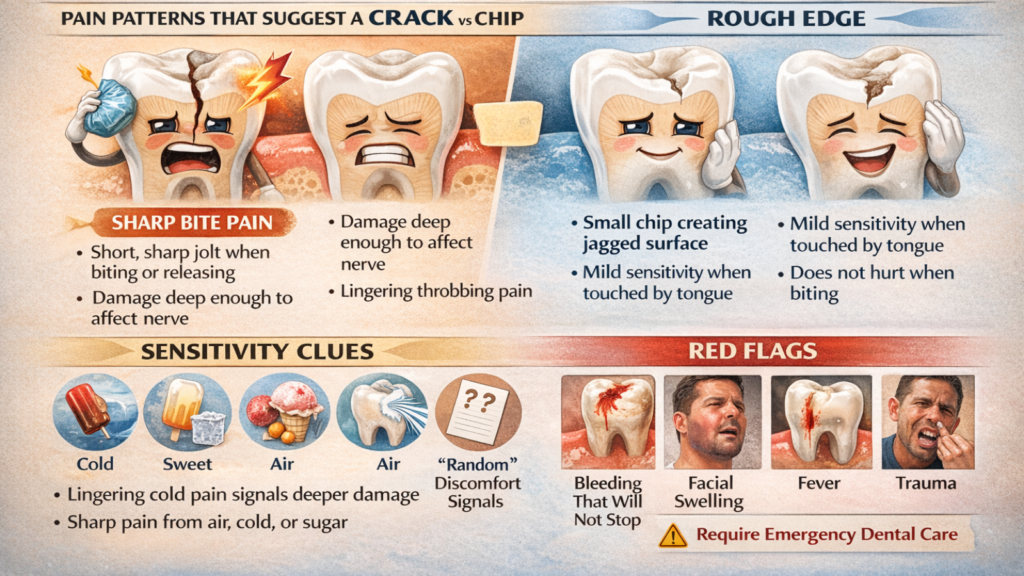
Pain patterns reveal the type and severity of tooth damage, sharp pain on biting or releasing suggests a crack, while a rough edge with mild sensitivity indicates a chip. Temperature sensitivity, especially lingering pain from cold or sharp discomfort from air, signals deeper damage involving dentin or pulp. Red flags such as persistent bleeding, facial swelling, fever, severe pain, or visible pulp exposure require same-day emergency dental care to prevent serious complications.
Pain Patterns That Suggest a Crack vs a Chip (Sharp Bite Pain vs Rough Edge)
Pain patterns help you distinguish between a crack and a chip before you see a dentist. Cracks and chips produce different sensations because they affect different tooth layers and structures.
Sharp bite pain is the hallmark of a cracked tooth. The pain occurs the instant you bite down on something or when you release the bite. It feels like a sudden jolt, stab, or electric shock. The pain disappears once you stop biting, but returns predictably when you chew on that side. This pattern occurs because the crack flexes when you apply pressure, irritating the nerve inside the tooth. The pain is sharp, fleeting, and localized to one tooth.
Rough edge is the primary symptom of a chipped tooth. Your tongue repeatedly touches a jagged or sharp edge where the enamel broke away. The sensation is annoying but rarely painful unless the chip is large enough to expose dentin. You may feel mild sensitivity to cold, but the discomfort is dull and continuous rather than sharp and bite-related. Chipped teeth do not hurt when you release a bite because there is no fracture line flexing under pressure.
Persistent aching suggests deeper involvement, possibly pulp exposure or infection. The pain is constant, throbbing, and worsens at night. It does not respond clearly to biting or releasing pressure. Persistent aching indicates a broken tooth with pulp exposure or an advanced crack that has infected the nerve.
Temperature sensitivity occurs in both cracks and chips but differs in quality. Cracked teeth produce sharp, fleeting pain when exposed to cold or hot liquids, and the pain lingers briefly after the stimulus is removed. Chipped teeth cause mild, dull sensitivity that resolves immediately once the cold or hot item is removed. If cold causes lingering, severe pain, the damage is deep.
Use these pain patterns to assess urgency at home. Sharp bite pain requires a dental visit within 24 hours because cracks worsen quickly. Rough edges from chips can wait 24 to 48 hours unless pain becomes severe. Persistent aching or extreme sensitivity demands same-day attention.
Sensitivity Clues: Cold, Sweet, Air Sensitivity, and “Random” Discomfort Signals
Sensitivity patterns reveal how deep the damage extends and whether the nerve is affected. Observing what triggers your discomfort helps you describe symptoms accurately to your dentist.
Sensitive teeth, specifically cold sensitivity, indicate dentin exposure.. Dentin tubules connect to the nerve, so cold liquids or air trigger sharp, brief pain. Mild cold sensitivity in a chipped tooth is normal and resolves after the dentist smooths the edge. Severe, lingering cold sensitivity in a cracked tooth suggests the crack has penetrated deeply toward the pulp. If cold sensitivity wakes you at night or prevents you from drinking water, the crack is serious.
Sweet sensitivity occurs when sugary foods contact exposed dentin. Sugar changes osmotic pressure in the dentin tubules, stimulating the nerve. Sweet sensitivity is less common than cold sensitivity but equally significant. It suggests dentin involvement and requires prompt treatment.
Air sensitivity is a red flag for pulp exposure. Breathing through your mouth causes sharp, intense pain in the affected tooth. Air sensitivity indicates the pulp is partially exposed or very close to the fracture line. This symptom requires same-day dental care.
Random discomfort signals are episodes of pain or sensitivity that seem to happen without clear triggers. The tooth aches unexpectedly, then stops. Random discomfort suggests a crack that opens and closes intermittently, irritating the nerve unpredictably. This pattern is common in cracked teeth because chewing pressure, jaw position, and temperature changes affect how much the crack flexes. Random discomfort is not a reason to delay treatment, it indicates active crack progression.
Document your sensitivity patterns before your appointment. Note what triggers pain, how long the pain lasts, and whether it is sharp or dull. This information helps your dentist diagnose the problem and plan treatment.
Same-Day vs Can-Wait Guidance: Who Needs a Dentist Today vs Within 24–48 Hours
Knowing when to seek immediate care versus scheduling a routine appointment protects your tooth and saves money. Delaying necessary treatment worsens outcomes; rushing to the dentist for minor chips wastes time and causes unnecessary anxiety.
Same-day dental visits are necessary if you experience any of these symptoms:
- Bleeding that continues for more than 10 minutes despite applying pressure
- Visible pulp exposure (red, bloody tissue inside the tooth)
- Severe pain that prevents you from sleeping, eating, or concentrating
- Facial swelling, especially near the jaw or under the eye
- Fever or pus discharge from the gum around the tooth
- Large broken piece with sharp edges cutting your tongue or cheek
- Tooth mobility (the tooth moves when touched)
- Trauma involving loss of consciousness or jaw misalignment
These symptoms indicate serious damage or infection that requires urgent intervention. Call your dentist immediately or visit an emergency dental clinic in Kathmandu such as BrightSmile Dental Clinic (+977-9748343015).
Appointments within 24 hours are appropriate if you experience:
- Sharp, fleeting pain when biting or releasing bite (suggests crack)
- Small chip with dentin exposure (yellowish layer visible)
- Mild to moderate sensitivity to cold or sweet
- Discomfort that interferes with eating but not sleeping
- Visible crack line or rough edge
These symptoms indicate damage that will worsen but is not immediately life-threatening. Schedule an appointment as soon as possible to prevent progression.
Appointments within 24 to 48 hours are acceptable if you have:
- Tiny chip confined to enamel with no pain
- Rough edge that bothers your tongue but no sensitivity
- Minor cosmetic concern on a front tooth
- Craze lines with no discomfort
These issues are minor and can wait a day or two. Do not delay beyond 48 hours, however, because even minor damage can worsen unexpectedly.
Use this guidance to prioritize your response. When in doubt, call your dentist’s office and describe your symptoms, they will advise whether you need same-day care.
Red Flags: Bleeding That Will Not Stop, Facial Swelling, Fever, Pus, Severe Pain, Trauma
Red flags indicate dental emergencies that require immediate professional intervention. These symptoms suggest complications such as infection, abscess, or severe trauma that can endanger your health if left untreated.
- Bleeding that will not stop after 10 to 15 minutes of applying pressure suggests significant soft tissue injury or damage to blood vessels inside the tooth. Persistent bleeding requires professional care to control the source and assess underlying damage.
- Facial swelling around the jaw, cheek, or under the eye indicates infection spreading beyond the tooth into surrounding tissues. Swelling that develops rapidly (within hours) or interferes with breathing or swallowing is a medical emergency. Severe facial infections can spread to the brain or bloodstream. Seek immediate care at a hospital or emergency dental clinic.
- Fever accompanying dental pain or swelling signals systemic infection. A fever above 38°C (100.4°F) combined with tooth pain suggests an abscess. Systemic infection requires antibiotics and urgent dental treatment.
- Pus discharge from the gum around a damaged tooth confirms abscess formation. Pus may taste bitter or foul and drain spontaneously when the abscess ruptures. Abscess drainage does not mean the infection is resolved, it indicates the infection has spread into bone. You need antibiotic therapy and root canal treatment or extraction.
- Severe pain that prevents sleep, eating, or normal activities requires same-day evaluation. Pain that worsens rapidly (over hours rather than days) suggests acute pulpitis or abscess formation. Delaying treatment allows the infection to spread and increases the risk of tooth loss.
- Trauma involving loss of consciousness, jaw misalignment, or difficulty opening your mouth suggests fractures of the jaw or facial bones in addition to tooth damage. These injuries require imaging (CT scan or X-ray) and multidisciplinary care involving oral surgeons and emergency physicians. Go to a hospital emergency department immediately.
Red flags are your body’s warning system. Do not ignore them or attempt home remedies. Professional care is necessary to resolve these emergencies safely.
How Dentists Diagnose It (and Why X-Rays Do Not Always Show Cracks)
Dentists diagnose tooth damage through clinical examination including bite tests, tapping, gum evaluation, and mobility checks before ordering imaging. X-rays miss most cracks because fracture lines are hairline-thin and oriented vertically, but they reveal important information such as decay, bone loss, and infection signs around the tooth. Advanced tools such as magnification, dye staining, transillumination, and wedging tests confirm crack location and depth when clinical findings are inconclusive.
What Dentists Check First: Bite Test, Tapping, Gum Evaluation, and Mobility
Dentists use a systematic clinical examination to diagnose tooth damage before ordering imaging. The initial exam identifies symptoms and narrows down the diagnosis, guiding further testing.
- Bite test is the first diagnostic step for suspected cracks. Your dentist gives you a small plastic or rubber wedge (called a Tooth Slooth or Fractfinder) to bite on different parts of the tooth. You bite down and release. If you feel sharp pain on biting or releasing over one specific cusp, the test is positive for a crack beneath that cusp. The bite test isolates the cracked segment and predicts where the fracture runs.
- Tapping (percussion test) involves tapping the tooth gently with a dental instrument. A cracked or infected tooth feels more tender to tapping than healthy adjacent teeth. Increased tenderness suggests inflammation around the root tip, which occurs when cracks extend deep or when infection is present.
- Gum evaluation checks for swelling, redness, pus, or abnormal pockets around the tooth. Infection from a cracked tooth causes localized gum inflammation. Your dentist probes around the tooth to measure pocket depth. Deep, isolated pockets (7–10 mm) suggest a vertical crack extending below the gum line, a poor prognostic sign.
- Mobility test assesses whether the tooth moves when pushed. Healthy teeth have minimal mobility. Increased mobility suggests a split tooth, vertical root fracture, or severe bone loss from infection. Mobile teeth often require extraction because the supporting structures are compromised.
These clinical tests take only a few minutes but provide critical diagnostic information. Many dentists diagnose cracked teeth based entirely on clinical findings because imaging often misses cracks.
Why X-Rays Miss Cracks (and What They Can Reveal: Decay, Bone Loss, Infection Signs)
X-rays are essential for diagnosing tooth damage, but they rarely show cracks directly. Understanding what X-rays can and cannot reveal helps you interpret your dentist’s findings.
X-rays miss cracks because fractures are hairline-thin and oriented vertically through the tooth. Standard dental X-rays show horizontal slices, so vertical cracks are invisible unless they run parallel to the X-ray beam, a rare alignment. Most cracks run from the chewing surface downward at oblique angles that X-rays cannot capture.
What X-rays reveal instead:
- Firstly, decay around old fillings weakens tooth structure and increases crack risk. X-rays show dark areas indicating decay beneath or adjacent to fillings.
- Secondly, bone loss around the tooth suggests chronic infection from an undetected crack. Cracks allow bacteria to reach the root, causing bone resorption visible on X-rays.
- Thirdly, widened periodontal ligament space appears as a dark halo around the root tip. This widening indicates inflammation and infection, common sequelae of cracked teeth.
- Fourthly, root fractures occasionally appear on X-rays as radiolucent (dark) lines running through the root. These are easier to see than coronal (crown) cracks because root fractures often separate bone around them.
Your dentist uses X-rays to rule out decay, assess bone health, and identify complications from cracks rather than to visualize the crack itself. Clinical examination remains the gold standard for crack detection.
Confirmation Tools: Magnification, Dye, Transillumination (Light Test), Wedging/Segment Testing
Advanced diagnostic tools help dentists confirm crack location, depth, and extent when clinical examination and X-rays are inconclusive. These tools are especially useful for diagnosing hairline cracks that cause symptoms but are not visible to the naked eye.
Magnification (dental loupes or microscopes) allows dentists to examine tooth surfaces at 3× to 20× magnification. Fine crack lines invisible without magnification become apparent under magnified view. Dentists look for irregular lines, stained fissures, and subtle fractures along filling margins.
Dye application makes cracks visible by staining them. Your dentist dries the tooth, applies a colored dye (often blue or purple) to the chewing surface, rinses it away, and examines the tooth under magnification. Dye seeps into crack lines and remains visible after rinsing, revealing the crack’s location and extent. This technique is simple, quick, and effective for confirming suspected cracks.
Transillumination (light test) shines bright light through the tooth from different angles. Healthy enamel transmits light evenly. Cracks block light transmission, appearing as dark lines or shadows. The dentist holds a fiber-optic light behind or beside the tooth and looks for interrupted light patterns. Transillumination is particularly useful for anterior (front) teeth where cracks are harder to see clinically.
Wedging and segment testing applies controlled pressure to suspected crack segments. Your dentist places a wedge or rubber dam clamp on one side of the tooth and asks you to bite down. If the separated segments cause sharp pain when flexed, the test confirms a crack. This technique predicts crack direction and helps determine whether the tooth is still restorable.
These tools complement clinical examination and X-rays. Your dentist may use one or several techniques to achieve an accurate diagnosis before recommending treatment.
Prognosis & “Saveability”: When Bonding/Crown Works vs When Root Canal/Extraction Is Likely
Prognosis depends on crack depth, location, and extent. Not all cracked or broken teeth are saveable. Your dentist evaluates several factors to determine whether restoration is feasible or extraction is necessary.
Favorable prognosis (bonding, filling, or crown) applies to:
- Chips limited to enamel with no dentin exposure → smooth and bond, or place a small filling
- Small cracks confined to enamel or shallow dentin with no symptoms → place a crown to prevent progression
- Fractured cusp with no nerve involvement → remove the fractured segment, place a filling or onlay, and crown if needed
- Cracked tooth that does not extend below the gum line and responds normally to cold → crown to stabilize the tooth
These cases have high success rates (85–95%) because the structural damage is limited and the nerve is healthy.
Guarded prognosis (root canal and crown) applies to:
- Cracked tooth with pain on biting, cold sensitivity, and suspected pulp involvement → perform root canal to remove infected nerve, then crown
- Large break exposing pulp → root canal to clean the nerve chamber, then crown
- Cracked tooth with intermittent pain that has not yet caused abscess → root canal and crown prevents future infection
Root canal treatment has an 80–90% success rate if the crack does not extend below the gum line.
Poor prognosis (extraction) applies to:
- Split tooth with the crack extending fully through the tooth → no treatment can reunite the segments; extraction is necessary
- Vertical root fracture → the crack runs through the root, making the tooth unsaveable
- Crack extending below the gum line into the bone → insufficient remaining tooth structure to support a restoration
- Severe mobility indicating bone loss → extraction and replacement with implant or bridge
Your dentist will explain prognosis clearly during consultation. If extraction is necessary, discuss replacement options (implant, bridge, partial denture) immediately to prevent adjacent teeth from shifting.
What to Do Now: First Aid, Treatment Options, Costs, and Prevention (Kathmandu Context)
Immediate first aid includes rinsing with warm water, controlling bleeding with gauze pressure, taking ibuprofen for pain, and saving any broken fragments in milk or saliva. Treatment options range from simple bonding for small chips (NPR 3,000–6,000) to crowns for cracks (NPR 10,000–25,000) and root canal therapy for pulp involvement (NPR 9,800–16,000), with specific recommendations depending on damage depth and location. Contact BrightSmile Dental Clinic in Putalisadak (+977-9748343015) for same-day emergency appointments, transparent pricing, and comprehensive care tailored to Kathmandu patients.
First Aid Right Now: Rinse, Control Bleeding, Reduce Pain, and Save the Broken Piece Properly
Immediate first aid reduces pain, prevents infection, and preserves treatment options. Take these steps as soon as damage occurs.
- Rinse your mouth with warm water to remove blood, food debris, and broken fragments. Gentle rinsing cleans the area without causing additional trauma. Do not use mouthwash containing alcohol, as it stings broken tissue.
- Control bleeding by applying gentle pressure with clean gauze or a damp tea bag to the bleeding site. Bite down on the gauze for 10 minutes without checking. Tea bags contain tannic acid, which promotes clotting. If bleeding continues after 15 minutes of pressure, seek immediate dental care.
- Reduce pain with over-the-counter pain relievers. Ibuprofen (400 mg every 6 hours) reduces pain and inflammation. Paracetamol (500–1000 mg every 6 hours) is an alternative if you cannot take ibuprofen. Apply a cold compress to your cheek for 15 minutes to reduce swelling and numb the area. Do not place aspirin directly on the tooth or gum, it burns tissue.
- Save the broken piece by placing it in a clean container with milk, saline solution, or your saliva. Do not let the fragment dry out. Bring it to your dental appointment, dentists can sometimes reattach large fragments with bonding material.
Do not panic. Most tooth damage is treatable. Follow these first aid steps, and contact your dentist as soon as possible.
Temporary Protection While You Wait: Cover Sharp Edges, Soft Diet, Chewing Rules, Sleeping Tips
Temporary protection prevents worsening damage and reduces discomfort until you see your dentist. These measures are safe and effective for short-term use (24–48 hours).
Cover sharp edges with dental wax (available at pharmacies) or sugar-free chewing gum. Soften the wax or gum in your hands, press it gently over the sharp edge, and smooth it out. This barrier protects your tongue and cheek from cuts. Replace the wax or gum after eating. Do not use regular chewing gum, it contains sugar that increases infection risk.
Follow a soft diet until you see your dentist. Eat soft foods such as daal-bhaat (soft rice and lentils), yogurt, mashed potatoes, soup, smoothies, and scrambled eggs. Avoid hard, crunchy, sticky, or chewy foods such as meat, raw vegetables, chips, and sweets. Soft foods reduce chewing pressure on the damaged tooth.
Chewing rules minimize stress on the injured tooth. Chew on the opposite side of your mouth. Cut food into small pieces so you do not bite down forcefully. Avoid opening your mouth wide, which can shift jaw position and flex the cracked tooth.
Sleeping tips reduce nighttime pain and protect the tooth. Sleep with your head elevated on two pillows to reduce blood flow to the injured area and decrease throbbing. Take pain reliever 30 minutes before bed. If you grind your teeth, avoid sleeping on the side of the damaged tooth, sleep on your back or the opposite side.
These temporary measures keep you comfortable and safe until professional treatment. Do not delay your dental appointment, temporary protection is not a substitute for definitive treatment.
What NOT to Do: DIY Glues, Chewing on That Side, Very Hot/Cold Foods, Delaying with Swelling
Avoiding common mistakes prevents complications and protects your tooth. Patients often make these errors thinking they are helping, but they cause harm.
Do not use DIY glues such as superglue, epoxy, or craft adhesive to reattach broken pieces. These products contain toxic chemicals, do not bond to wet tooth surfaces, and prevent proper dental repair. Superglue also generates heat during curing, which can burn gum tissue. Only dentists use biocompatible dental adhesives designed for oral use.
Do not chew on that side of your mouth. Biting down on a cracked or broken tooth worsens the damage, spreads the fracture deeper, and increases pain. Even if the tooth feels stable, chewing on it risks splitting the tooth completely.
Avoid very hot or cold foods and drinks. Extreme temperatures cause the tooth to expand and contract, worsening cracks and triggering severe pain. Drink room-temperature water, avoid ice cream and hot tea, and let hot foods cool before eating.
Do not delay treatment if you have facial swelling. Swelling indicates infection spreading beyond the tooth. Delaying treatment allows the infection to worsen, increases the risk of systemic complications, and may result in tooth loss or hospitalization. Swelling is an emergency, seek care immediately.
Other mistakes to avoid include taking aspirin and placing it directly on the tooth (it burns tissue), ignoring pain because “it comes and goes” (intermittent pain means progressive damage), and assuming small chips do not need treatment (small chips can hide deeper cracks).
Following these guidelines protects your tooth and ensures the best treatment outcome.
Treatment Options by Type: Bonding/Filling/Onlay/Crown/Veneer vs Root Canal (What Decides)
Treatment depends on damage type, depth, and tooth location. Your dentist selects the most conservative option that restores function, prevents complications, and lasts long-term.
Bonding repairs small chips in front teeth. Your dentist applies tooth-colored composite resin to the chipped area, shapes it to match the original contour, and hardens it with a curing light. Bonding takes 30–60 minutes, requires no anesthesia, and costs NPR 3,000–6,000 per tooth in Kathmandu. Bonding is ideal for minor enamel chips with no dentin exposure.
Fillings restore chips and fractured cusps in back teeth. Your dentist removes any decay, shapes the cavity, and places composite or amalgam filling material. Fillings cost NPR 2,000–5,000 depending on material and size. Fillings work well for small to moderate damage confined to enamel and shallow dentin.
Onlays are partial crowns that cover one or more cusps without covering the entire tooth. Onlays preserve more natural tooth structure than full crowns and are ideal for fractured cusps or large fillings with remaining healthy tooth walls. Onlays cost NPR 8,000–15,000 in Kathmandu.
Dental Crowns cover the entire tooth, protecting it from further damage and restoring full function. Crowns are necessary for cracked teeth, large breaks, heavily filled teeth, and root-canal teeth. The dentist removes a thin layer of enamel, takes an impression, and places a temporary crown. The permanent crown (porcelain, zirconia, or metal) is cemented 1–2 weeks later. Crowns cost NPR 10,000–25,000 depending on material.
Veneers are thin porcelain shells bonded to the front surface of teeth. Veneers restore appearance after chips or breaks in front teeth. They cost NPR 15,000–30,000 per tooth and are cosmetic options for patients who want aesthetic perfection.
Root canal and crown is necessary when the crack or break exposes the pulp or when the nerve is infected. Your dentist removes the infected pulp, cleans and shapes the root canals, fills them with biocompatible material, and places a crown to protect the brittle root-canal tooth. Root canal treatment costs NPR 9,800–16,000 in Kathmandu; adding a crown brings the total to NPR 20,000–40,000.
Read more about veneer and crown
What decides the treatment?
- Depth: Enamel-only damage → bonding or filling; dentin involvement → filling or crown; pulp involvement → root canal and crown
- Location: Front teeth → bonding or veneer for aesthetics; back teeth → crown for strength
- Extent: Small chip → bonding; large break or crack → crown; split tooth → extraction
- Symptoms: No pain → conservative restoration; pain on biting → crown; severe pain → root canal and crown
Your dentist will explain options, show you photos or models, and discuss costs transparently. BrightSmile Dental Clinic in Putalisadak offers comprehensive consultations with clear pricing (NPR 500–1,000 consultation fee, deductible from treatment if you proceed within 30 days). Call +977-9748343015 or visit our clinic to discuss your treatment plan.
Key Takeaways
- Chipped, cracked, and broken teeth differ in appearance, symptoms, and urgency. Chips remove small enamel pieces and cause rough edges. Cracks create invisible fracture lines that hurt on biting. Breaks involve large fragments and often expose dentin or pulp.
- Symptoms guide urgency. Sharp bite pain, bleeding, swelling, fever, or pulp exposure require same-day care. Small chips and craze lines can wait 24–48 hours. Use the pain patterns and red flags in this guide to assess your situation.
- Early treatment prevents complications. Untreated cracks spread, leading to infection, abscess, and tooth loss. Crowns placed early stop crack progression. Root canal treatment saves teeth with infected nerves. Extraction is necessary only when cracks extend below the gum line or split the tooth.
- First aid and temporary protection keep you comfortable until you see your dentist. Rinse, control bleeding, take pain relievers, cover sharp edges with dental wax, and eat soft foods. Avoid DIY glues, chewing on the damaged side, and delaying treatment if you have swelling.
- Treatment options range from simple bonding to root canal and crown. Your dentist selects the best option based on damage depth, location, and symptoms. Costs in Kathmandu range from NPR 3,000 for bonding to NPR 40,000 for root canal and crown.
If you have a chipped, cracked, or broken tooth, contact BrightSmile Dental Clinic in Putalisadak for best broken tooth treatment services. Our team provides transparent pricing, same-day emergency appointments, and gentle treatment in a comfortable environment. Call +977-9748343015 or message us on WhatsApp to schedule your consultation today.
Can a cracked tooth heal on its own?
A cracked tooth cannot heal on its own because enamel and dentin do not contain living cells to regenerate. Without treatment, the crack deepens over time, potentially reaching the nerve and requiring root canal or extraction. Early intervention with a crown prevents further damage and saves the tooth.
How much does it cost to fix a chipped tooth in Kathmandu?
Fixing a chipped tooth in Kathmandu costs NPR 3,000–6,000 for bonding, NPR 2,000–5,000 for fillings, NPR 15,000–30,000 for veneers, and NPR 10,000–25,000 for crowns. Prices vary by damage severity and material used.
Is a cracked tooth an emergency?
A cracked tooth is an emergency if it causes severe pain, swelling, fever, bleeding, or pulp exposure. Moderate cracks with bite pain need care within 24 hours. Minor enamel cracks can wait 24–48 hours but still require evaluation.
What happens if I ignore a small chip?
Ignoring a small chip allows bacteria to collect and cracks to worsen. The tooth weakens over time, increasing fracture risk. Dentists recommend evaluating most chips within 48 hours, even if painless.
Why does my cracked tooth only hurt sometimes?
A cracked tooth hurts intermittently because the fracture flexes during biting or temperature changes, irritating the nerve. The pain signals active crack progression and requires treatment before it reaches the pulp.
Can dentists see cracks on X-rays?
Dentists usually cannot see cracks on standard X-rays because fracture lines are too thin and vertical. They rely on bite tests, dyes, magnification, and transillumination. X-rays help detect bone loss or infection, not the crack itself.
Should I get a crown or root canal for my cracked tooth?
Get a crown if the crack is shallow and confined to enamel or dentin. A root canal is needed if the crack reaches the pulp or causes nerve pain. Dentists base treatment on symptoms and diagnostic tools.
What should I eat with a broken tooth while waiting for my appointment?
Eat soft foods like daal-bhaat, yogurt, soup, scrambled eggs, and mashed potatoes on the opposite side of your mouth. Avoid hard, sticky, or hot foods to reduce pain and damage. Cut food into small pieces.
How long can I wait to fix a chipped front tooth?
You can wait 24–48 hours to fix a painless cosmetic chip, but delaying over a week increases infection risk and enamel wear. If dentin or pulp is exposed, get treatment within 24 hours.
Are cracked molars more common than cracked front teeth?
Yes, cracked molars are more common because they endure higher chewing forces and have deep grooves that trap stress. Front teeth chip more often due to direct impacts but rarely crack from biting.
