Losing one or more teeth affects far more than just your smile. Chewing becomes difficult, neighboring teeth shift out of position, and jawbone begins to deteriorate over time. Many dental patients in Kathmandu wonder whether dental implants offer the right solution for their situation. Understanding eligibility requirements, necessary diagnostic tests, and medical factors helps you determine candidacy before scheduling consultations.
Dental implants provide permanent tooth replacement that looks, feels, and functions like natural teeth. However, not everyone qualifies immediately for this treatment. Your overall health status, jawbone condition, gum health, lifestyle habits, and commitment to oral care all influence success rates. This comprehensive guide explains candidacy criteria, preparatory treatments that may be needed, and long-term care requirements you must know before making informed decisions about implant placement.
Understanding Dental Implant Candidacy: Who Can Get Implants?
Dental implants serve as artificial tooth roots placed into jawbone to support replacement teeth. Most healthy adults who have lost one or more teeth qualify for this treatment. Successful implant placement depends on sufficient bone density, healthy gums, and overall physical wellness that supports proper healing.
What Makes Someone a Good Candidate for Dental Implants?

Several factors determine implant candidacy. Firstly, adequate jawbone volume and density provide stable anchoring for titanium posts; secondly, healthy gum tissue free from active infection supports integration; thirdly, commitment to maintaining excellent oral hygiene ensures long-term success. Patients must have completed jaw growth, which typically occurs in late teens or early twenties. Well-controlled chronic conditions rarely prevent treatment, but unmanaged health issues require stabilization before proceeding.
Things that make a good candidate:
- Completed jaw growth (late teens or older)
- Healthy gums free from active disease
- Sufficient bone density and volume
- Well-managed chronic health conditions
- Non-smoker or willing to quit tobacco
- Commitment to excellent oral hygiene
Non-smokers generally experience higher success rates than tobacco users. Smoking restricts blood flow, slows healing, and increases failure risk significantly. Quitting tobacco several weeks before surgery greatly improves outcomes and reduces complications.
Common Absolute and Relative Contraindications (When Implants Aren’t Recommended)
Absolute contraindications prevent implant placement entirely. Severe, uncontrolled diabetes with poor wound healing makes surgery unsafe. Active cancer treatment involving radiation to jaw areas damages bone and prevents proper integration. Severe immunodeficiency disorders compromise healing capacity beyond acceptable limits.
Relative contraindications require careful evaluation but don’t automatically disqualify candidates. Controlled diabetes with stable blood sugar levels allows safe treatment. Mild to moderate osteoporosis may need medication adjustment or bone grafting. Bruxism (teeth grinding) necessitates protective nightguards to prevent excessive force on implants.
Patients taking bisphosphonates for osteoporosis face increased risk of jaw complications. Anticoagulant medications require coordination with physicians to manage bleeding risk during surgery. Each case receives individual assessment to weigh benefits against potential complications.
Age, Maturity and Growth Considerations (Teens vs Adults)
Jaw development must be complete before implant placement. Girls typically finish facial growth around ages 16 to 18. Boys continue developing until ages 18 to 21. Placing implants prematurely can lead to misalignment as surrounding bone continues growing.
Young adults who lost permanent teeth often wait until skeletal maturity. Temporary solutions like removable partial dentures bridge gaps during this waiting period. Once growth completes, permanent implant placement proceeds safely.
No upper age limit exists for implant candidates. Seniors in their seventies, eighties, and beyond successfully receive implants. Health status matters more than chronological age. Adequate bone quality, manageable medical conditions, and ability to maintain oral hygiene determine suitability regardless of years.
How Your Dentist Decides: Consultation Checklist
Comprehensive evaluation begins with detailed medical and dental history review. Dentists ask about current medications, chronic conditions, previous surgeries, and lifestyle habits. Physical examination assesses existing teeth, gum health, bite alignment, and visible bone structure.
Imaging studies provide crucial information about bone quality and quantity. Digital X-rays reveal bone levels, tooth roots, and hidden pathology. Three-dimensional CBCT scans measure precise bone dimensions, locate nerves and sinuses, and identify anatomical limitations.
Specialists collaborate when complex cases require additional expertise. Periodontists evaluate and treat gum disease before implant placement. Oral surgeons handle bone grafting, sinus lifts, and difficult extractions. Physicians provide medical clearance for patients with significant health conditions.
Medical & Lifestyle Factors That Affect Your Candidacy

General health status significantly influences implant success rates. Chronic conditions, medications, and daily habits all impact healing capacity. Understanding these factors helps dentists create safe, effective treatment plans tailored to individual circumstances.
Chronic Medical Conditions That Matter (Diabetes, Osteoporosis, Autoimmune Disorders)
Diabetes affects wound healing and infection resistance. Well-controlled diabetes (HbA1c below 7%) poses minimal additional risk. Uncontrolled high blood sugar delays healing, increases infection rates, and reduces osseointegration (bone-implant fusion). Patients must stabilize glucose levels before surgery and maintain strict control throughout recovery.
Diabetes considerations:
- HbA1c below 7% indicates good control
- Uncontrolled diabetes delays healing
- Increased infection risk with high blood sugar
- Coordination with physician essential
Osteoporosis factors:
- Mild cases rarely prevent treatment
- Moderate to severe may need medication adjustment
- Bisphosphonate therapy requires careful evaluation
- Bone density testing may be necessary
Osteoporosis weakens bone density systemwide, including jaws. Mild osteoporosis rarely prevents implant placement. Moderate to severe cases may require bone density testing and medication adjustments. Bisphosphonate therapy (common osteoporosis treatment) carries risk of Osteonecrosis of the Jaw (ONJ), particularly with intravenous formulations.
Autoimmune disorders like rheumatoid arthritis, lupus, and Sjögren’s syndrome can impair healing. Immunosuppressant medications reduce infection-fighting capacity. Coordination between dental professionals and rheumatologists ensures safe timing for procedures and appropriate medication management during healing phases.
Medications and Special Cases (Bisphosphonates, Anticoagulants, Cancer Therapy)
- Bisphosphonates strengthen bones but can interfere with jaw healing. Oral bisphosphonates (pills) carry lower risk than intravenous versions. Dentists may recommend temporary discontinuation before surgery in consultation with prescribing physicians. Careful monitoring during healing detects early signs of complications.
- Anticoagulants (blood thinners) like warfarin or newer agents prevent clotting but increase surgical bleeding. Most patients continue medications with minor dosage adjustments. Procedures can proceed safely with proper precautions like hemostatic agents and careful technique. Stopping anticoagulants carries stroke or heart attack risk, so coordination with cardiologists ensures balanced management.
- Cancer therapy creates unique challenges. Radiation to head and neck areas damages blood supply and weakens bone structure. Chemotherapy suppresses immune function and slows healing. Dentists typically wait until treatment completion and recovery before considering implants. Some radiation patients require hyperbaric oxygen therapy to improve bone health before surgery.
Smoking, Alcohol, Nutrition and Lifestyle Effects on Success
Tobacco use dramatically reduces implant success rates. Nicotine constricts blood vessels, reducing oxygen delivery to healing tissues. Studies show smokers experience failure rates two to three times higher than non-smokers. Quitting at least eight weeks before surgery and maintaining abstinence throughout healing significantly improves outcomes.
Heavy alcohol consumption impairs immune function and interferes with bone metabolism. Moderate drinking doesn’t prevent treatment, but excessive use requires lifestyle modification. Alcohol also affects medication metabolism and can interact with pain medications or antibiotics prescribed during recovery.
Nutrition directly impacts healing capacity. Protein deficiency slows tissue repair. Vitamin D and calcium support bone integration. Vitamin C promotes collagen formation essential for gum healing. Well-nourished patients heal faster with fewer complications than those with dietary deficiencies.
Oral Health Factors: Gum Disease (Periodontitis), Infection, and Bruxism
Active periodontal disease must be controlled before implant placement. Bacteria causing gum infection can colonize implant surfaces, leading to peri-implantitis (gum disease around implants). Treatment includes deep cleaning (scaling and root planing), antimicrobial therapy, and sometimes gum surgery. Once infection clears and tissue stabilizes, implant placement proceeds safely.
Existing dental infections require resolution first. Abscesses, cavities, and failing root canals harbor bacteria that spread to surgical sites. Complete infection elimination through fillings, root canals, or extractions protects new implants from contamination.
Bruxism (teeth grinding) exerts excessive force on implants. Untreated grinding can loosen implants or fracture prosthetic components. Custom nightguards distribute forces evenly and protect both natural teeth and implants. Patients with severe bruxism may need additional implants to distribute load or specialized implant designs to withstand forces.
Tests & Pre-Operative Assessments: How Clinics Check You’re Ready
Thorough diagnostic evaluation determines candidacy and guides treatment planning. Modern dental technology provides detailed information about bone structure, anatomical limitations, and overall health status. Comprehensive assessment ensures safe procedures and predictable outcomes.
Clinical Dental Exam and Medical History Review: What to Bring
Initial consultations involve detailed discussions about health background. Bring current medication lists including dosages and prescribing doctors. Previous dental records help establish treatment history and identify past complications. Medical records documenting chronic conditions provide important context for risk assessment.
Physical examination evaluates oral structures systematically. Dentists check gum color, texture, and attachment levels. Probing around existing teeth measures pocket depths indicating periodontal health. Bite analysis reveals alignment issues or excessive forces. Soft tissue examination detects lesions, asymmetry, or signs of pathology.
Discussion covers expectations, concerns, and treatment preferences. Dentists explain procedures, timelines, and costs clearly. Open communication establishes trust and ensures realistic understanding of what treatment involves. Questions about recovery, temporary teeth, and long-term maintenance receive thorough answers.
Imaging Explained: Panoramic X-Ray, Periapical X-Rays, CBCT/CT and What Each Shows
Panoramic radiographs capture entire upper and lower jaws in single images. This imaging shows overall bone levels, remaining teeth, sinus positions, and nerve locations. Panoramic views help identify gross pathology and plan preliminary approaches.
Panoramic X-rays show:
- Overall jaw structure and bone levels
- Remaining tooth positions
- Sinus locations
- Major nerve pathways
CBCT scans reveal:
- Precise bone height and width measurements
- Three-dimensional nerve mapping
- Sinus proximity to potential implant sites
- Bone density variations
Periapical X-rays focus on specific tooth regions with high detail. These images reveal bone density, root structures, and localized infections. Periapical films guide precise measurements for individual implant sites.
Cone Beam Computed Tomography (CBCT) provides three-dimensional imaging essential for modern implant planning. CBCT scans measure bone height, width, and density in millimeters. Three-dimensional visualization maps critical structures like nerves, sinuses, and blood vessels. Software allows virtual implant placement before actual surgery, ensuring optimal positioning and angulation.
Lab Tests and Medical Clearance: When General Blood Tests or MD Clearance Are Needed
Routine blood work isn’t required for healthy patients undergoing straightforward implant placement. Complete Blood Count (CBC) may be ordered for patients with bleeding disorders or anemia. Coagulation studies (PT/INR) guide management for anticoagulated patients.
Patients with diabetes should have recent HbA1c results demonstrating glucose control. Values above 8% suggest poorly controlled diabetes requiring medical management before surgery. Bone density tests help assess osteoporosis severity in high-risk patients.
Medical clearance from physicians becomes necessary for complex health conditions. Cardiologists evaluate patients with heart disease or recent cardiac events. Endocrinologists help optimize diabetic control. Oncologists provide guidance for cancer patients regarding treatment timing and precautions.
Specialist Referrals: Periodontist, Oral Surgeon, or Physician Collaborations
Periodontists specialize in gum disease treatment and soft tissue management. Referral occurs when extensive periodontal therapy precedes implant placement. Periodontists also perform advanced bone grafting and manage complex aesthetic cases requiring gum contouring.
Oral surgeons handle surgical complications, difficult extractions, and extensive bone grafting. Patients needing sinus lifts, ridge augmentation, or multiple implants often receive care from oral surgeons. Surgical specialists manage medical emergencies and complex anatomical challenges.
General physicians coordinate care for medically compromised patients. Collaboration ensures medication adjustments, infection prophylaxis, and complication management align with overall health needs. Team approaches produce safer outcomes for high-risk candidates.
Preparatory Treatments and Alternatives If You’re Not Ready

Some candidates require preliminary procedures before receiving implants. Bone deficiencies, gum disease, and anatomical limitations often respond to preparatory treatments. Alternative options exist for patients who cannot undergo implant surgery.
Bone Grafting, Ridge Augmentation and Sinus Lift: When and Why They’re Used
Bone grafting rebuilds deficient jawbone using natural or synthetic materials. Autografts harvest bone from patient sites like chin or jaw angles. Allografts use processed donor bone from tissue banks. Synthetic materials include calcium phosphate or bioactive glass that stimulates new bone formation.
Ridge augmentation rebuilds width and height of collapsed bone ridges. Tooth loss causes bone resorption over time. Grafting restores dimensions necessary for implant stability. Healing typically requires four to six months before implant placement.
Sinus lifts create space for implants in upper back jaw regions. Maxillary sinuses naturally extend close to tooth roots. After tooth loss, inadequate vertical bone remains between sinus floor and ridge crest. Sinus membrane elevation and bone grafting underneath provide height for implant anchoring.
Treating Gum Disease and Infections Before Implant Placement
Periodontal therapy eliminates bacteria and inflammation compromising implant success. Scaling and root planing remove calculus (tartar) and infected tissue below gumlines. Antimicrobial rinses and antibiotics supplement mechanical cleaning.
Severe cases may require gum surgery. Flap procedures access deep pockets for thorough cleaning. Bone recontouring removes defects harboring bacteria. Guided tissue regeneration encourages new attachment of gums to teeth.
Infected teeth undergo appropriate treatment before implant surgery. Endodontic therapy (root canals) saves restorable teeth. Extractions remove hopeless teeth creating chronic infection sources. Healing periods allow complete tissue recovery before implant placement.
Non-Implant Options: Bridges, Removable Dentures, or Short-Term Provisional Solutions
Fixed dental bridges replace missing teeth by crowning adjacent natural teeth. Preparation involves reducing neighboring tooth structure. Bridges restore function and aesthetics but sacrifice healthy tooth structure. Lifespan averages 10 to 15 years before replacement becomes necessary.
Removable partial dentures clip onto remaining teeth. Acrylic and metal frameworks hold artificial teeth filling gaps. Partials offer affordable, non-surgical options. Daily removal for cleaning and potential discomfort during eating represent disadvantages.
Complete dentures replace all teeth in upper or lower arches. Suction and muscle control hold dentures in place. Modern dentures provide good aesthetics and basic function. Bone resorption continues under dentures, requiring periodic relining or replacement.
Implant-Supported Prosthesis Options (Single Crown vs Bridge vs Overdenture)
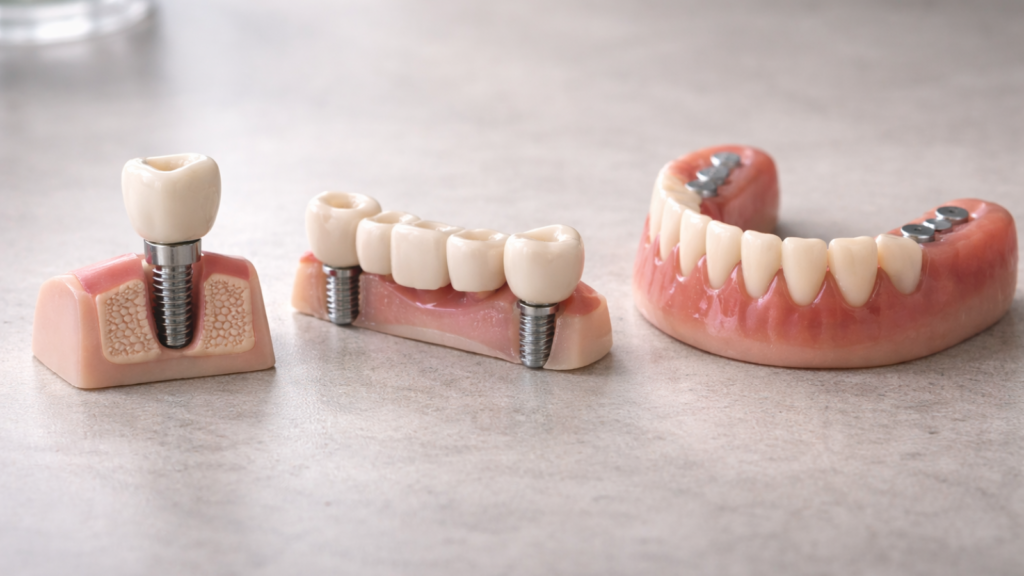
Single-tooth implants replace individual missing teeth independently. Titanium posts receive custom crowns matching surrounding natural teeth. Single implants preserve adjacent teeth and function like natural roots.
Implant-supported bridges replace multiple consecutive missing teeth. Two or more implants anchor fixed bridges spanning edentulous spaces. This approach eliminates need for complete dentures while providing stable chewing function.
Implant-retained overdentures combine benefits of implants and dentures. Two to four implants secure removable prosthetics with attachments. Overdentures provide superior stability compared to conventional dentures at lower cost than full fixed implant bridges; see dental implant vs bridges to compare which option fits your needs and budget.
Risks, Success Factors and Aftercare You Must Know
Understanding potential complications, success predictors, and maintenance requirements helps patients achieve optimal long-term results. Proper aftercare significantly influences implant longevity. Awareness of warning signs enables early intervention when problems arise.
Typical Success Rates and What Lowers Them
Modern dental implants demonstrate success rates exceeding 95% over 10 years when properly placed and maintained. Lower jaw implants typically succeed more often than upper jaw placements due to denser bone structure. Single-tooth replacements show slightly higher success than multiple-implant cases.
Several factors reduce success rates significantly. Smoking decreases success by 10 to 15 percentage points. Uncontrolled diabetes, poor oral hygiene, and untreated bruxism all increase failure risk. Inadequate bone volume without proper grafting leads to early loosening.
Implant surface characteristics and placement technique also affect outcomes. Immediate placement after extraction carries slightly higher risk than delayed placement in healed bone. Experienced surgeons working in well-equipped facilities achieve better results than less-experienced practitioners.
Peri-Implantitis and Infection: Signs, Prevention and Early Actions
Peri-implantitis resembles gum disease around natural teeth but affects implant supporting structures. Bacterial colonization triggers inflammation, bone loss, and potential implant failure. Early stages (peri-mucositis) involve gum inflammation without bone loss. Advanced peri-implantitis destroys supporting bone.
Warning signs include bleeding during brushing, gum redness, swelling around implant sites, and deepening pockets. Pus discharge or implant mobility indicate advanced infection requiring immediate attention. Regular dental visits detect early changes before significant damage occurs.
Prevention centers on excellent daily hygiene. Brushing twice daily with soft-bristle brushes cleans implant surfaces gently. Flossing or interdental brushes remove plaque from hard-to-reach areas. Professional cleanings every three to six months maintain gum health around implants. Here’s what happens during teeth cleanings so you know what to expect.
Post-Op Care: Immediate Recovery, Diet, Pain Control and Antibiotics
First 24 hours after surgery require careful management. Apply ice packs to reduce swelling. Avoid disturbing surgical sites with tongue or fingers. Sleep with head elevated to minimize swelling.
Recommended foods for first week:
- Yogurt and smoothies
- Scrambled eggs
- Mashed potatoes and vegetables
- Soups (lukewarm, not hot)
- Soft fish
- Protein shakes
Foods to avoid:
- Hot liquids
- Crunchy or hard foods
- Spicy dishes
- Alcoholic beverages
- Foods requiring vigorous chewing
Soft diet prevents excessive pressure on healing sites. Recommended foods include yogurt, smoothies, scrambled eggs, and mashed vegetables. Avoid hot liquids, crunchy foods, and anything requiring vigorous chewing for first week. Gradually reintroduce normal foods as comfort allows.
Pain management typically involves over-the-counter analgesics like paracetamol or ibuprofen. Dentists prescribe stronger medications when necessary. Antibiotics prevent infection in most cases. Complete entire prescribed course even when feeling better.
Long-Term Maintenance: Hygiene, Checks, and When Repairs Are Needed
Daily oral care maintains implant health for decades. Brush all surfaces thoroughly twice daily. Use low-abrasive toothpaste to avoid scratching implant surfaces. Floss or use specialized implant brushes between teeth and around crowns.
Professional maintenance visits every six months allow early problem detection. Dentists evaluate gum health, check prosthetic components, and take periodic X-rays monitoring bone levels. Professional cleaning removes calculus buildup preventing peri-implantitis.
For dental implant services contact BrightSmile Dental Clinic
Prosthetic repairs occasionally become necessary. Crowns can chip, break, or become loose. Retightening abutment screws solves most looseness issues. Crown replacement restores fractured restorations. Implant posts themselves rarely require replacement when properly maintained.
Can I get dental implants even though I have diabetes?
Patients with well-controlled diabetes can safely receive dental implants. Maintain an HbA1c below 7% to reduce infection risk and support bone healing. Stable blood sugar before surgery and during the 3–6 month healing phase significantly improves implant success rates.
How long must I wait after tooth extraction before getting implants?
The waiting period after tooth extraction ranges from immediate placement to four months. Most dentists place implants after 3–4 months, allowing complete bone healing when infection, bone quality, and extraction complexity are favorable.
Are dental implants painful to get?
Dental implant surgery is not painful due to local anesthesia. Patients typically experience mild discomfort for 3–7 days after surgery, similar to a tooth extraction. Over-the-counter pain medication effectively controls post-operative soreness.
What happens during CBCT scan and does radiation pose risks?
A CBCT scan takes 20–30 seconds while the patient remains still. Radiation exposure equals roughly 1–2 days of natural background radiation. The diagnostic accuracy significantly outweighs the minimal radiation risk.
Can smokers successfully get dental implants?
Smokers can receive dental implants, but failure rates are nearly double compared to non-smokers. Quitting smoking at least 8 weeks before surgery and remaining tobacco-free during healing greatly improves implant success.
How much bone loss is too much for implants?
No amount of bone loss automatically disqualifies implant placement. Procedures such as bone grafting, ridge augmentation, or sinus lifts rebuild deficient bone. CBCT imaging determines available bone volume and required preparation.
Do I need to see my medical doctor before implant surgery?
Patients with conditions such as heart disease, uncontrolled diabetes, or recent cancer treatment require physician clearance before implant surgery. Healthy individuals without systemic disease usually do not need medical consultation. You can contact our dental in Kathmandu to get consultation.
How soon can I eat normally after implant placement?
Patients follow a soft diet for the first 7 days after implant placement. Normal foods return gradually as comfort improves. Most patients resume a full diet within 2–3 weeks.
What makes peri-implantitis different from regular gum disease?
The main difference between peri-implantitis and gum disease is progression speed and structure. Peri-implantitis advances faster because implants lack a periodontal ligament, increasing the risk of rapid bone loss.
Can I replace all my teeth with implants in Kathmandu?
Kathmandu dental clinics offer full-arch implant solutions, including fixed bridges and implant-retained overdentures. Treatment planning evaluates bone quality, implant count, and total cost using CBCT diagnostics.
